A reader asked “My question is, do you have any source where it shows which strain does the allicin(garlic) kill?”
I will answer this question by showing the steps that I took to answer it.
- https://www.wikipedia.org/ and enter the name – you want to get the various brand names that it may have. In this case it is easy: {garlic,allicin}
- Go to PubMed. and start with a wide search:
- (garlic OR allicin) and bacteria
- My results had over 600 hits.
- Start scanning the titles and making notes, I usually add the Uri to the article for future reference, often the title is enough, sometimes opening the links will get good details.
General Results
- Effective on “Infectious bronchitis virus (IBV) is a coronavirus.” http://www.ncbi.nlm.nih.gov/pubmed/27516987
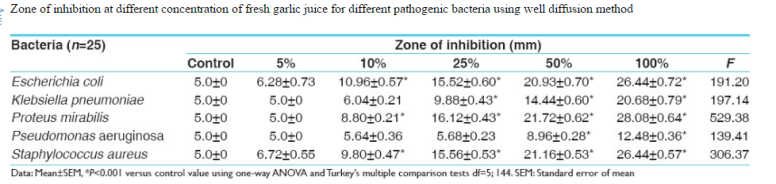
- Antimicrobial activity of fresh garlic juice: An in vitro study.
- Antifungal activity, kinetics and molecular mechanism of action of garlic oil against Candida albicans.
- Inhibition of streptococcal pyrogenic exotoxin B using allicin from garlic.
- Anti-microbial efficacy of Allium sativum extract against Enterococcus faecalis biofilm and its penetration into the root dentin: An in vitro study.
- The Effects of Allium sativum Extracts on Biofilm Formation and Activities of Six PathogenicBacteria.
- “Sandasi (16) confirmed the inhibitory effects of A. sativum L. extracts against planktonic forms and biofilm formation of Candida albicans, Listeria monocytogenes and P. aeruginosa.”
Specific Results
If you want to know if it will impact Lactobacillus bacteria (i.e. probiotics):
(garlic OR allicin) and lactobacillus
which returned 37 hits.
- “The inhibition zones of the different concentrations of garlic extract were not significantly different for S. mutans, S. sanguis, and S. salivarius. For P. aeruginosa and lactobacillus spp. the inhibition zones of 5%, 10% and 20% concentrations were not significantly different from one another,” Antibacterial effect of different concentrations of garlic (Allium sativum) extract on dental plaque bacteria.
- Effect of garlic powder on the growth of commensal bacteria from the gastrointestinal tract. “While for most bacteria the antimicrobial effect was transient, the lactobacilli showed a degree of resistance to garlic, indicating that its consumption may favour the growth of these beneficial bacterial species in the gut. Garlic intake has the potential to temporarily modulate the gut microbiota.”
- “The impact of these extracts on the growth of selected probiotic bacteria (Lactobacillus reuteri, Lactobacillus rhamnosus, Bifidobacteria lactis) and pathogenic bacteria (Escherichia coli 0157:H7 and Escherichia coli LF82) was assessed using a standard minimum inhibitory concentration method. The results showed that aqueous extractions of garlic and black peppercorns significantly enhanced the growth of one strain of probiotic bacteria (L. reuteri) whilst inhibiting both pathogenic strains of E. coli at a 1:50 dilution.” In vitro effects of food extracts on selected probiotic and pathogenic bacteria.
No results can happen
Since is high in CFS and is also associated with histamine production, I tried the following search:
(garlic OR allicin) and Morganella
There were no results.

