Jarisch-Herxheimer reaction (JHR or ‘herx’) is an acute febrile reaction which may complicate the initiation of an effective treatment against infections due to intracellular microorganisms. JHR can also be expressed as the worsening of symptoms or the appearance of new symptoms. JHR is traditionally associated with antibiotics and antivirals but may appear from taking anything that impacts the immune response or infections.
When it comes to probiotics, the usual Herx pattern is different. With an antibiotics induced herx, the herx will usually start when the concentration of the antibiotic approaches it’s maximum concentration and then ease off as the antibiotic leaves the system. The pattern is illustrated below.
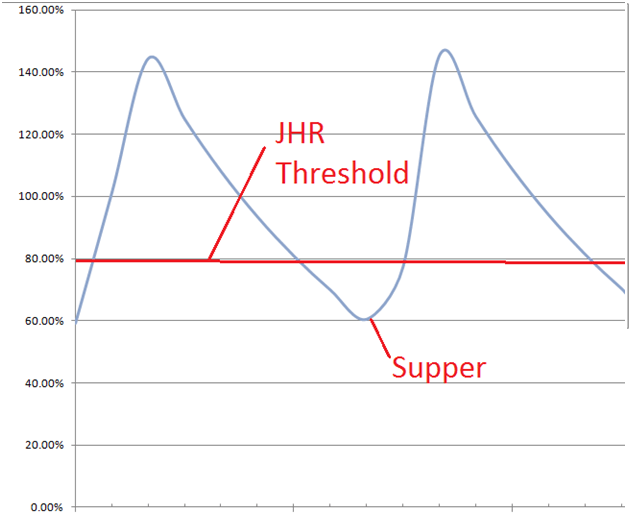
Example of tissue concentration from an antibiotic taken twice a day
With a biological agent, each probiotic capsule increases the amount of it’s species that is alive and living in the gut. Probiotics have friend-foe identification and produce ‘antibiotics’ against other species. When the population of the probiotics species reaches the JHR threshold (may be a week or more in some cases), then a herx may start from killing off foe-species. This is where the challenge begins in handling the herx. If the herx gets too severe, then stopping will not result in a quick ebbing (as happens with antibiotics), but may continue until one of two states are reached:
- Most of the foe-species producing the toxin causing the herx are killed, so there is insufficient toxins to produce a herx.
- The population of this probiotics is reduced / out-competed so it is not producing sufficient foe-antibiotics to create a herx.
The time to take this may be days…. the herx just keeps going and going…

