There have been some recent articles and a nice summary from a presentation given (before the articles was published). One of the things that I have observed in some 15 years being involved with the CFS community is that hypothesis never die– despite many studies blowing holes in them. For example the view that CFS is a mitochondrial disease.
- Sara Myhill, Chronic fatigue syndrome and mitochondrial dysfunction [2009]
- Mitochondrial dysfunction in a family with psychosis and chronic fatigue syndrome[2016].
- Bottom-up proteomics suggests an association between differential expression of mitochondrial proteins and chronic fatigue syndrome [2016].
- Metabolic features of chronic fatigue syndrome [2016].
Recent research found was that the symptoms (but not the disease) are related to mitochondrial.
- Association of mitochondrial DNA variants with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) symptoms[Dec 2016].
- Mitochondrial DNA variants correlate with symptoms in myalgic encephalomyelitis/chronic fatigue syndrome [2016].
What Cornell found (and I agree!)
- Do some patients with ME/CFS identified by expert M.D.s actually have a genetic mitochondrial disease? NO
- Can mitochondrial genome variation be correlated with susceptibility to ME/CFS? NO
- Is mitochondrial genome variation correlated with particular ME/CFS symptoms or their severity? YES
- Anti-inflammatory bacterial species are reduced in ME/CFS patients? YES
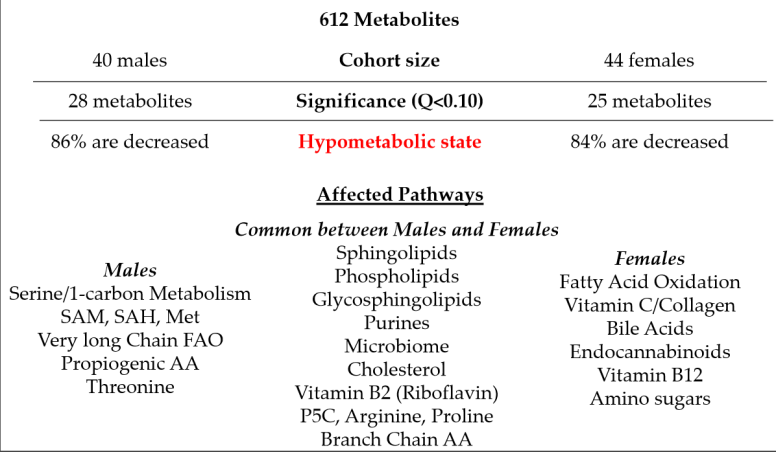

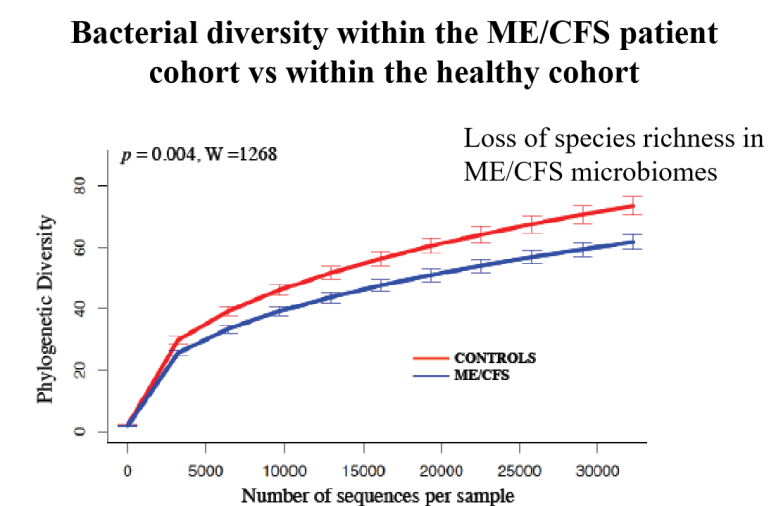
Presentations to Watch
What evidence is there of not being DNA etc.
Twin studies — Same DNA, same mitochondria. So what is the difference between having or not having CFS?
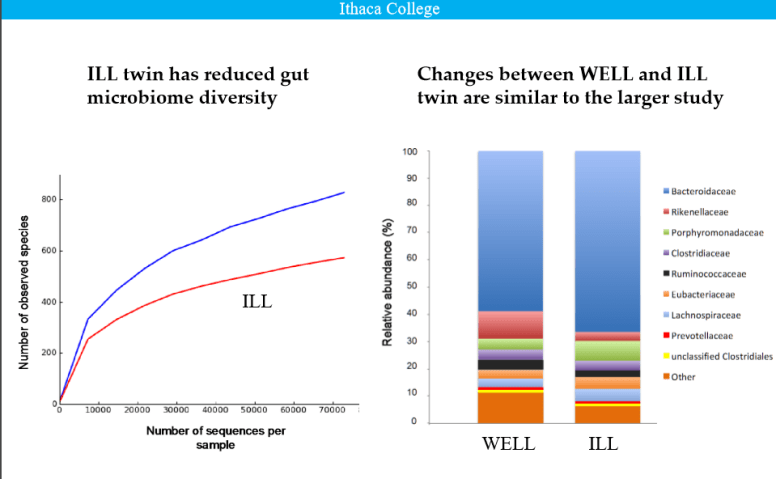
Bottom Line
My base hypothesis is that CFS/IBS/ etc is caused by a microbiome shift. This shift decreases TH1 associated bacteria and increases TH2 associated bacteria. The shift to TH2 results in increased histamine release and histamine sensitivity.
This shift results in alteration of the amino acids and the metabolites produces by the bacteria in the microbiome because different bacteria produce different amino acid and metabolites. For example, B12 is mainly produced by Lactobacilus Reuteri; if the quantity of L. Reuteri drops then a person ends up with low B12 levels.
