From Stockholm in 2015, we had this article: “Determining the Long-term Effect of Antibiotic Administration on the Human Normal Intestinal Microbiota Using Culture and Pyrosequencing Methods [2015]”
- Ciprofloxacin is a fluoroquinolone
- Clindamycin is a lincosamide antibiotic
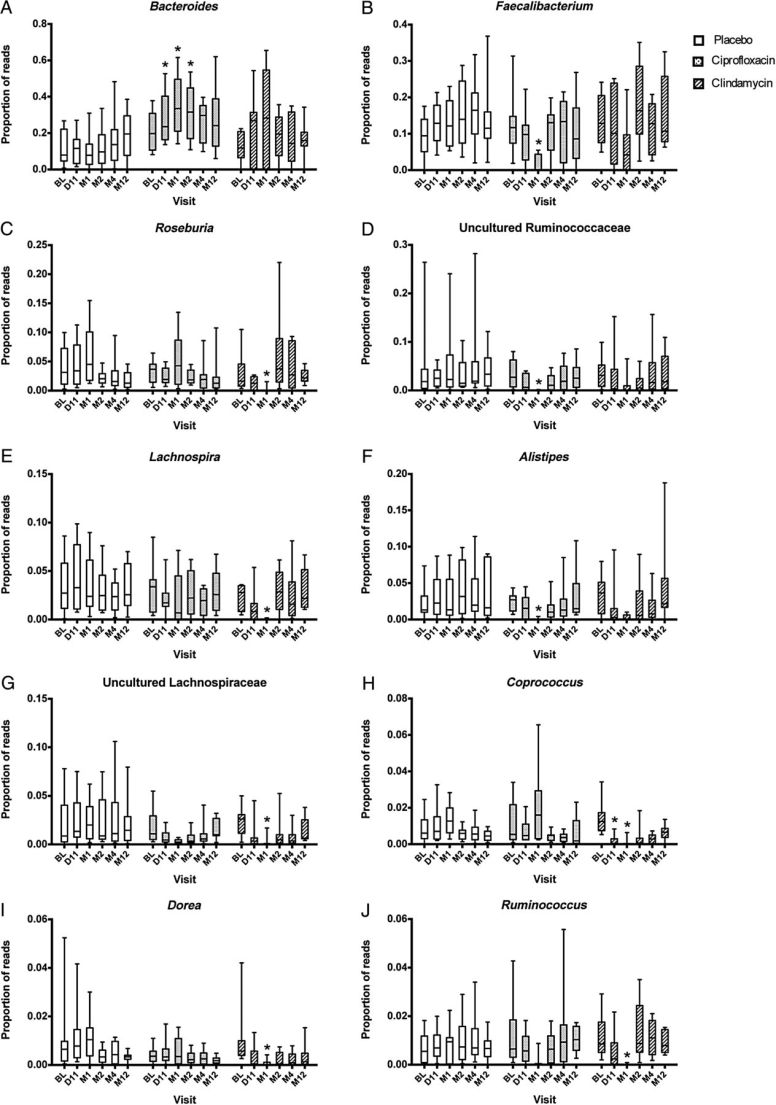
This study is interesting because you can see variation in the population of the control group over the 11 months (possibly due to season food consumption, sun exposure, etc). For some groups like Ruminococcaceae, they appear to survive well for the 10 days that the antibiotic was taken and then collapsed to nothing in the following 20 days and then returned by 2 months.
Abbreviations: BL, baseline; D11, day 11; M1, month 1; M2, month 2; M4, month 4; M12, month 12.
“Study Design
Thirty healthy volunteers aged between 18 and 45 years with normal findings in their medical history and physical examination (15 men and 15 women) were included in the study. The volunteers had undergone at least a 3-month washout period following a treatment with any systemic or topical antibiotics. Volunteers who were currently enrolled in another investigational drug or device study or who had participated in such a study in the 3 months prior to the screening visit were excluded. Twenty volunteers were randomly assigned to the treatment groups (ciprofloxacin or clindamycin) and 10 volunteers in the control group. Ten volunteers (5 men and 5 women) were given ciprofloxacin (500 mg twice daily) and 10 volunteers (5 men and 5 women) were given clindamycin (150 mg 4 times daily) for a 10-day period; the remaining 10 volunteers (5 men and 5 women) in the control group were given placebo for 10 days. Fecal samples were collected for analyses at 6 occasions: immediately before antibiotic or placebo administration, day 11 (ie, immediately after treatment), and at 1, 2, 4 and 12 months postdosing”.
Studies on CFS/FM/IBS
- Clindamycin increases risk ratio of Clostridium difficile by 44 [2008], nothing else found.
- Fluoroquinolone
- “After 4-12 months they developed post-Q-fever fatigue syndrome and were treated with intracellular active antibiotics (fluoroquinolones and tetracycline) for 3-12 months. Efficacy of the treatment was observed in two patients, but in one patient the results were not encouraging.” [2007]
- Used by Prof. Garth L. Nicolson “the recommended treatments for mycoplasmal blood infections require long-term antibiotic therapy, usually multiple 6-week cycles of doxycycline (200-300 mg/d), ciprofloxacin or Cipro (1,500 mg/d), azithromycin or Zithromax (500 mg/d) and clarithromycin or Biaxin (750-1,000 mg/d). Multiple cycles are required,”
- Used by Cecile Jadin, MD
