A reader in Germany sent a copy of their report with the following comment
“I am a reader from Düsseldorf Germany. Thank you for all the great work you do on your site. Attached are the results I mentioned in the comments on your post about KyberKompakt Pro. I do not think the results point to a definitive case of CFS in my case. Please feel free to share them if you think readers in Europe may benefit from testing by this lab.”
On first inspection, it is clear that they have a microbiome dysfunction as seen below. What appears to be the “finger print” for CFS?
Before we answer that, we need to look at the research definition for CFS. Using the CDC Case Defintion, we must have 4 out of 8 symptoms. We know that many symptoms are connected to specific bacteria — for example histamine issues and morganella species (very high histamine producers). We would not expect a perfect match for the microbiome — just at least 50% match of known shifts. For reference, see this post and prior examples (Feb 2017)
- Criteria: Low Lactobacillus — Test results Agree
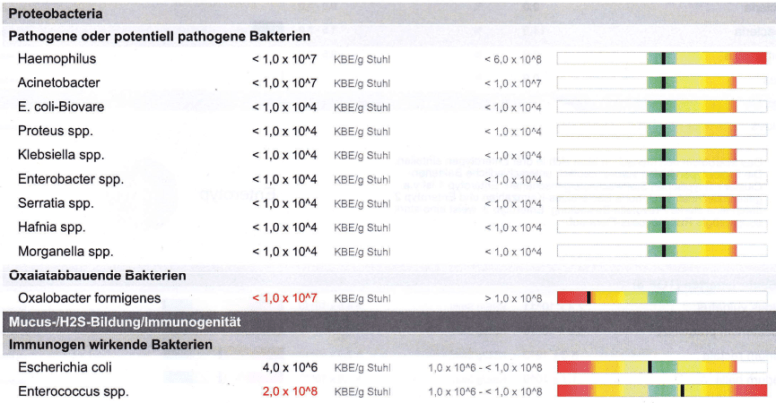
- Criteria: Low E. Coli — Test results have this person at the bottom of the normal range (likely 90% of people have higher concentrations) — possible
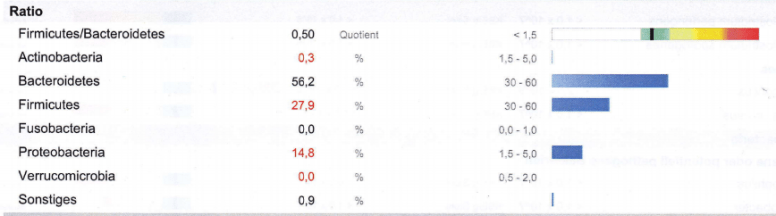
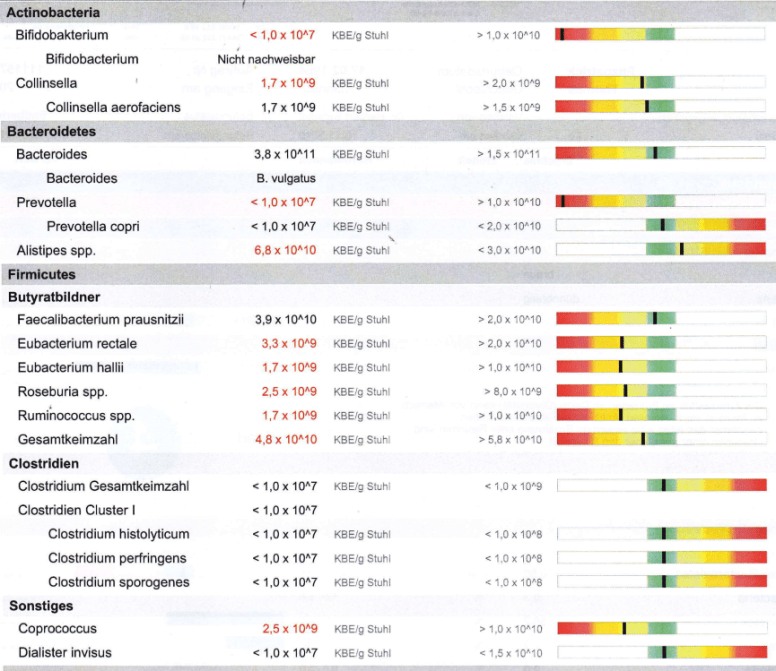
- Criteria: Low Bifidobacterium — Test results Agree (Bifidobacterium is under Actinobacteria)
- Criteria: Low Firmicutes — Test result Agreed [ see my post “83% accuracy in ME/CFS diagnosis with microbiome analysis” ]
- Criteria: Low Enterococcus — Test result High abnormal
- Criteria: Low Akkermansis — Test results Agreed [Post on]
- Criteria (.5): Low Faecalibacterium prausnitzi: — Test results normal (implies not shifting to UC or Crohns [post] occurs in some CFS patients only
- Criteria: High Candida — Test Results agreed (note that the normal “Candida species” is normal — it is the others in this family that are high)
My tally is that we have 5.5 of 7.5, with 4 out of 8 being our criteria. If I was just given this lab results, I would conclude that CFS or an associated condition is very probable.
