A reader forward Antimicrobial activities of widely consumed herbal teas, alone or in combination with antibiotics: an in vitro study[2017]
This study found “Of the 31 teas (24 different herbs and seven bag teas), as shown in Table S1, only 15 teas showed inhibition zones against one or more microorganisms in the disk diffusion assays, while the others: linden, lemon balm, hibiscus, rosemary, nettle, chamomile, bay, yarrow, eucalyptus, lavender, galangal, orange, sage, ginger, herb bennet, and echinacea teas did not show any activity.”
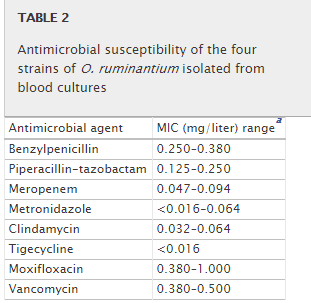
It then presents this lovely table. S. Aureus is a suspected maintainer of CFS(see post). The smaller the number, the less is needed.

Among the tables is one that suggests you need to have cups of teas every 8 hours and the effect may take up to 4 hrs, at least for rosehip tea bags. (RB)

Note, ” The combinations of herbal teas with antibiotics showed synergistic, additive, or antagonistic effects, depending on the antibiotic or type of tea. ” So if you are doing teas and antibiotics — you need to read this article in full. The tea may reduce the effect of the antibiotics (or increase it!).
- Highly antibiotic-resistant Acinetobacter baumannii clinical isolates are killed by the green tea polyphenol (-)-epigallocatechin-3-gallate (EGCG) [2009].
- Epigallocatechin gallate synergy with ampicillin/sulbactam against 28 clinical isolates of methicillin-resistant Staphylococcus aureus [2001].
- Synergistic interactions of epigallocatechin gallate and oxytetracycline against various drug resistant Staphylococcus aureus strains in vitro [2013].
- Inhibition of penicillinase by epigallocatechin gallate resulting in restoration of antibacterial activity of penicillin against penicillinase-producing Staphylococcus aureus [2002].
Bottom Line
Rosehip (Rosa canina) tea (and soup?) looks like a excellent item to take 3 times per day — assuming you are not taking E.Coli probiotics at the same time.
- “Among the tested bacteria, Pseudomonas aeruginosa and Salmonella typhimurium were the most susceptible to the activity of R. canina leaf extract with MIC and MBC values both 0.009 mg mL(-1). For most of the bacterial strains investigated the extract showed significantly higher activity compared to the used standard compounds streptomycin and ampicillin.“ [2015]
- In vivo anti-inflammatory effect of Rosa canina L. extract.[2011]
Rose hips contain the carotenoids beta-carotene, lutein, zeaxanthin and lycopene.
It has been used in some IBS Studies [2000] [2009]. A 2008 technical paper on rose hip is here.
“A rose hip preparation (not clear whether it was rose hip or rose hip and seed) was investigated in a randomized double-blind study including 60 patients suffering from irritable bowel syndrome. They started to register their intestinal complaints 2 weeks before the administration of the products by means of a questionnaire. Patients receiving the proprietary rose hip drink as placebo pro-fited less than those receiving additional Lactobacillus plantarum 9843, but abdominal pain was reduced in both groups (Nobaek et al., 2000). ”
According to WebMd:
“Rose hips are also used for stomach disorders including stomach spasms, stomach acid deficiency, preventing stomach irritation and ulcers, and as a “stomach tonic” for intestinal diseases. They are also used for diarrhea, constipation, gallstones, gallbladder ailments, lower urinary tract and kidney disorders, fluid retention (dropsy or edema), gout, back and leg pain (sciatica), diabetes, high cholesterol, weight loss, high blood pressure, chest ailments, fever, increasing immune function during exhaustion, increasing blood flow in the limbs, increasing urine flow and quenching thirst.”
We do not know a great deal about which bacteria it kills or encourages — so this is definitely an item for “the art of microbiome manipulation“.
Discuss with your medical professional trying 3 cups of tea (every 8 hrs) for a week and see if there is any significant change. Do not substitute “rose hip capsules” , you want actual tea (and yes, it is a bit of an acquired taste).

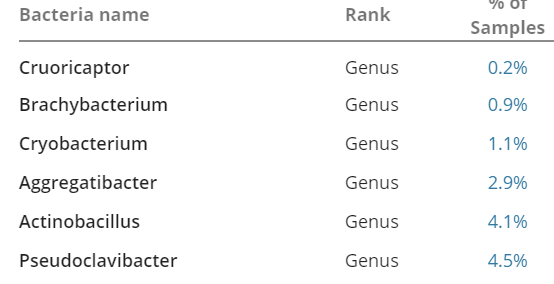
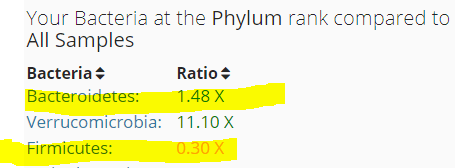
 – E.Coli’s parent — much higher than most. But Genova Diagnostics lab report Zero for E.Coli specifically.
– E.Coli’s parent — much higher than most. But Genova Diagnostics lab report Zero for E.Coli specifically.