I wrote about Magnesium and Malate acid back in 2012. There are sites that takes you thru the pros and cons of different magnesiums such as MAGNESIUM SUPPLEMENTS: DIFFERENT TYPES & DIFFERENT BENEFITS. I wish to do a short revisit by looking only at the pH of each because a hypothesis suggests that those having a higher pH (more alkaline) would likely have additional impact beyond just the magnesium.
- Magnesium Gylcinate 9 – 11 [source] – $1.50/gram
- Magnesium Oxide – 11.2 $ 0.02 /gram
- Magnesium Citrate – 4.0 [source] [source] $0.85/gram
- Magnesium Malate – 7 – 11 [source] $0.05/gram
- Magnesium Taurate – 9-10 [source] $1.00 /gram
- Magnesium Threonate -5.8 – 7 [source] $ 0.50 /gram
- Magnesium Carbonate – 10.41 $0.02 /gram
- Magnesium Hydroxide (Milk of Magnesia) – 10.5 [source] $0.03/gram
There are three dimensions to consider:
- Ability for magnesium to get absorbed (instead of just passing thru) — see link at top
- pH of the product (more pH is usually better)
- cost of the product.
Importance of Magnesium
- “Low intake of omega-3 fatty acids, vitamin B6, magnesium, zinc and antioxidants may also play a supporting role in symptom occurrence.” [2016]
- “This pilot study suggests that transdermal magnesium chloride applied on upper and lower limbs may be beneficial to patients with fibromyalgia.” [2015]
- “The number of tender points, tender point index, FIQ and Beck depression scores decreased significantly with the magnesium citrate treatment. The combined amitriptyline + magnesium citrate treatment proved effective on all parameters except numbness. Low magnesium levels in the erythrocyte might be an etiologic factor on fibromyalgia symptoms.” [2013]
- Women with fibromyalgia have lower levels of calcium, magnesium, iron and manganese in hair mineral analysis [2011].
- The relationship between serum antioxidant vitamins, magnesium levels, and clinical parameters in patients with primary fibromyalgia syndrome [2011].
- “Magnesium sulphate, a substance known to cause release of cholecystokinin (CCK) from the small intestinal mucosa, was given by mouth (dose 0.1g/kg in 150 ml water) to 20 patients with the irritable bowel syndrome. …These findings provide further evidence that ;functional’ abdominal pain after food may in some cases be related to an exaggerated intestinal motor response to cholecystokinin.” [1973]
- “The diet of IBS patients was found to consist of a low calcium, magnesium, phosphorus, vitamin B2 and vitamin A content.” [2012]
- Magnesium deficit in a sample of the Belgian population presenting with chronic fatigue [1997].
- “[Chronic Fatigue] Patients treated with magnesium claimed to have improved energy levels, better emotional state, and less pain, as judged by changes in the Nottingham health profile. 12 of the 15 treated patients said that they had benefited from treatment, and in 7 patients energy score improved” [1991]
- Cognitive behaviour therapy for the chronic fatigue syndrome. Evening primrose oil and magnesium have been shown to be effective [1996].
- “magnesium was demonstrated effective on ME/CFS patients’ symptom profiles.” [2012]
- [A case of chronic fatigue syndrome who showed a beneficial effect by intravenous administration of magnesium sulphate] [1992].
- Magnesium status and parameters of the oxidant-antioxidant balance in patients with chronic fatigue: effects of supplementation with magnesium [2000]. “Mg supplementation was followed by an improvement in Mg body stores, in serum vitamin E and its interrelated stage of lipid peroxidation.”
- “Magnesium (p = .002) and support groups (p = .06) were strongly associated with fatigue worsening from 6 months to 2 years.” [2005]
- “Red blood cell magnesium concentrations were measured in samples from 89 patients who fulfilled the diagnostic criteria for chronic fatigue syndrome and the results compared to those found in an age and sex matched group selected from the normal population. No significant difference was found. … There is therefore no indication for the use of magnesium therapy in the management of this condition.” [1994] – note that was confined to red cell analysis only.
- Chronic fatigue syndrome and chronic primary magnesium deficiency (CFS and CPMD) [1992].
Microbiome Dimension
- Changes in intestinal bifidobacteria levels are associated with the inflammatory response in magnesium-deficient mice [2010]. Mg+ and Mg- below indicate deficient or increased. After 4 days, both bifido and lactobacillus increased.
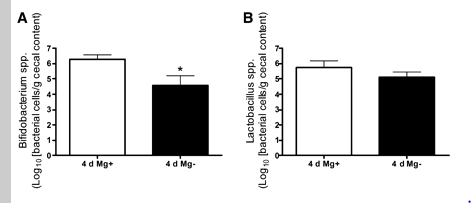
- “We conclude that calcium and magnesium fluxes play an important role in the physiology of the bifidobacteria and that several metal growth inhibitors interfere with iron metabolism.” [1984]
- Mg improves the thermotolerance of probiotic Lactobacillus rhamnosus GG, Lactobacillus casei Zhang and Lactobacillus plantarum P-8 [2017].
- Mn(2+) and Mg(2+) synergistically enhanced lactic acid production by Lactobacillus rhamnosus FTDC 8313 via affecting different stages of the hexose monophosphate pathway [2014].
- “Nutritional requirements of Lactobacillus delbrueckii subsp. lactis in a chemically defined medium[2004]. “Magnesium was the only essential oligoelement.”
pH factor
Optimal pH for Bifidobacterium bifidum is 7.0 [source] with other sources saying 6.5 – 7.0. Stomach acid is around 1.0-3.0. This raise the question whether it may be good to take you bifidobacteria with magnesium instead of at a separate time..
From National Institute of Health site:
- “Diets with higher amounts of magnesium are associated with a significantly lower risk of diabetes,”
- “People who experience migraine headaches have lower levels of serum and tissue magnesium than those who do not.”
- ” taking 300 mg magnesium twice a day, either alone or in combination with medication, can prevent migraines”
- “Forms of magnesium most commonly reported to cause diarrhea include magnesium carbonate, chloride, gluconate, and oxide [11].”
Bottom Line
Magnesium impact on CFS etc may be because it encourages the growth of Lactobacillus and Bifidobacteria
Magnesium oxide/Magnesium Hydroxide are cited as less bioavailable. My conclusions today are still the same as in 2012, Magnesium Malate is the best bang for the buck (and bucks are always sparse for CFS patients!). Dosage should be determined by your MD, the literature indicated that 5000 mg/day can create problems with the young and the elderly, I would question more than 1000 mg/day and suggest that 600 mg/day (used to treat another condition successfully) may be warranted.
Note: Magnesium Malate tablets cited as 1250 mg is not 1250 mg of magnesium, just 425mg for three 1250mg tablets. That is 140 mg or magnesium per tablet, so 7 tablets of 1250mg per day would be needed to reach 1000 mg/day.

A very common mistake that CFS patients make in their brain fog is thinking that their dosage are sufficient. “Yes, I am taking Magnesium — it is in my multivitamin!” (Looking at Centrum multivitamins, I see there is 64 mg, approximately 1/10 of what may be needed to do corrective action for low magnesium).
As always, start with a low dosage and slowly work up.
THIS IS NOT MEDICAL ADVICE — this post is an education summary of what has been reported on PubMed. Always consult with a knowledgeable medical professional before changing diet, supplements and prescription drugs.
