A reader wrote a comment and link on my Rifaximin post,
“Herbal therapy is equivalent to rifaximin for the treatment of small intestinal bacterial overgrowth”
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4030608/
The link has a table of 4 different capsules, each with different herbs. I have a working model that CFS/FM/IBS is a overgrowth of (Klebsiella, Enterobacteria, Enterococcus,Streptococcus) and very low levels of (E.Coli, Bifidobacterium, Lactobacillus) reported first in 1998.
The advantage of having a model is the ability to estimate probable impact from different herbs, spices, antibiotics etc.
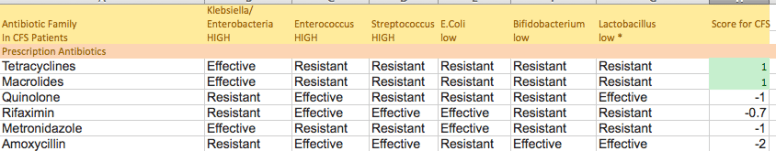
Below, I took each of the herbs and attempt to cross-reference them to their impact on the above bacteria families to see if there are specific ones that are really well suited for CFS. The score is done as follow:
- Overgrowth
- Effective 1
- No Info/Weak 0
- Resistant 0
- Undergrowth
- Effective -2
- No Info/Weak -1
- Resistant 0
Feel free to use your own formula if you disagree.
Undergrowth is more important because those bacterias as they increase will reduce the overgrowth. Killing the overgrowth will leave a vacuum which may well be repopulated with dysfunctional bacteria. The Ideal Herb or spice would be a THREE (3). The best found was a Zero (0)
You must rotate herbs, I have seen this reported in multiple studies:
“In general, the development of adaptation varied according to the bacterial strain and the essential oil … it is important to use essential oils at efficient bactericidal doses in animal feed, food, and sanitizers, since bacteria can rapidly develop adaptation when exposed to sub-lethal concentrations of these oils.” [2015]
There is a single candidate “super” herb/spice (1) . Has any one tried Thyme oil or Thyme mouth wash? Please comment.
-
Thyme (Thymus vulgaris)
The best ones (0) are:
-
Mastic Gum (Chios Mastic Mastiha) – ideally chewed in the mouth
- Neem (Azadirachta indica)
- Oregano (Origanum compactum/vulgare) – used by the person in the letter I published.
- Olive Leaf (Olea europaea)
- Pau D’Arco (Tabebuia spp)
-
Tulsi (Ocimum tenuiflorum)
The second best ones (-1) are:
- Cinnamon ( Cinnamomum verum)
- Ginger (Zingiber Officinale)
- Licorice (Glycyrrhiza glabra)
- Rhubarb (Rheum rhabarbarum)
- Sage (Salvia officinalis)
- Thyme (Thymus vulgaris)
- Wormwood (Artemisia)
The chart is based on whatever could be found. In some cases, some strains were killed and others were resistant. Your response will likely vary to each of the above.
For CLARITY to the brain fogged
- 3 VERY VERY GOOD
- 1 Unusually Good
- 0 Recommended
- -1 Acceptable
- -2 You may be doing more harm than good
- -3 You are shooting craps — we have no solid information on what will happen
- -4 You are probably harming yourself
- -5 You are making yourself worst!
There is an excellent article on more unusual Indian herbs. “The millenarian use of these plants in folk medicine suggests that they represent an economic and safe alternative for treatment of Urinary Tract Infections.” As well as this article.