How about a little more information about this person? See below.

Patient Notes:
- Avid cyclist, in early 50’s (7000 km cycling/year). ” I turned 50 in mid February and remember thinking that I was in the best shape of my life. One month later I was no longer riding my bike and felt terrible. I have gone through extensive testing since that time but still do not have a firm diagnosis. Recently, I have been developing more mild arthritic type symptoms. I do have a positive Rheumatoid Factor although my doctor tells me it is quite low and does not register as positive on the high sensitivity test. I did see a Natropath here who tells me I have CFS but think it is perhaps a type of Fibromyalgia. The trouble is I do not seem to fit neatly into any bucket. I do have “sticky blood” and I also have a high zonulin level which could point toward an intestinal permeability problem I have attempted significant dietary modifications but have yet to experience any real benefit.”
- Onset:
- Pneumonia that took 3 months 2 recover (similar to my own first onset of CFS)
- Subsequently “terrible headaches and very painful and stiff neck. Doctor initially said viral meningitis but this was not confirmed by serology” .. (the alternative older name for CFS is Myalgic encephalomyelitis meaning inflammation of the brain and spinal cord.)
Labs
- CT Scan and MRI in 2014 indicated no problems (I would suggest pressing for a SPECT scan, my MRI was fine, my SPECT scan was [incorrecly] diagnosised as early Alzheimer’s. See this post on appropriate brain scans)
- Dry eye – common in CFS
- Brain Fog — very common in CFS (but not for 100% of patients)
- difficulty gaining weight (currently about 140 lbs)
- Antiphospholipid antibodies (sticky blood)
- Positive for HHV-6, CMV, Coxsackie B5, Paravirus B19, Toxoplasma (almost the full house for virii associated with CFS!)
- One positive test for Lyme, negative for repeat (False positive are common if EBV is reactivated)
- Vitamin D – initially very low (March 2014) – now in low normal range. Have not found a doctor who will test 1.25 D
Bottom Line
To quote this saying “If it looks like a duck, swims like a duck, and quacks like a duck, then it probably is a duck”. Your microbiome looks like CFS, your active virus are CFS associated virii, and your complaints (symptoms) quacks like CFS, then it is probably CFS!
I am not a medical professional and thus cannot give a diagnosis. I am a statistician, and thus can state there is a high probability that it is well within the range of symptoms and conditions called CFS/ME.
Suggestions to discuss with your MD
- Given the number of virus you have, it is not probable (< 50%) antivirals would be effective (based on studies of antivirals for CFS). If I had to choose just one to try, I would likely go with Tamiflu.
- In my model, these virus have become active because the body systems to keep them in control have been disrupted. They are a consequence and not a cause.
- Candida: fluconazole and other antifungals
- Herbs and Spices: Haritaki, Wormwood, Olive Leaf, Neem, Tulsi. Many are also antivirals.
- Increase Vitamin D, perhaps up to 15,000 IU/day
- Probiotics: E.Coli (since you are in Germany, they are easy to obtain), Bifidobacteria only probiotics,
- Low molecular weight heparin or regular heparin taken sub-lingual (held in mouth for 3 minutes and then spit out — much cheaper).
- Get a full panel of inherited coagulation defects done.
