A reader wrote with positive results:
“Ever since I developed Sjogren’s, I started researching a method to get back to normal. One of the more interesting studies in Pubmed I came across was the use of Vancomycin to manipulate the gut biome for autoimmune recovery, so naturally, I had to try this.
https://www.ncbi.nlm.nih.gov/pubmed/11083284
Since Vancomycin pretty much stays in the gut similar to Rifaximin, it tends to be safer than most other antibiotics, so I decided to use 250 mg 4 times daily for 14 days, as per a study that was recently run by NYU in another autoimmune related study.”
- “Vancomycin became available for clinical use >50 years ago but was soon discarded in favor of other antibiotics that were deemed to be more efficacious and less toxic.” [2006 – full text, review of the history of vancomycin]
- “Prior to its release, vancomycin was used to treat an entity called “postoperative micrococcal colitis” [2]. The response to vancomycin was excellent, and the presence of this disease, also called “acute staphylococcal ileocolitis,” became an indication for the use of vancomycin [29]. Although Clostridium difficile is the primary agent of pseudomembranous enterocolitis, Staphylococcus aureus is clearly an occasional cause of the disorder [30]. Because vancomycin is active against both pathogens and is poorly absorbed from the intestinal tract, it became the drug of choice for treating pseudomembranous enterocolitis [31]”
- “With the increased use of vancomycin came data suggesting that vancomycin might not be equivalent to β-lactams.”
- “[In Rats] Vancomycin significantly altered the microbiota, which was restored to control levels by 8 weeks of age. Notably, vancomycin-treated animals displayed visceral hypersensitivity in adulthood without any significant effect on anxiety responses as assessed in the elevated plus maze or open field tests... a temporary disruption of the gut microbiota in early-life results in very specific and long-lasting changes in visceral sensitivity in male rats, a hallmark of stress-related functional disorders of the brain-gut axis such as irritable bowel disorder.” [2014]
- Visceral hypersensitivity means a general increase in pain sensation experienced in internal organs. It is common in IBS sufferers. [source]
- “In patients experiencing an acute episode of recurrent Clostridium difficile infection (CDI), a single Fecal transplantation by enema was not significantly different from oral vancomycin taper in reducing recurrent CDI. ” [2017] – in other words, it may be as effective as a fecal transplant… more studies are needed.
- “To date fecal transplant cures Clostridium difficile infections with more efficacy than vancomycin, and prevents recurrence.” [2015]
- Short- and long-term effects of oral vancomycin on the human intestinal microbiota [2017]. FULL TEXT
- “oral vancomycin remains the treatment of choice for severe C. difficile infection (CDI). Despite its effectiveness against CDI (cure rate of ∼90%),”
- “microbiota alterations induced by vancomycin may promote intestinal colonization by other pathogens, including VRE, Klebsiella pneumoniae or Escherichia coli.10Moreover, oral vancomycin therapy may predispose to other microbiota-related disorders, including obesity, asthma or diabetes.7,11,12“
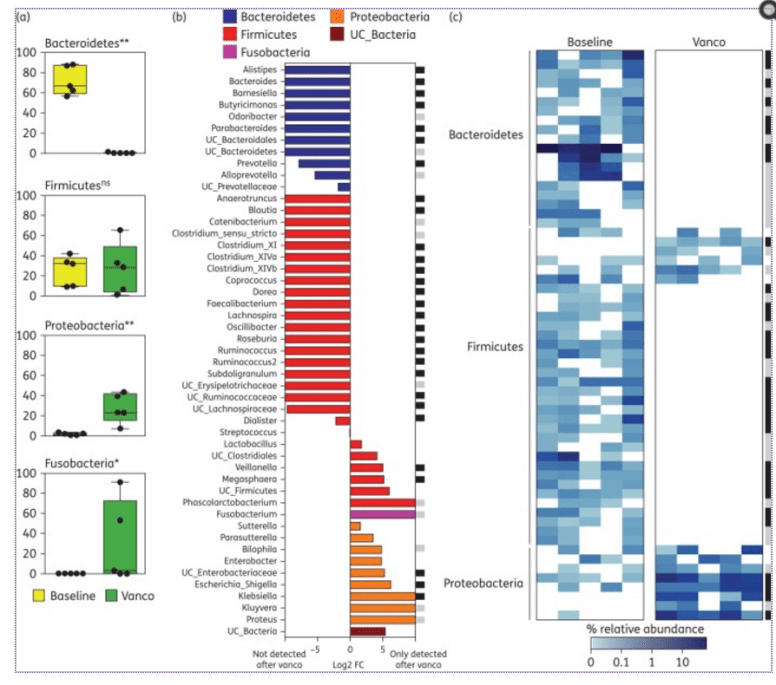
- “By contrast, microbiota richness was greatly reduced upon vancomycin administration. Following antibiotic cessation, microbiota richness gradually increased, although it never recovered to baseline levels. A similar result was obtained when the Shannon diversity index was calculated (Figure 1c and Figure S3), which takes into account the number of OTUs and their relative proportion. In this case, however, baseline levels were recovered 22 weeks after antibiotic withdrawal.”
Bottom Line
Vancomycin seems close to doing a disk format and re-install of the operating system on a PC. You need to reinstall all of your programs (i.e. populate with probiotics) — unfortunately you no longer have most of the installation disks….
If you do use Vancomycin, I would strongly suggest having as many human-sourced probiotics as possible on hand, and start them 2-6 days after the last dosage, for example:
- Symbioflor-2
- Mutaflor
- Lactobacillus Fermentus ME3
- Biogaia Lactobacillus Reuteri
- Enterococcus faecium SF68
As well as these SBO
- Prescript Assist
- General Biotics Equilibrium
