A reader who has been very very limited in what they can eat due to histamine response — so limited that a good day is just 500 calories. She has stated taking benadryl once a day with major improvement.
She started taking it on the suggestion of a physician when she shared with the physician that she may have a mast cell dysfunction. I must emphasis, that she was careful to ‘share a suspicion‘ — informing a physician of your self-diagnosis often leads to labelling by medical professional and poor cooperation.
Benadryl is diphenhydramine. It is also known as Benadryl, Banophen, Diphenhist, Wal-Dryl, Nytol, Unisom, ZzzQuil, Diphen, Benadryl Allergy, Aller-G-Time, and more
Why Benadryl and not some arbitrary antihistamine?
“Diphenhydramine is a sedating peripheral H1 receptor antagonist. It is used for symptomatic relief of allergic symptoms caused by histamine released in response to allergens.”[eMedicine] H1 receptor antagonist is the fancy way of saying H1-Blocker.
As with most things biological, there are multiple paths to a reaction. In some cases a H2 blocker is a better choice. [eMedicine] lists these as other H1 blockers and sedating (quieting the release of histamines):
There are other H1 blockers but they are not poor sedating or selective. These include:
In short, all antihistamines are not the same in how they are acting. Finding the right one if you are dealing with histamine and mast cell issues is essential.
But Wait! Let us examine the difference in Microbiome impact!
I tend to be a firm believer that some medicines and drugs also owe their effectiveness to changes of the microbiome they cause.These changes alter metabolites/chemicals the the microbiome produces and the body reacts to. Unfortunately, information on the expensive diamine oxidase (DAO) that is used also, is not available.
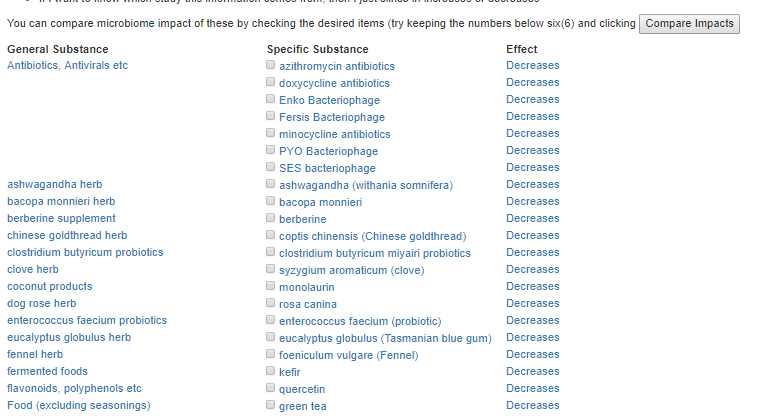
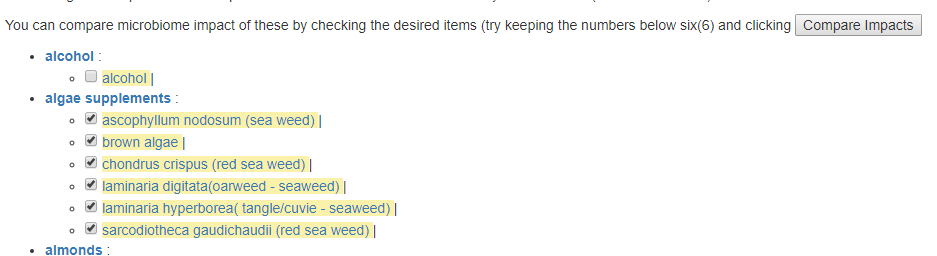
In time, I have a page to allow readers to do this themselves on my http://microbiomeprescription.com/ site – that is, examine microbiome impact when there are multiple candidate drugs to treat an issue.
Table below in Excel: Antihistamines
- -1 : decreases
- 1 : increases
- 0 : no impact
| tax_rank |
tax_name |
Hydroxyzine_hydrochloride |
Diphenhydramine |
Cyproheptadine |
Loratadine |
Desloratadine |
Fexofenadine |
Cetirizine |
| family |
Bacteroidaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Bifidobacteriaceae |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| family |
Clostridiaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Coriobacteriaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Desulfovibrionaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Enterobacteriaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Eubacteriaceae |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| family |
Fusobacteriaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Lachnospiraceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Peptostreptococcaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Porphyromonadaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Prevotellaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Ruminococcaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Streptococcaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Veillonellaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| family |
Verrucomicrobiaceae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Akkermansia |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Bacteroides |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Bifidobacterium |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Bilophila |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Blautia |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Clostridium |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Collinsella |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Coprococcus |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Dorea |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Eggerthella |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Escherichia |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Eubacterium |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| genus |
Fusobacterium |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Odoribacter |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Parabacteroides |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Peptoclostridium |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Prevotella |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Roseburia |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Ruminococcus |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Streptococcus |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| genus |
Veillonella |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Akkermansia muciniphila |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides caccae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides fragilis |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides ovatus |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Bacteroides thetaiotaomicron |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides uniformis |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides vulgatus |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bacteroides xylanisolvens |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Bifidobacterium adolescentis |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Bifidobacterium longum |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Bilophila wadsworthia |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Collinsella aerofaciens |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Dorea formicigenerans |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Eggerthella lenta |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Escherichia coli |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Fusobacterium nucleatum |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Lactobacillus paracasei |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Odoribacter splanchnicus |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Parabacteroides distasonis |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Parabacteroides merdae |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Peptoclostridium difficile |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Roseburia hominis |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Roseburia intestinalis |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
| species |
Streptococcus parasanguinis |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Streptococcus salivarius |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species |
Veillonella parvula |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
-1 |
| species_group |
Lactobacillus casei group |
-1 |
-1 |
-1 |
0 |
-1 |
-1 |
-1 |
Bottom Line
I hope this post will educate people that “all antihistamines are not the same” – both in terms of known mechanism as well as impact on the microbiome.
I am hoping to have a page done by next weekend that will allow the impact of various medications and drugs (as far as is known and published) on the microbiome.
Addendum
The reader is also taking the following in addition to help with the suspected mast cell issues:
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.