This is my second enhanced uBiome analysis. The main difference is that I no longer rely only on DataPunk.Net data but have extended that by reviewing more recent studies on PubMed etc.
Patient Background
Travel to the US in 2013 and got a difficult virus, returned home
- took 4 weeks to recover
- start exercising/working as soon as I felt a little better
- exercise/work too hard, get sick again
- Then ME/CFS symptoms arose
- 3 months later I’m slowly getting better
- Then get a stomach bug with all sorts of weird symptoms
- Can’t sleep
- constipation with a lot of gas
- Cortisol starts crashing
- lots of fatigue
- brain fog gets worse and worse
- Tried all remedies under the moon
- eventually try fecal transplants, and symptoms start improving
- sleep & energy production especially
- increased energy
- can work and exercise again
- but cognitive problems still very strong
- spect scan shows bad results
- brain doesn’t look good
- bad blood flow in a lot of areas.
CFS Diagnosis confirmed by one of Europe’s leading CFS Researchers/MD.
Standard Items
- Diversity: 25%ile (much lower than most CFS patients who are 90%ile or higher)
- Bifidobacterium: 0.28x (much higher than most CFS patients, but still low)
- Lactobacillus: 0.01x – typical very low or none
- E. Coli: Usually inferred from
This set of improvements agrees with the improvements he described above.
Hit List for Bacteria
Prime List
Bacteria > 1.5x all samples
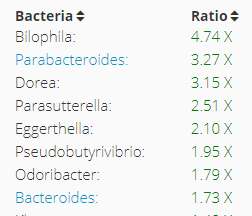
Items with {X} below were also see as abnormal on their RED Metagenomics Stool Analysis Report done earlier. {-} indicated normal. {?} indicated not tested.
So 50% of the genus reported by uBiome are NOT reported by RED test. Only 25% of those tested by both were in agreement.

The transplant etc could account for the difference (they were not done at the same time). I would put greatest emphasis on the bacteria genus in common with both of tests: Dorea https://atomic-temporary-42474220.wpcomstaging.com/2017/10/18/reducing-dorea-genus/
Avoid
Take
Secondary List
Bacteria that are found in < 5% of samples

Bottom Line Theoretical Items
The lists below are done by merging the lists from the deep dives. Some items may encourage one genus and discourage another genus — those are placed in inconclusive. The impact on Lactobacillus, Bifidobacterium and E.Coli are intentionally ignored[See this post for the logic]. This is all based on applying logic to the results of studies — thus theoretical.
Inconclusive:
In general, should try to avoid (helps some, inhibits some — we do not know the balance). These could be tried in isolation to other changes to infer their impact on your own uBiome.
Avoid:
Take:
- Lactobacillus reuteri
- Lactobacillus kefiri
- Lactococcus lactis
- Bacillus licheniformis
- Bifidobacterium bifidum
- Possibly: B. infantis, B. adolescentis or B. breve
- L-glutamine
- β-glucan
- Vitamin C
- Black Tea
- Tea Tree Oil
- Oral Iron Supplements
- Flaxseed
- Capsaicin (chili peppers)
- high-fat diet
- Ketogenic diet
- Vitamin D3
- Metronidazole antibiotics
- Alchohol
- Oligosaccharide prebiotics
- Walnut
- Sucralose (Splenda)
- Garlic
- Chitosan
- Tea
- Cinnamon,
- Lemongrass,
- Oregano,
- Clove
Personal Note
This reader brain’s scans sounds very much like what my own SPECT scan, and my daughter’s (done by Dr. Daniel Amen) saw. What helped me the most with brain fog actually came from a Russian study of pilot functioning in low oxygen: heparin and piracetam taken together. Regular heparin (low dosage) is taken sublingual (instead of injection) and held in the mouth for 2-4 minutes and then spitted out. The heparin will improve the lactobacillus (I suspect the anticoagulant action may also apply to some bacteria) according to this [2013] study.
Other items taken for brain function was minocycline, see this post for more discussion.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of CFS or any other condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.