Tetracyclines includes minocycline, doxycycline and other brand names. In this post, I am revisiting what we currently know about the shifts of the microbiome as a result.
My last post on Va In this pncomycin had me discovering some lovely graphics on the shift of the microbiome.
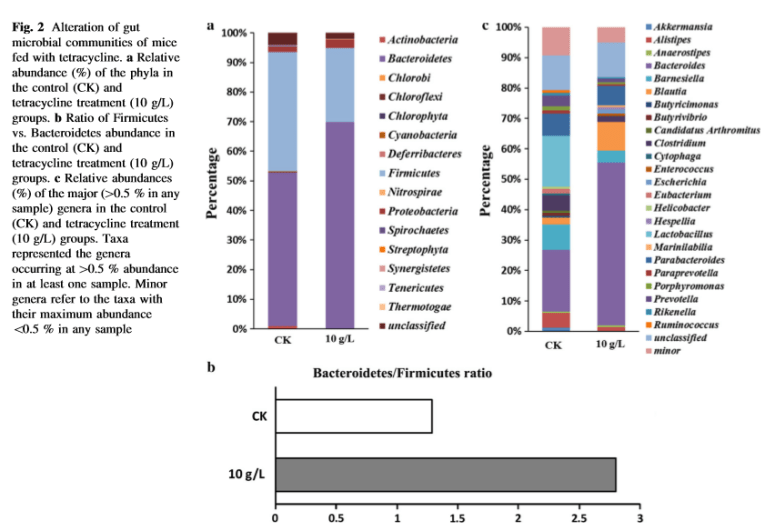
From Metagenomic insights into tetracycline effects on microbial community and antibiotic resistance of mouse gut[2015]. we have the following graphics
Studies of tetracycline on CFS/FM/IBS
- “After 4-12 months they developed post-Q-fever fatigue syndrome and were treated with intracellular active antibiotics (fluoroquinolones and tetracycline) for 3-12 months. Efficacy of the treatment was observed in two patients, but in one patient the results were not encouraging.” [2007]
- “Four CFS patients (the CFS group) and 54 controls [the post-Q fever fatigue syndrome (QFS) group] positive for C. burnetii were treated mainly with minocycline or doxycycline (100 mg/day) for 3 months. After treatment, all 58 patients tested negative for C. burnetii infection.” [2005]
- “These results of an open label study in Japan suggest that minocycline administration is useful for improving chronic nonspecific symptoms considered to be post-Q fever fatigue syndrome caused by C. burnetii infection.” [2004]
- “post-Q fever chronic fatigue syndrome has been described. … the treatment of choice for acute infection in both diseases is still tetracycline-group antibiotics.” [2007]
- Used by Prof. Garth L. Nicolson
- “the recommended treatments for mycoplasmal blood infections require long-term antibiotic therapy, usually multiple 6-week cycles of doxycycline (200-300 mg/d), ciprofloxacin or Cipro (1,500 mg/d), azithromycin or Zithromax (500 mg/d) and clarithromycin or Biaxin (750-1,000 mg/d). Multiple cycles are required,”
- Used by Dr. Cecile Jadin, MD. Site
