I know many people whose autoimmune condition appear to have been triggered by mold or fungus exposure. Mold or mould is a fungus — so my focus will be fungus (which included the subset mold). I have not explore this area explicitly before.
From Wikipedia:
Toxic house mold
The common house mold, Trichoderma longibrachiatum, produces small toxic peptides containing amino acids not found in common proteins, like alpha-aminoisobutyric acid, called trilongins (up to 10% w/w). Their toxicity is due to absorption into cells and production of nano-channels that obstruct vital ion channels that ferry potassium and sodium ions across the cell membrane. This affects in the cells action potential profile, as seen in cardiomyocytes, pneumocytes and neurons leading to conduction defects. Trilongins are highly resistant to heat and antimicrobials making primary prevention the only management option.
Fungus Produced Toxins
- “toxins were identified with HPLC/ESI-MS/MS as trichorzianines, trilongins, trichostrigocins and trichostrigocin-like peptaibols.” [2018]
- “Buildings that have been flooded often have high concentrations of Trichoderma spores in the air while drying… inhalation of Trichoderma spores and mycelial fragments may result in exposure to membrane-disrupting peptaibols. This investigation contributes to a more comprehensive understanding of the biologically active natural products produced by fungi commonly found in damp buildings.” [2017]
- “Peptaibols are a family of antimicrobial peptides, which are synthesized by non-ribosomal peptide synthetases (NRPS) and contain high proportions of alpha-aminoisobytyric acid (Aib). Up to now, 317 peptaibols have been identified, and the majority of them are produced by Trichoderma strains.” [2011]
Clearly, mold can and does impact the microbiome. Eliminating the mold in the body (after verifying that it is there) is a first step. The second step is restoring the microbiome.
- “Dr. Brewer reports that chronic fatigue syndrome patients are much more likely than healthy people to have mold toxin in their urine…Brewer found that 94% of his CFS patients had at least one kind of mycotoxin detected in their urine. ” [src] Discussion of the studies.
- The published studies are [2013] and [2014].
- A recover study:
”
Antifungal and the Microbiome
Recently I added antifungals to the list of gut modifiers. These are listed at antifungal (prescription):
- amphotericin b (prescription)
- bifonazole (prescription)
- butenafine hydrochloride (prescription)
- butoconazole nitrate (prescription)
- chlorphensin carbamate (prescription)
- ciclopirox ethanolamine (prescription)
- clotrimazole (prescription)
- econazole nitrate (prescription)
- fluconazole (prescription)
- flucytosine (prescription)
- griseofulvin (prescription)
- haloprogin (prescription)
- isoconazole (prescription)
- itraconazole (prescription)
- ketoconazole (prescription)
- liranaftate (prescription)
- miconazole (prescription)
- naftifine hydrochloride (prescription)
- nystatine (prescription)
- oxiconazole nitrate (prescription)
- sertaconazole nitrate (prescription)
- sulconazole nitrate (prescription)
- terconazole (prescription)
- tiabendazole (prescription)
- tioconazole (prescription)
- tolnaftate (prescription)
- voriconazole (prescription)
The enhancement that I added recently, described in this post, Improved filtering of gut modifiers, allows the impact of various antifungals on your microbiome to be viewed.
The little trick to see the impact of prescription drugs on your ubiome
- AFTER logging in to http://microbiomeprescription.azurewebsites.net
- Click one of the above, for example itraconazole (prescription)
- You will see it’s address is: http://microbiomeprescription.com/Library/Modifier?mid2=649
- Simply add “&seq=999999” (where 9999999 is your own sequence number) and you will see what this antifungal also impacts. An example (for a person with mold triggered CFS is used)
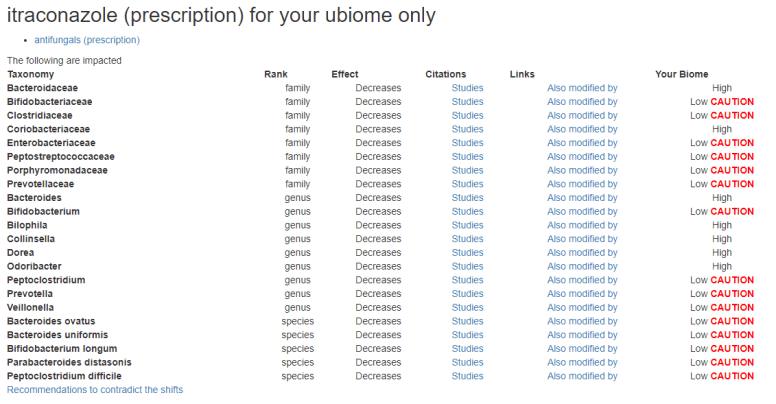
Finding a perfect fit is unlikely. The algorithm used on the site attempts to balance the pro-and-cons. Your medical professional can do your own tuning with the above. With prescription drugs there can be many factors involved for a specific patient.
For example, this one may be a better profile than above:
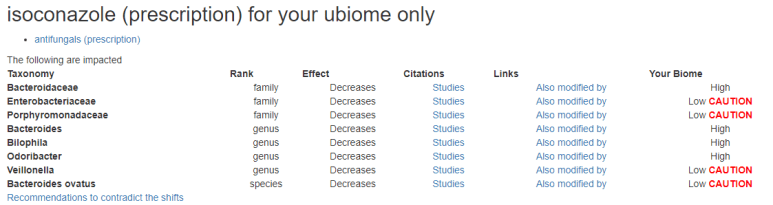
with this appearing to be the second choice
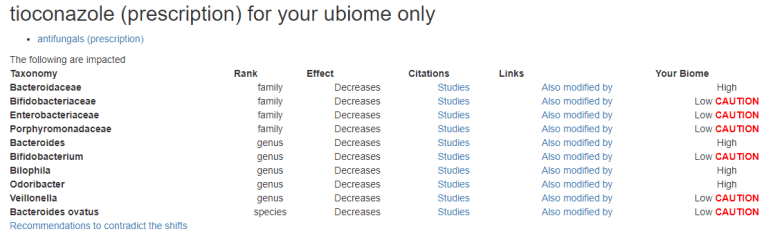
Bottom Line — review for other prescription drugs
With drugs, pharmacists know the term “contraindicated“. This means two drugs have undesired side-effects. Using the above technique, we can identify drugs that may be contraindicated for your current microbiome.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.
