Foreword – and Reminder
I am not a licensed medical professional and there are strict laws where I live about “appearing to practice medicine”. I am safe when it is “academic models” and I keep to the language of science, especially statistics. I am not safe when the explanations have possible overtones of advising a patient instead of presenting data to be evaluated by a medical professional before implementing.
I cannot tell people what they should take or not take. I can inform people items that have better odds of improving their microbiome as a results on numeric calculations. I am a trained experienced statistician with appropriate degrees and professional memberships. All suggestions should be reviewed by your medical professional before starting.
Back Story
Typical for ME/CFS, fatigue and brain fog prevented much of a backstory. Fortunately, she was able to complete symptoms — which gives a good back story and also shows overlaps with many others:
- Neurocognitive: Brain Fog [482 samples]
- General: Fatigue [442 samples]
- Sleep: Unrefreshed sleep [388 samples]
- Neuroendocrine Manifestations: worsening of symptoms with stress. [367 samples]
- Neurocognitive: Difficulty paying attention for a long period of time [360 samples]
- Neurocognitive: Can only focus on one thing at a time [341 samples]
- Neurological-Audio: Tinnitus (ringing in ear) [331 samples]
- Neurological-Audio: hypersensitivity to noise [309 samples]
- Gender: Female [299 samples]
- DePaul University Fatigue Questionnaire : Fatigue [297 samples]
- Immune Manifestations: general malaise [295 samples]
- Onset: 2010-2020 [285 samples]
- DePaul University Fatigue Questionnaire : Unrefreshing Sleep, that is waking up feeling tired [268 samples]
- Neurological: Difficulty reading [253 samples]
- General: Depression [242 samples]
- Post-exertional malaise: Worsening of symptoms after mild physical activity [230 samples]
- Post-exertional malaise: Physically tired after minimum exercise [226 samples]
- Neuroendocrine Manifestations: cold extremities [224 samples]
- Post-exertional malaise: Muscle fatigue after mild physical activity [223 samples]
- Post-exertional malaise: Post-exertional malaise [215 samples]
- Official Diagnosis: Allergic Rhinitis (Hay Fever) [211 samples]
- Neuroendocrine Manifestations: intolerance of extremes of heat and cold [208 samples]
- Post-exertional malaise: Inappropriate loss of physical and mental stamina, [205 samples]
- Official Diagnosis: Chronic Fatigue Syndrome (CFS/ME) [201 samples]
Analysis
Following my usual path My Profile/Overview found an over population of rare bacteria and under population of common bacteria. This is important to note because most clinical studies focused on shifts of common bacteria, and exclude rare bacteria (sample sizes and lack of sufficient statistical training are the typical cause).

Dr. Jason Hawrelak’s criteria came in at 56%ile, not any clear issues, with the following main items of note:
- Akkermansia -none, which suggests Akkermansia Probiotics (which persists up to 30 days – from conversations with their staff)
- Bacteroides – significant overgrowth
I looked at a new feature to see the area of imbalances, and too much production of compounds is evident.

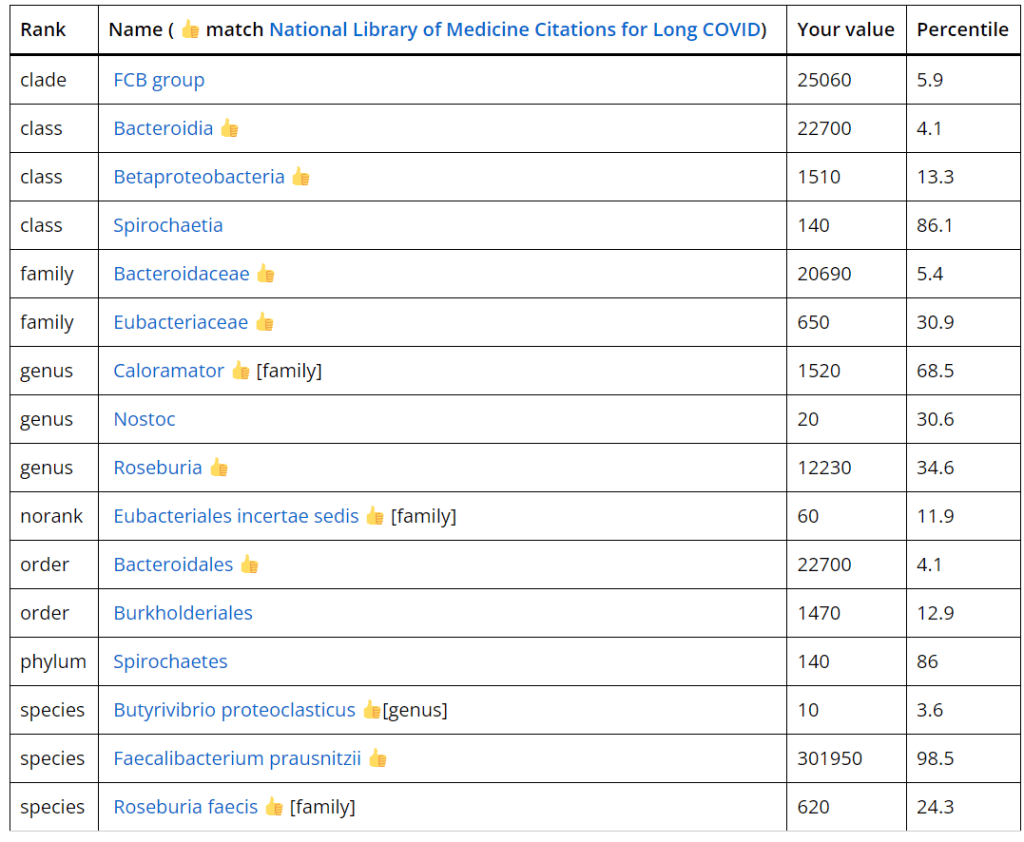
Looking at My Profile/Visualization/Microbiome Tree for colored items (and drilling down to the lowest level that are highlighted:
- Insolitispirillum peregrinum (which makes up almost 99% of Alphaproteobacteria)
- Under Bacteroides, the following stands out
- Faecalibacterium prausnitzii is high (97%ile)
- Caloramator mitchellensis is border line concern (high)
My first analysis in building a consensus report is hand picking the above and seeing the results.
The top items are similar to other ME/CFS suggestions and repeats my often refrain “Have barley porridge with walnuts” sweeten with sucralose for breakfast each day:
WARNING ABOUT GLUTEN-FREE MIS-INFORMATION
Research your science well:”Gluten is a complex mixture of hundreds of related but distinct proteins, mainly [in wheat] gliadin and glutenin. Similar storage proteins exist as secalin in rye, hordein in barley, and avenins in oats and are collectively referred to as “gluten.” ” What is gluten? (US National Library of Medicine)
Barley is free of glutenins and gliadins, the troublesome glutens. You may be using “All black men are criminals” reasoning. You really need to be tested for which types of gluten proteins you reactive to and not go for internet-legend that all glutens are bad.

