Several readers asked me to summarize Rheumatoid arthritis and the microbiome like I did for multiple sclerosis. The readers often cited high rates of RA in immediate family, and the risk was known since at least 1993. A followup post on mitigation is here.
“A high frequency of small intestinal bacterial overgrowth was found in patients with RA; it was associated with a high disease activity and observed in patients with hypochlorhydria or achlorhydria and in those with normal acid secretion.” [1993]
The pattern for autoimmune seem to be an interaction between DNA/SNPS/Genes and the microbiome. How the two come together determines if onset occurs, severity etc.
DNA is not an easy to change. Microbiome is. Many successful treatments for rheumatoid arthritis have involved antibiotics before the microbiome dimension was discovered.
- “In this article, we discussed the role of gut microbiota in the pathogenesis of rheumatic diseases based on a large number of experimental and clinical materials, thereby providing a new insight for microbiota-targeted therapies to prevent or cure rheumatic diseases.” ]2017]
- “Altered microbiota, well described in patients affected by RA, seems associated with perturbation of certain metabolic pathways and the therapies addressed to correct gut microbiome dysbiosis could help in the maintenance of immune homeostasis of the host.” [2017]
- From [20172017]
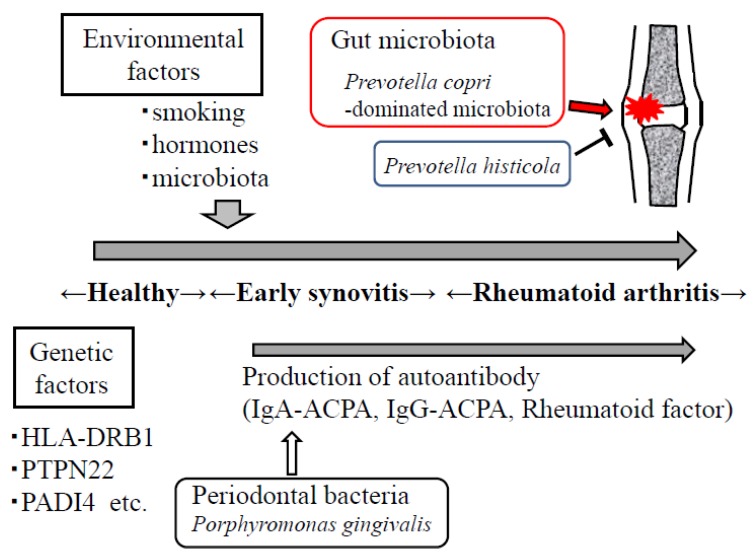
Rheumatoid arthritis and the Microbiome
-
- Intestinal Dysbiosis and Rheumatoid Arthritis: A Link between Gut Microbiota and the Pathogenesis of Rheumatoid Arthritis [2017].
- “in this disease, about 100 described genes are associated with susceptibility, protection, severity, activity, and treatment response “
- ” a reduction of certain bacteria belonging to the family Bifidobacterium and Bacteroides”
- “a marked increase of species belonging to the genus Prevotella”
- “We and others have demonstrated that the abundance of Prevotella copri is increased in some early RA. ..On the other hand, Prevotella histicola from human gut microbiota suppressed the development of arthritis. In summary, Prevotella species are involved in the pathogenesis of arthritis.” [2017]
- “These findings indicate that some Prevotella strains may be clinically important pathobionts that can participate in human disease by promoting chronic inflammation.” [2017]
- Evidence of the Immune Relevance of Prevotella copri, a Gut Microbe, in Patients With Rheumatoid Arthritis[2017].
- Reduced:[2015]
- Eubacterium rectale-Clostridium coccoides group
- Bacteroides fragilis subgroup etc.
- Veillonella,
- Haemophilus
- Increased:[2015]
- Clostridium asparagiforme
- Lactobacillus salivarius etc
- Prevotella copri
- Intestinal Dysbiosis and Rheumatoid Arthritis: A Link between Gut Microbiota and the Pathogenesis of Rheumatoid Arthritis [2017].
- “the genus Pseudonocardia and various related OTUs were the only taxa overrepresented in RA bronchoalveolar lavage fluid and correlated with higher disease activity and erosions.”[2016]
- The aggravation of arthritis by periodontitis is dependent of IL-17 receptor A activation[2017].
- “The effects of P. gingivalis-induced periodontitis on arthritis … lead to increased neutrophil infiltration into the joints.”
- The oral and gut microbiomes are perturbed in rheumatoid arthritis and partly normalized after treatment[2015].
- “The redox environment, transport and metabolism of iron, sulfur, zinc and arginine were altered in the microbiota of individuals with RA.”
- Alteration of Fecal Microbiota Profiles in Juvenile Idiopathic Arthritis. Associations with HLA-B27 Allele and Disease Status[2016].
