A reader asked me to look at these and other antivirals for Myalgic encephalomyelitis/chronic fatigue syndrome :
“I hope your 2023 is off to a healthy start. I was wondering if you could look into how Paxlovid and similar protease inhibitor-style antivirals impact the microbiome.
I got Covid around Christmas and was prescribed Paxlovid. To my surprise, not only did I immediately feel better Covid symptom-wise, but there were many other positive changes.
My brain fog and fibromyalgia-like symptoms improved quickly and drastically. Unfortunately, these changes did not last very long after finishing my course of Paxlovid.
A similar thing also happened to me years ago when I got influenza A and was prescribed Tamiflu.
Also, anecdotally, from Twitter and Facebook groups around CFS, I know I’m not the only one to have this experience with Paxlovid.
There is also at least one trial underway testing the use of Paxlovid in Long covid patients.
Or perhaps it could also relate to the additional antiparasitic and/or anti-inflammatory actions of some antivirals?
Very curious to get your take and expertise on how this might be microbiome related.”
From a reader
Conceptual Model
It is well documented that virus changes the microbiome (see this list 20+ studies for COVID). A possible reason is that the virus wants to increase substances it needed to reproduce and decrease the substances that inhibits it. This is done by chemical signaling — the virus sends bogus messages to the microbiome.
By reflection, it is likely that antivirals also change the microbiome – possibly by reversing the changes done by the virus. Likely along the same mechanism.
” a viral infection usually results in substantial perturbations in the commensal microbiota, causing dysbiosis in the host, which may in turn further affect viral infectivity.” [2019]
“HCV infection alters the gut microbiota, whereas intestinal dysbiosis induces an underlying inflammatory state.” [2023]
For some literature on this – note that this has only become of interest in research very recently:
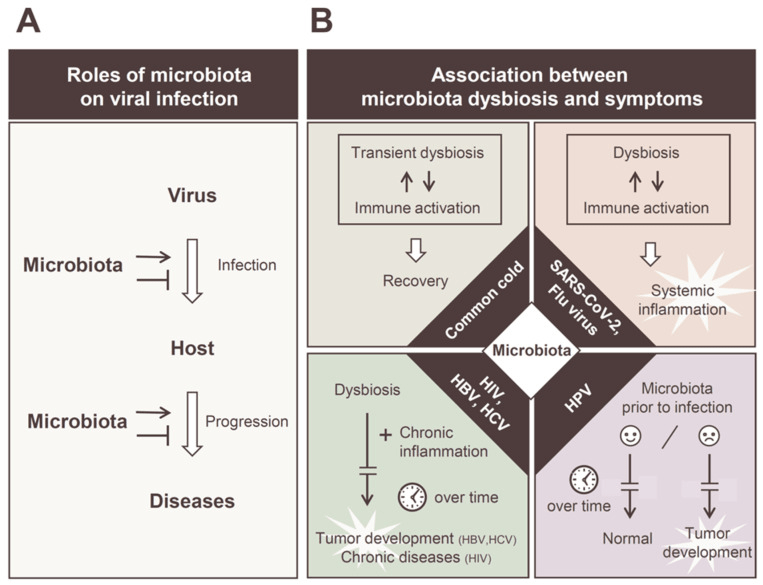
- Role of Microbiota in Viral Infections and Pathological Progression [2022] (digram below)
- The Interaction Between Viruses and Intestinal Microbiota: A Review [2021]
- Viral Infections, the Microbiome, and Probiotics [2021]
- Intestinal Microbiota-A Promising Target for Antiviral Therapy? [2021]
- How the gut microbiome regulates host immune responses to viral vaccines [2019]
- The Commensal Microbiota and Viral Infection: A Comprehensive Review [2019]
Past Studies of Antivirals and ME/CFS
I have covered some in some past posts:
- Valacyclovir, EBV and CFS [2016]
- Valganciclovir antiviral and CFS [2016] 21% improved
- Also see Viral Reactivation and the Microbiome [2020]
Valacyclovir has information available on the microbiome impact. For other antivirals I was not able to find new studies in the ME/CFS context
What was interesting is for a condition that is comorbid, Sjögren’s syndrome
- Microbiota dysbiosis in primary Sjögren’s syndrome and the ameliorative effect of hydroxychloroquine [2022]
Antiviral Impact on Microbiome
“The use of antiretrovirals caused a significant impact on the individuals intestinal microbiota” [2007]
- Influence of hepatitis C virus eradication with direct-acting antivirals on the gut microbiota in patients with cirrhosis [2018]
- Enterobacteriaceae, Enterococcus, and Staphylococcus was decreased
- Short-term high-dose gavage of hydroxychloroquine changes gut microbiota but not the intestinal integrity and immunological responses in mice [2021]
- Altered Gut Microbiome under Antiretroviral Therapy: Impact of Efavirenz and Zidovudine [2021]
- Raltegravir:
- Gut microbiota alterations after switching from a protease inhibitor or efavirenz to raltegravir in a randomized, controlled study [2023] Prevotella 9 (higher), Phascolarctobacterium and Bacteroides (Lower)
Bottom Line
Antivirals likely have antibiotics like effects on the microbiome. This is documented above. The problem is a lack of studies on which bacteria are impacted. This gives it uncertainty for being effective for any specific individuals.
My wish is that for any long term studies using these for Long COVID or ME/CFS is that microbiome samples be done before after and then 3 months after treatment stops. This would provide concrete information that can be applied at an individual.
My gut feeling is that a single course will not be sufficient for remission. I would suggest following the pattern of rotating and pulsing the antivirals which has helped. This could be combined with appropriate antibiotics. For those not familiar with this pattern:
- Once a month take a course of antiviral or antibiotics (7-14 days) and then nothing for the rest of the month
- Next month take a different one
There are several studies showing that this pattern is more effective than continuous. The conceptual model is that you disturb the bad bacteria and give a chance for the good bacteria to attempt a recovery. The survivors of the bad ones slowly regrow, changing antibiotics or antiviral will typically reduce these survivors because the new substance mechanism is different (so the antibiotic-resistance genes that the survivors had, may not work anymore).
More Coming…
“Thanks, Ken! Just saw the posted version. It won’t be perfect, but I do have a sample about a month before I got Covid and have one on the way, which will be sampled about two weeks after finishing Paxlovid. Not sure you’ll be able to glean anything from that specific test, but worth a shot.”
