- “A recent study by Forslund et al. (1) adds another dimension for consideration by illustrating how medications may adversely affect the microbiome—an interaction often overlooked in post hoc analyses of disease-microbe relationships.” [2015]
- “Early-life antibiotic use is associated with increased risk for metabolic and immunological diseases, and mouse studies indicate a causal role of the disrupted microbiome. However, little is known about the impacts of antibiotics on the developing microbiome of children. Here we use phylogenetics, metagenomics and individual antibiotic purchase records to show that macrolide use in 2-7 year-old Finnish children (N=142; sampled at two time points) is associated with a long-lasting shift in microbiota composition and metabolism. The shift includes depletion of Actinobacteria, increase in Bacteroidetes and Proteobacteria, decrease in bile-salt hydrolase and increase in macrolide resistance. Furthermore, macrolide use in early life is associated with increased risk of asthma and predisposes to antibiotic-associated weight gain. Overweight and asthmatic children have distinct microbiota compositions. Penicillins leave a weaker mark on the microbiota than macrolides. Our results support the idea that, without compromising clinical practice, the impact on the intestinal microbiota should be considered when prescribing antibiotics.” [2016]
- Mother’s Microbiome Shapes Offspring’s Immunity [2016]
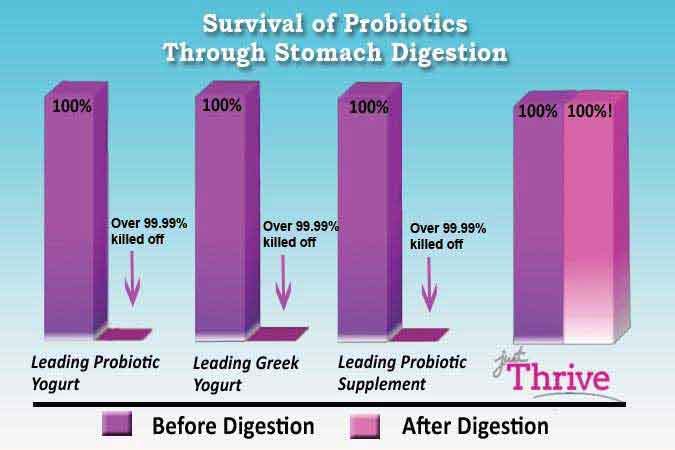
- Thrive Probiotics – Claims that the bacteria produce antioxidants as well as that 100% survives (which is because they are all bacillus). Contains:
- Bacillus Subtilis HU58 ” Two isolates of B. subtilis examined here were HU58, a human isolate and PXN21, a strain used in an existing commercial product. Compared to a domesticated laboratory strain of B. subtilis both isolates carried traits that could prove advantageous in the human gastro-intestinal tract. This included full resistance to gastric fluids, rapid sporulation and the formation of robust biofilms.” [2012]
- Bacillus Indicus HU36 “Recently isolated spore-forming pigmented marine bacteria Bacillus indicus HU36 are sources of oxygenated carotenoids with original structures (about fifteen distinct yellow and orange pigments with acylated d-glucosyl groups)” [2015] ” Overall, carotenoids from Bacillus indicus HU36 and Bacillusfirmus GB1 were found to be interesting antioxidants to fight postprandial oxidative stress in the stomach” [2013]
- Bacillus Clausii – strain is not identified, another probiotic does: Enterogermina
- Bacillus Coagulans
- Note: Expensive and no studies for FM/IBS/CFS for the species or strains.
- “Increased proportions of the Fusobacteriaceae family correlated with increased disease activity and levels of C-reactive protein in patients with UC who underwent pouch surgery. In contrast, proportions of Faecalibacterium were reduced in patients with pouchitis vs controls; there was a negative correlation between proportion of Faecalibacterium and level of C-reactive protein. There was an association between antibiotic treatment, but not biologic or immunomodulatory therapy, with reduced proportions of 11 genera and with increased proportions of Enterococcus and Enterobacteriaceae.” [2016]
- “Gut microbes produce a chemical that enhances clotting in the arteries, increasing the risk of heart attack and stroke.” [2016] … i.e. hypercoagulation!
- ” But with hundreds of microbial species crammed together in tight quarters, new research suggests that our intestinal innards might resemble a battlefield more than a conference room. Researchers have found that gut bacteria continually wage war on their neighbors, perhaps as a way to stake out space. The team injected different strains of Bacteroides fragilis, the species of gut-dwelling bacteria (pictured here), into mice that lacked their own microbes. When they analyzed the rodents’ stools over time, they found evidence that the strains were attacking each other. Different strains of B. fragilis inject different combinations of toxins into neighboring bacteria. Bacteria within the same strain fight back: They’re immune to the toxins secreted by their strain-mates. But different species or strains of bacteria can succumb to the assault, giving the attacking strain more room to spread out.” [2016]
- Pylopass, a non-viable L.Reuteri probiotic (i.e. killed) [2013] was found effective against H. Pylori.
- “Iron replacement therapy in patients with inflammatory bowel disease alters gut microbiota depending on how it is administered, suggest scientists… oral treatment (instead of IV) was associated with decreased abundances of operational taxonomic units assigned to the species Faecalibacterium prausnitzii, Ruminococcus bromii, Dorea sp. and Collinsella aerofaciens.” [2016]
- “A chronic lack of dietary fibre has been found to reduce the diversity of bacteria in the guts of mice. This effect is not fully reversed when fibre is reintroduced, and increases in severity over multiple generations” [2016]
- “Smart gas sensing pills developed at RMIT University can measure intestinal gases inside the gut and send the data directly to a mobile phone.” [2016]
“In the United States, the described benefit of a substance impacts how it is regulated. In the case of beneficial bacteria (i.e., probiotics),
- if the probiotic is added to food “primarily for taste, aroma or nutritive value” but also providing an added beneficial effect to a healthy individual, the probiotic will be regulated as a food.4
- If the probiotic is marketed to help maintain the structure or function of the body and to “supplement” the diet, the probiotic will generally be considered a dietary supplement (when labeled according to dietary supplement labeling regulations) and the associated claim is termed a “structure/function” claim. A structure/function claim does not need pre-market approval, but does need to be substantiated with “competent and reliable” scientific evidence proving the claim is “truthful and not misleading.”5 Recent claims indicate a wide variety of effects of consumed probiotics on the body, including effects on the skin that consumers regard as a “cosmetic” effect.6 Probiotics have also been added directly to cosmetic products to modulate the cutaneous microbiota.7 However, cosmetic manufacturers must keep in mind that any product that affects the structure or function of the body when applied to the skin is considered a drug, and therefore claims for cosmetics must be limited to the beautifying or attractiveness effects.8
- In general, claims for foods and dietary supplements that discuss the nutritive value or maintenance of the body do not need pre-market approval, but claims that relate a food or dietary supplement ingredient to the reduction in risk of a disease, termed “health claims,” do require pre-market approval by FDA, which regulates claims stated on food and dietary supplement labels.
- However, if a probiotic is claimed to “prevent, treat, cure or mitigate” disease, the probiotic will be regulated as a drug and the associated claim is a drug claim. Even if a probiotic is added to a food product or dietary supplement, but the claims on the packaging (or other media such as websites or social media) state the probiotic prevents or treats disease or symptoms characteristic of a disease, then FDA or FTC, the latter of which has jurisdiction over advertisements for food, drugs and medical devices, would consider the probiotic a “biologic” drug, and therefore misbranded as a food or dietary supplement.” [2016] This is why Mutaflor is deemed a drug in the US. It also means any effective probiotic for CFS/IBS/FM may end up being deemed a (prescription) drug in the US.
