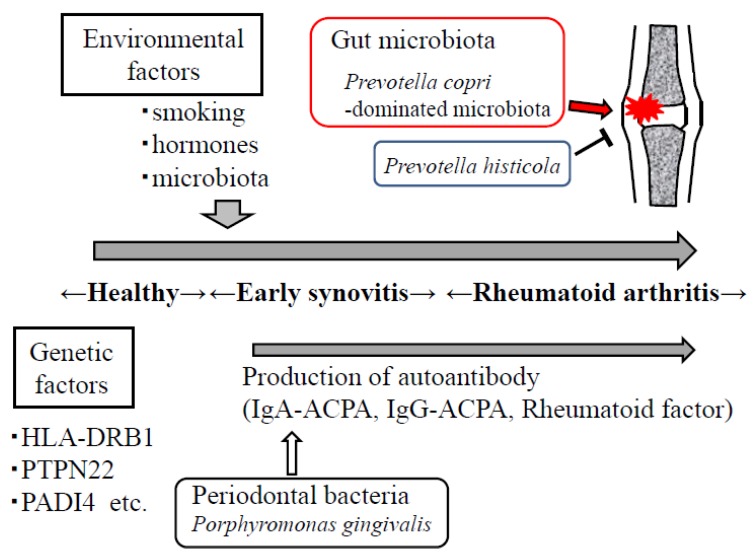
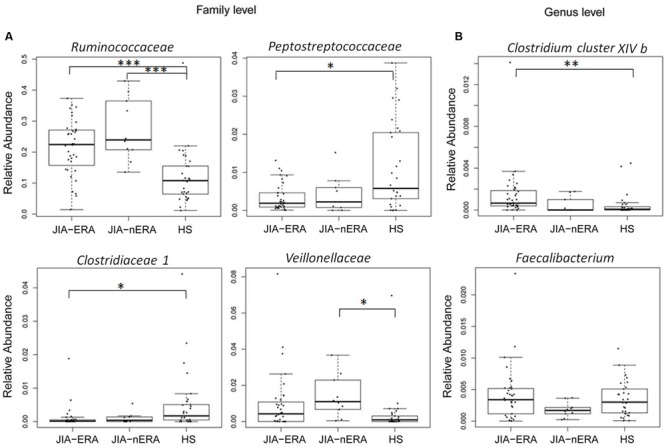
This is a theoretical post. Working from high bacteria and low bacteria cited in this earlier post, I went to DataPunk.Net and extracted information about each genus.
I have struck thru items that appear on both sides. We do not know if these items will help or make things worst…. i.e. these are should avoid for safety items.
The Increase or Decrease are what you in theory would reduce high bacteria and enhance low bacteria. In some cases, the same item will decrease the high bacteria and increase the low bacteria; in general, we have limited knowledge from published articles.
| High Bacteria | Low Bacteria |
|---|---|
|
|
| To Improve Decrease Intake of |
To Improve Increase Intake of |
|
|
For caution, we should ignore items that impact only one of the bacteria. We want items that impact several bacteria.
Bottom Line
Some of the increased items above appears to be backed by the literature:
- Effect of ω-3 polyunsaturated fatty acids on arthritic pain: A systematic review [2017].
- “ω-3 PUFAs may have a therapeutic role in decreasing pain associated with RA, with doses of 3 to 6 g/d appearing to have a greater effect”
There were some pleasant surprises above…
- On the right there are a lot of sugar substitutes (Saccharin, Stevia, Sucralose / Splenda)…. and evidence is that they reduce risk of RA! They may also reduce the severity (speculation)
- “Regular consumption of sugar-sweetened soda, but not diet soda, is associated with increased risk of seropositive RA in women, independent of other dietary and lifestyle factors.” [2014]
- Resistant starch Types I,II,III are all should be reduced while Type IV should be increased.
-
- “Dietary modulation of the gut microbiota impacts human health. Here we investigated the hitherto unknown effects of resistant starch type 4 (RS4) enriched diet on gut microbiota composition and short-chain fatty acid (SCFA) concentrations in parallel with host immunometabolic functions in twenty individuals with signs of metabolic syndrome (MetS). Cholesterols, fasting glucose, glycosylated haemoglobin, and proinflammatory markers in the blood as well as waist circumference and % body fat were lower post intervention in the RS4 group compared with the control group. 16S-rRNA gene sequencing revealed a differential abundance of 71 bacterial operational taxonomic units, including the enrichment of three Bacteroides species and one each of Parabacteroides, Oscillospira, Blautia, Ruminococcus, Eubacterium, and Christensenella species in the RS4 group. Gas chromatography–mass spectrometry revealed higher faecal SCFAs, including butyrate, propionate, valerate, isovalerate, and hexanoate after RS4-intake. “[2016]
- This was a human study and used 30% RS4 enriched flour.
- One source.
- “Dietary modulation of the gut microbiota impacts human health. Here we investigated the hitherto unknown effects of resistant starch type 4 (RS4) enriched diet on gut microbiota composition and short-chain fatty acid (SCFA) concentrations in parallel with host immunometabolic functions in twenty individuals with signs of metabolic syndrome (MetS). Cholesterols, fasting glucose, glycosylated haemoglobin, and proinflammatory markers in the blood as well as waist circumference and % body fat were lower post intervention in the RS4 group compared with the control group. 16S-rRNA gene sequencing revealed a differential abundance of 71 bacterial operational taxonomic units, including the enrichment of three Bacteroides species and one each of Parabacteroides, Oscillospira, Blautia, Ruminococcus, Eubacterium, and Christensenella species in the RS4 group. Gas chromatography–mass spectrometry revealed higher faecal SCFAs, including butyrate, propionate, valerate, isovalerate, and hexanoate after RS4-intake. “[2016]
-
For magnesium (where for CFS/FM in general, more is better) we have the opposite being suggested above, that is reduce it!!. Looking at studies — a reduced level appear to help RA.
This is the second time that we observed: microbiome shift seen in an autoimmune condition–> what corrects the shift –> studies confirm the suggestions improves the condition.
As always consult with your medical professional before changing diet or supplements. The above considers the condition is isolation of other conditions that may be a factor.