The avoid list suggests not to use soy milk with the porridge. Red wine for ME/CFS is a very typical avoid (most ME/CFS cannot tolerate wine… I wonder why 😉 ). Let us see how much consensus we get from doing the pro-forma consensus building

We go to Changing Microbiome/Consensus Suggestions
- Use JasonH (15 Criteria) – 10 bacteria picked
- Standard Lab Ranges (+/- 2 Std Dev) – 4 bacteria picked
- Box Plot Whisker – 28 bacteria picked
- Kaltoft-Moltrup Normal Ranges – 82 bacteria picked
- Percentile in top or bottom 10 % – 83 bacteria picked
The Consensus report is attached.
And despite may ways of slicing and dicing, the same items appear as above on the top of the consensus.
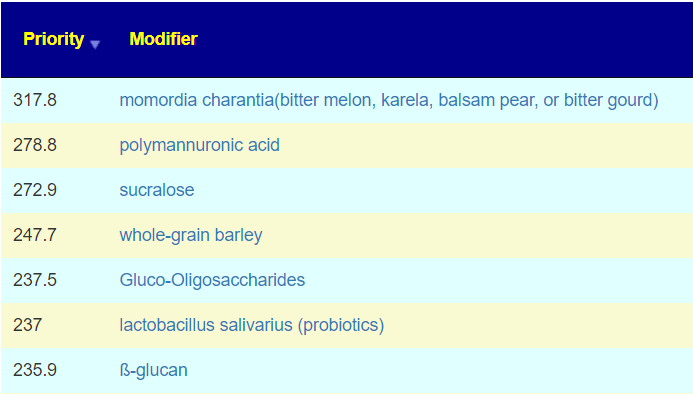

And the worst items are also similar —

Watch the types of sugars!!!
The following are popular sugar alternatives (often deemed “more healthy”) which should be avoided: stevia, saccharin, xylitol. On the best alternatives for this microbiome: sucralose (Splenda), glucose (sugar), raffinose(sugar beet).
Getting Suggestions From Symptoms
The person has entered their symptoms (see above). Unfortunately, there are many different paths that can be taken. The intent of picking bacteria by symptoms is to allow suggestions to be based on the most likely bacteria for the most troublesome symptoms for a person.
This is on Research Feature / Experimental /Build a Hand Picked collection using Symptoms. I went with the following for illustration purposes.
Picked Symptoms
- Neurocognitive: Brain Fog
- Onset: 2010-2020
- Immune Manifestations: Hair loss
- Neurological-Audio: Tinnitus (ringing in ear)
- Neurological: Joint hypermobility
I used “Expected” settings and got the following list. All of these were items with low values,

The suggestion list is very different than above:
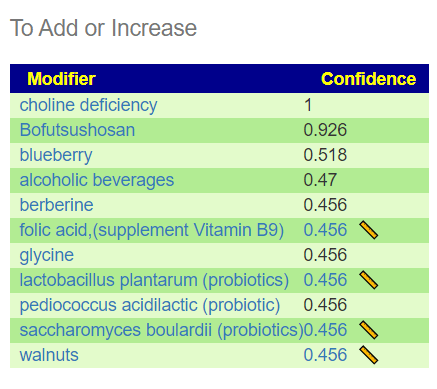
We see walnuts and for our morning porridge, add in blueberry. Bofutsushosan is very interesting because it increases AKKERMANSIA (mentioned above). I have done Bofutsushosan with Akkermansia probiotic and found a major increase in Akkermansia. Choline Deficiency means avoid foods that are HIGH in choline – see NIH List here.
The avoid list (items that will reduce the above bacteria) includes a number of probiotics:

Summing up probiotics
The following are my suggestions (2-3 weeks of doing one, then rotate to the next one)
- Akkermansia Probiotic — take with Bofutsushosan (available on Amazon etc)
- lactobacillus salivarius
- bifidobacterium infantis
- Lactobacillus plantarum
I should note that in some conference notes, ME/CFS specialists hint that random probiotics results in worsening of ME/CFS symptoms.