A reader commented that she, like a friend, evolved into atypical Crohn’s Disease from CFS. On the surface, it means something that looks like Crohn’s Disease but does not behaves typically or appears typically how Crohn’s disease respond to treatment.
For example and to establish definitions.
| An Atypical Presentation [2004] |
|---|
| In this case, the patient only exhibited a few of the traditional signs, symptoms and clinical findings associated with Crohn’s disease. The patient presented with an acute GI bleed, which is seen in only 20% of patients with Crohn’s disease. In this case, the disease’s onset was acute and severe, which sharply contrasts to the typical insidious onset of Crohn’s. Additionally, the patient did not experience weight loss traditionally associated with Crohn’s disease. The histology of all four specimens taken at the time of colonoscopy was similar and did not fit the usual histologic picture of ulcerative colitis or ischemic colitis. The location of the ulcers is unusual for the initial manifestation of Crohn’s disease. |
| ….Crohn’s disease is an inflammatory bowel disease marked by patchy areas of full-thickness inflammation anywhere in the gastrointestinal tract, from mouth to anus…. Crohn’s disease is mediated by T lymphocytes, which arise in genetically susceptible individuals as a result of a breakdown in the regulatory constraints on mucosal immune responses to enteric bacteria. |
- “In patients with atypical Crohn’s disease features, … prognosis can be remarkably favorable upon oral treatment with cyclophosphamide.” [2016] – this has high toxicity.
- A Case of Intestinal Mastocytosis Misdiagnosed as Crohn’s Disease [2015]. This is too many mast cells producing too much histamine.
This is a nice study, The Treatment-Naive Microbiome in New-Onset Crohn’s [2014] Disease which shows a both any treatment and what happens with treatment with an antibiotic.
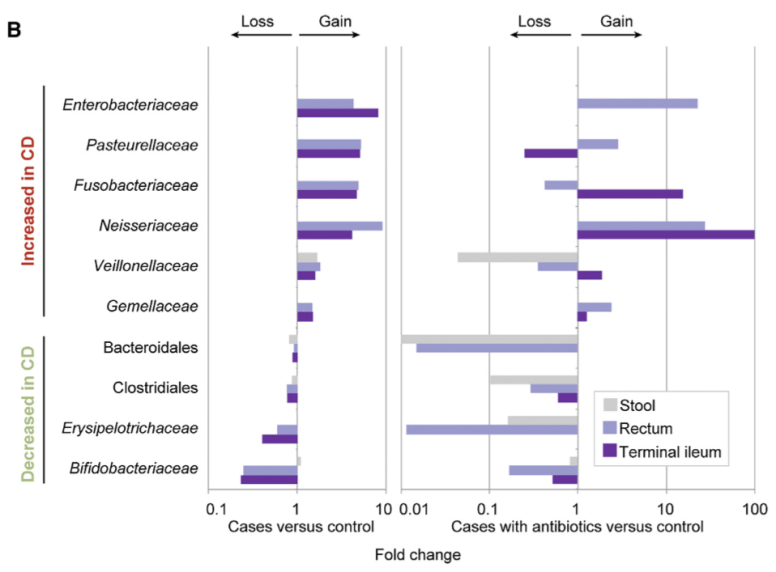
Note some factors shared with CFS and FM microbiomes:
- Major decrease if bifidobacteria [Kyberompact Post]
- Increase of Enterobacteriaceae as seen with IBS [2016]
The differences:
- Pasteurellacease are normal or low in CFS [Post], high in Crohn’s disease
- Fusobacteriaceae are normal in CFS, high in Crohn’s disease
- Some species of Veillonellaceae are low in CFS [post], the entire group is high in Crohn’s disease
The two biggest shifts (the biggest increase and the biggest decrease) in Crohn’s disease are also seen with CFS. The difference is that other families have not shifted yet. How the body responds to further shifts is influenced by DNA.
This study also illustrate the effect of antibiotics — they appear to make the total shift worst (but may result in some symptom relief).
Bottom Line
As I wrote earlier: Autoimmune = DNA + Microbiome shift. The more that shifts, the worst the autoimmune condition can become. Which autoimmune disease is likely a function of your DNA. If you are unlucky, you may end up with several pages of diagnosis. The final problem is how to shift the microbiome back to normal. The first step is to inhibit further shifting: for CFS, given what is available, it appears to be E.Coli probiotics and bifidobacteria probiotics as a starting point.