- HS: Healthy Subjects
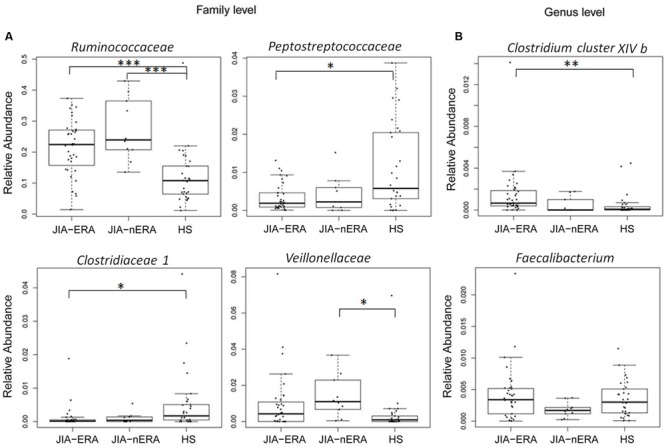
- “abundant taxa identified JIA patients for the HLA-B27 allele, including Bilophila, Clostridium cluster XIVb, Oscillibacter, and Parvimonas. “
- “reduction in Clostridiaceae and Peptostreptococcaceae in JIA-ERA, and increase in Veillonellaceae in JIA-nERA, “
- “A growing number of microbiota constituents such as Prevotella copri, Porphyromonas gingivalis, and Collinsella have been correlated or causally related to rheumatic disease. [2016]
- “Mice susceptible to collagen-induced arthritis (CIA) showed enriched operational taxonomic units (OTUs) affiliated with the genus Lactobacillus as the dominant genus prior to arthritis onset. With disease development, the abundance of OTUs affiliated with the families Bacteroidaceae, Lachnospiraceae” [2016]
- An expansion of rare lineage intestinal microbes characterizes rheumatoid arthritis [2016].
- “A taxon-level analysis suggested an expansion of rare taxa, Actinobacteria, with a decrease in abundant taxa in patients with RA compared with controls. Prediction models based on the random forests algorithm suggested that three genera, Collinsella, Eggerthella, and Faecalibacterium, segregated with RA. The abundance of Collinsella correlated strongly with high levels of alpha-aminoadipic acid and asparagine as well as production of the proinflammatory cytokine IL-17A. A role for Collinsella in altering gut permeability and disease severity was confirmed in experimental arthritis.”
- “reducing the concentration of Bacteroides spp., Bifidobacterium spp., Lactobacillus spp. populations, typical strain E. coli. But over growth of populations Klebsiella spp., Proteus spp., Staphylococcus spp., atypical forms of E. coli, Candida spp. ” [2014]
Treatment Options
- Anti-arthritic activity of cell wall content of Lactobacillus plantarum in freund’s adjuvant-induced arthritic rats: involvement of cellular inflammatory mediators and other biomarkers [2017].
- “Cell wall content of L. plantarum treated animals showed improvement in all the parameters as compared to that in CFA-treated animals and exert anti-arthritic activity.”
- ” pretreatment with L. salivarius could significantly improve CIA in mice and may help alleviate RA in a clinical setting.” [2016]
- The effects of orally administered Bacillus coagulans and inulin on prevention and progression of rheumatoid arthritis in rats [2016].
- “the oral intake of probiotic B. coagulans and prebiotic inulin can improve the biochemical and clinical parameters of induced RA in rat.”
- “More importantly, the altered gut microbiome and oral microbiome of RA patients were partially corrected by disease-modifying antirheumatic drugs (DMARDs). ” [2015]
- Recent infections are associated with decreased risk of rheumatoid arthritis: a population-based case-control study [2015].
- “Gastrointestinal and urogenital infections, but not respiratory infections, are associated with a significantly lowered risk of RA. “
- Effects of Lactobacillus casei supplementation on disease activity and inflammatory cytokines in rheumatoid arthritis patients: a randomized double-blind clinical trial[2014].
- “Probiotic supplementation may be an appropriate adjunct therapy for RA patients and help alleviate symptoms and improve inflammatory cytokines.”
- “L. casei 01 supplementation improved the disease activity and inflammatory status of patients with RA.” [2014]
- ” the results of this study indicated that taking probiotic supplements (Lactobacillus acidophilus (2 × 10(9) colony-forming units [CFU]/g), Lactobacillus casei (2 × 10(9) CFU/g) and Bifidobacterium bifidum (2 × 10(9) CFU/g) for 8 weeks.) for 8 weeks among patients with RA had beneficial effects on DAS-28, insulin levels, HOMA-B and hs-CRP levels.”[2016]
Bottom Line
The first item is a refrain from older posts — start by getting your mouth in shape!
- “The association between rheumatoid arthritis (RA) and periodontitis is well established.” [2016]
During the survey found several probiotics having symptom relief of RA, the ones that are easy to obtain are:
- Lactobacillus casei
- Lactobacillus plantarum
- Bacillus coagulans
In my next post, I will do the same type of theoretical analysis that I did for multiple sclerosis.
The gem of knowledge that I found interesting was “Gastrointestinal and urogenital infections, but not respiratory infections, are associated with a significantly lowered risk of RA. “. A hundred years ago, this information could have lead to the intentional causing of a gastrointestinal infection to treat RA — similar to the willful infection of Cowpox to prevent Smallpox [History]. I would not be surprise to read of people recovering from CFS after a bout of stomach flu (viral gastroenteritis) — it’s theoretically possible.
As always, this is intended as an educational post and not intended to treat any condition. Always consult with a knowledgeable medical profession before modifying supplements, diet, etc.