The Image:

The Table
|
Herb |
Klebsiella/ Enterobacteria |
Enterococcus |
Streptococcus |
E.Coli |
Bifidobacterium |
Lactobacillus |
Score for CFS |
|
Acacia Catechu |
Effective |
Resistant |
Effective |
Effective |
no info |
no info |
-2 |
|
Amur Cork Bark (Philodendron bark) |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
Chinese goldthread (coptis chinensis – berberine) |
Effective |
Effective |
Weak |
Effective |
Effective |
Resistant |
-1.5 |
|
Chinese Skullcap (Scutellaria baicalensis) |
no info |
no info |
no info |
no info |
no info |
Resistant |
-2 |
|
Cinnamon ( Cinnamomum verum) |
Effective |
Effective |
Effective |
Weak |
no info |
Effective |
-1 |
|
Clove (Syzygium aromaticum) |
Effective |
Effective |
Effective |
Effective |
no info |
Effective |
-2 |
|
Dill Seed (Anethum graveolens) |
Resistant |
Weak |
No Info |
Weak |
no info |
Effective |
-5 |
|
Garlic (Allium sativum) |
Resistant |
Effective |
Effective |
Effective |
Effective |
Effective |
-4 |
|
Ginger (Zingiber Officinale) |
Resistant |
Weak |
Effective |
Effective |
Resistant |
Resistant |
-1 |
|
Guduchi (Tinospora cordifolia) |
Effective |
no info |
no info |
Effective |
no info |
no info |
-3 |
|
Haritaki (Terminalia chebula) |
Effective |
Effective |
Effective |
Effective |
no info |
Effective |
-2 |
|
Horse Tail (Equisetum arvense) |
Effective |
no info |
Effective |
Effective |
no info |
no info |
-2 |
|
Indian Barberry (Berberis aristata – Berberine) |
Effective |
Effective |
Weak |
Effective |
Effective |
Resistant |
-2 |
|
Lemon Balm(Melissa officinalis) |
Resistant |
no info |
no info |
Effective |
no info |
no info |
-4 |
|
Lemon grass (Cymbopogon citratus) |
Effective |
Effective |
Effective |
Effective |
no info |
Effective |
-2 |
|
Licorice (Glycyrrhiza glabra) |
Resistant |
Effective |
Effective |
Resistant |
no info |
Effective |
-1 |
|
Mastic Gum (Chios Mastic Mastiha) |
Effective |
Effective |
Effective |
Effective |
no info |
Resistant |
0 |
|
Neem (Azadirachta indica) |
Effective |
Effective |
Effective |
Effective |
no info |
Resistant |
0 |
|
Olive Leaf (Olea europaea) |
Effective |
Effective |
Effective |
Effective |
no info |
Resistant |
0 |
|
Macassar Kernels (Brucea Javanica) |
no info |
no info |
Effective |
no info |
no info |
no info |
-2 |
|
Oregano (Origanum compactum/vulgare) |
Effective |
Effective |
Effective |
Resistant |
no info |
Effective |
0 |
|
Pau D’Arco (Tabebuia spp) |
Effective |
no info |
no info |
Weak |
Resistant |
Resistant |
0 |
|
Picrasma Excelsa |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
pinyin (Hedyotis Diffusa) |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
Pulsatilla Chinensis |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
Rhubarb (Rheum rhabarbarum) |
no info |
no info |
Effective |
Effective |
Resistant |
Resistant |
-1 |
|
Rosemary (Rosmarinus officinalis) |
Resistant |
Weak |
Effective |
Effective |
no info |
Effective |
-3 |
|
Sage (Salvia officinalis) |
Resistant |
Effective |
Effective |
Resistant |
no info |
Resistant |
-1 |
|
Sida cordifolia |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
Silver |
Resistant |
Effective |
Effective |
Resistant |
Effective |
Effective |
-2 |
|
Stemona Sessilifolia |
no info |
no info |
no info |
no info |
no info |
no info |
-3 |
|
Thyme (Thymus vulgaris) |
Very Effective |
Very Effective |
Effective |
Resistant |
no info |
no info |
1 |
|
Tulsi (Ocimum tenuiflorum) |
Effective |
Effective |
Effective |
Effective |
no info |
Resistant |
0 |
|
Winter Savory(Satureja montana) |
No in |
no info |
Effective |
Effective |
no info |
no info |
-3 |
|
Wormwood (Artemisia) |
Resistant |
Resistant |
Effective |
Effective |
Resistant |
Resistant |
-1 |
|
Yarrow (Achillea millefolium) |
Effective |
no info |
Weak |
Effective |
no info |
Resistant |
-2 |