A Bioscreen report was pending in my in-box. Bioscreen tests for a lot less bacteria genus than uBiome. I have done a prior post on a Bioscreen analysis. There are no perfect tests, nor perfect knowledge about what different bacteria genus do. I apply a logic model to what is available
Report
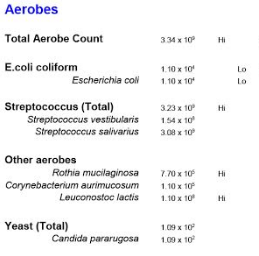

Standard Items
- Bifidobacterium is HIGH, totally atypical for CFS
- I would love to know the strains — it is possible to have bad strain in any family (just like real families!)
- Lactobacillus is LOW — as expected
- E. Coli is LOW as expected.
Overgrowths
With links to DataPunk.Net. The first thing that I saw was that none of these were included in my earlier deep dives — that is, we have a different profile which may account for the high bifidobacterium.
- Streptococcus – a genus
- Terrabacteria group -> Firmicutes -> Bacilli -> Lactobacillales -> Streptococcaceae -> Streptococcus
- Rothia mucilaginosa – a species that produces lactic acid from d-glucose and gluten
- Terrabacteria group -> Actinobacteria -> Actinobacteria -> Micrococcales -> Micrococcaceae -> Rothia -> Rothia mucilaginosa
- Leuconostoc lactis – a species that produces lactic acid from d-glucose
- Terrabacteria group -> Firmicutes -> Bacilli -> Lactobacillales -> Leuconostocaceae -> Leuconostoc -> Leuconostoc lactis
Reference:
- Streptococcus: https://cfsremission.wordpress.com/2017/10/25/reducing-streptococcus-genus/
- Rothia: https://cfsremission.wordpress.com/2017/10/25/decreasing-rothia-genus/
- Leuconostoc: https://cfsremission.wordpress.com/2017/10/26/reducing-leuconostoc-genus/
What the bug is going on????
I contacted the reader and was informed they also have a diagnosis of Coeliac disease (which caused me to research Coeliac disease’s microbiome shifts and do a post). With both CFS and Celiac disease Low or No bifidobacterium is expected NOT AN OVERGROWTH!
Every overgrowth reported is atypical — not commonly seen with prior CFS uBiome results (I had to do three more deep dives to write this post!).
I wrote the reader because I was concern that there may be another condition that has been misdiagnosed. Another autoimmune disease, primary sclerosing cholangitis
“Rothia, Enterococcus, Streptococcus, Veillonella, and three other genera were markedly overrepresented in primary sclerosing cholangitis” [2017] and we have “Our data do not support beneficial effects of probiotics[four Lactobacillus and two Bifidobacillus strains] on symptoms, liver biochemistry or liver function in PSC.” [2008] which hints that bifidobacillus may not be reduced as well as this 2016 study
Addendum
After this was posted, I received additional information which may explain the results.
- “My doctor prescribed 2 courses of EES (erythromycin) – one week antibiotics, one week probiotics (Mutaflor and Metagenics LGG), then repeat. He also recommended taking L-Glutamine, Bio-Gest, Arginine and Citrulline for my personal circumstances.”
- Streptococcus overgrowth is often reported after antibiotics.
- “both antibiotic-treated groups had distinct gut microbial communities and metabolites, including a reduction of bacterial diversity and an enrichment of harmful bacteria such as Streptococcus and Pseudomonas. ” [2017]
- Streptococcus overgrowth is often reported after antibiotics.
- “Regarding high Bifido, I was taking a multi-strain probiotic containing the exact strain of Bifido I am high in, and stopped it only 6 days prior to completing the BioScreen test due to some time constraints. I’m not sure whether Bifido has strong staying power in comparison to Lactobacillus (as I had zero Lacto despite it being in the same probiotic formula).”
- “This randomized, parallel-group, open-label trial (n=36) included a 4-week run-in, 2-week intervention, and 3-week follow-up period. …Bifidobacterium …was found at the end of the intervention (P<0.01 and P<0.001, respectively) and in the recovery time during follow-up (P<0.05 for both). ” [2010]
- “Viable counts of fecal lactobacilli were significantly higher (P=0.05) and those of enterococci were significantly lower (P=0.04) after the intervention (of Bifidobacterium animalis subsp. lactis (BB-12) and Lactobacillus acidophilus (LA-5) _ when compared to placebo. ” [2011]
Bottom Line Theoritical Items
Despite not knowing if this is or is not CFS — we can still apply theory to correct the shifts. I would greatly prefer to be working from a uBiome report for this reader — things are just weird!
The lists below are done by merging the lists from the deep dives linked above. Some items may encourage one genus and discourage another genus — those are placed in inconclusive. The impact on Lactobacillus, Bifidobacterium and E.Coli are intentionally ignored [See this post for the logic]. This is all based on applying logic to the results of studies — thus theoretical. The last one was only partially done because high levels are often deemed to be good. This is an addition (not a replacement) to this overview post.
Avoid
- Kefir
- Sauerkraut
- ad hoc Fermented Food
- olives
- cucumbers
- wine
- cheese
- gluten (based on overgrowth genus)
- Proton-pump inhibitors (PPI)
- Hospital Food
Take
- Vitamin D
- Licorice
- Triphala
- Figs
- Olive Leaf
- Turmeric
- Magnolia Bark
- Black cumin Seed
- Gooseberry
- Chinese Ginger, Fresh Ginger
- Stevia
- Aloe vera
- Garlic (allicin)
- Cinnamon bark oil
- Peppermint oil
- Hyocyamine
- Berberine
- Thyme oil
- Salvia officinalis, Common Sage
- Eucalyptus globulus, Tasmanian bluegum
- Coleus forskohlii, Plectranthus barbatus, Indian Coleus
- Coptis chinensis, Chinese gold thread
- Turnera diffusa, Damiana
- Larrea tridentata, chaparral, gobemadora, greasewood, creosote bush
- Withania somnifera
- Green Tea
- Resistant starch (type IV)
- Lemongrass oil
- Navy bean (Cooked)
- Bacillus clausii
- Lactobacillus casei Shirota
- Lactobacillus casei
- Lactobacillus Reuteri
- Lactobacillus paracasei
- Lactobacillus plantarum
- Lactobacillus salivarius
- Propionibacterium freudenreichii
Addendum to Bottom Line
The microbiome examined was not “stable” but impacted by both erythromycin and bifidobacterium longum probiotics. The scope of bacteria genus covered by this test is very sparse — so I apart from the above that may reduce Streptococcus, inference from this study is questionable.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of CFS or other disease. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.
