A European 30 y.o. reader wrote for some help. She has been treated by at least one of the top CFS physician in the world (I have actually met him at a conference), but with little joy.
Her stool revealed elevated IgA, too little bile acids, elevated PH, sugar. Bifido and Lactobacillus species were low. — so the typical CFS profile.
She has severe histamine intolerance and had tried some probiotics (they were not named).
When the gut bacteria shifted into the histamine intolerance zone, it is currently a treatment nightmare — mainly because there is so little useful information!
With that said, I am going to research a draft model and then find as much information that may be helpful with the model for treatment. This is speculation.
Model
Assumptions:
- Histamine intolerance is the result of a shift of bacteria.
- It may be either a decrease of DAO bacteria or their helpers/suppliers or an increase of histamine producing bacteria.
- “These results show that some Gram negative bacteria, associated with acute exacerbations in respiratory infections, produce histamine and possibly other inflammatory mediators,” [1989]
- “A diminished histamine degradation based on a reduced diaminoxidase activity is suspected as a reason for non-IgE-mediated food intolerance caused by histamine.” [2006]
- “Bacteria induced basophil histamine release through two ways: immunological (IgE-mediated) and non-immunological (sugar-lectin interactions).” [1998]
- “Staphylococcus aureus produces numerous bi-component toxins,..and histamine release” [1997]
- “Influenza A virus, S. aureus and lipopolysaccharide from S. typhimurium increased the maximum release of histamine and caused a shift to the left of the dose-response curves showing increased cell sensitivity and lowering of the threshold to these stimuli.” [1991]
- “Histamine release induced by Staphylococcus aureus was examined in cells obtained by bronchoalveolar lavage (BAL) in non-atopic individuals. Approximately half of the individuals responded with mediator release to the bacterium, and the release was found to be time- and concentration dependent.” [1991]
- Staphylococcus aureus and influenza A virus stimulate human bronchoalveolar cells to releasehistamine and leukotrienes [1989].
- “Staphylococcus aureus, lipopolysaccharide (LPS) from Salmonella typhimurium and influenza A virus were found to enhance the histaminerelease but did not release histamine per se….These findings indicate that the enhancement of mediator release by bacteria, endotoxin, and virus depends on a sugar-mediated reaction.” [1990] – i.e. cut all sugars!
- If practical, this can be tested. Low serum DAO activity, i.e. <10 U/mL would be expected (see my DAO post). Other studies cites < 40 U/ml
- It may be either a decrease of DAO bacteria or their helpers/suppliers or an increase of histamine producing bacteria.
Background Literature
- “Histamine was first thought only to be present in mast cells, but modern research has proven that many other cells also produce histamine to varying degrees. These include white blood cells such as basophiles, platelets, certain types of gastric cells and neurons.[ 2] Furthermore, histamine has been found to be present in all tissues of the body.[ 3]” [e]
- “Reduced diaminoxidase serum levels leading to occurrence of HIT symptoms like chronic headache, dysmenorrhea, flushing, gastrointestinal symptoms, and intolerance of histamine-rich food and alcohol were significantly more common in patients with Atopic eczema than in controls.” [2006]
- “The significance of HIT in patients with atopic dermatitis in whom the benefit of a low histamine diet has been proven is becoming increasingly understood recently.” [2012]
- “Twenty patients with histamine intolerance and highly reduced initial activity of serum DAO (<40 HDU/ml) went to a histamine-free diet and after 6 to 12 months of histamine-free diet all clinical parameters and serum for determination of DAO activity were taken again….all 20 patients after the histamine-free diet the main clinical symptoms typical for histamine intolerance have disappeared. Furthermore, the measured values for activity of serum DAO have increased significantly (p<0.0001)….We can conclude that determination of DAO activity in serum is a useful diagnostic tool, together with detailed history to differentiate between food allergy and histamine intolerance. “. [2011] [2013]
- Comment: The report did not indicate that the serum DAO went to normal, only that they changed (in a positive direction was implied but not stated). Neither was it stated if the patient could stop being on a histamine-free diet.
- DNA SNPs:
- “The minor allele at rs2052129, rs2268999, rs10156191 and rs1049742 increased the risk for a reduced DAO activity…
CONCLUSIONS: DAO gene variants strongly influence DAO expression and activity but alone are not sufficient to fully effectuate the potentially associated disease state of HIT, suggesting an interplay of genetic and environmental factors.” [2011]
- So, it appears that the microbiome may be a very significant player
- “The minor allele at rs2052129, rs2268999, rs10156191 and rs1049742 increased the risk for a reduced DAO activity…
Hunting the elusive Probiotics
Conjecture: Probiotics that help Atopic eczema or atopic dermatitis[AD] are likely to help histamine intolerance.
- “The effects of probiotics in the prevention and treatment of AD remain elusive. However, evidence from different research groups show that probiotics could have positive effect on AD treatment, if any, that depend on multiple factors, such as specific probiotic strains, time of administration (onset time), duration of exposure, and dosage.” [2016]
- “Alterations in the skin microbiome may lead to increased Staphylococcus aureus colonization and atopic dermatitis progression. Despite the evidence for their important role, probiotics have not been deemed efficacious for the treatment of atopic dermatitis, although studies suggest that probiotics may be effective at preventing the development of atopic dermatitis when given to young infants.” [2015]
- “In this study, administration of the probiotic strain Lactobacillus sakei probio-65 for 2 months significantly reduced the disease severity index in experimental dogs diagnosed with Canine atopic dermatitis.” [2015]
- “the negative impact of specific TLR genotypes[DNA/SNPs] may be positively affected by probiotic supplementation. Lactobacillus rhamnosus HN001 (HN001) exhibits a much stronger effect than HN019 in this respect.” [2015]
- “the association of S. thermophilus ST10 and tara gum could improve the activity of L. salivarius LS01 administered at high doses to adults with AD….A significant improvement in SCORAD index was observed in the probiotic group after 1 month of treatment, whereas no significant changes occurred in placebo patients. A slight decrease in fecal S. aureus count was observed in probiotic-treated patients.” [2014]
- A few antihistamines appear to be effective against S.Aureus “Chlorophenoxamine hydrochloride-topical and chlorophenoxamine hydrochloride-systemic were the most effective (P < 0.05).” [2009]
- ” The stimulation of rat mast cells with Staphylococccus cohnii, Staphylococcus coagulase(-) (two strains), Ureaplasma urealyticum, Peptostreptococcus spp., Bacteroides capillosus, Staphylococcus aureus and Streptococcus agalactiae resulted in lower but significant histamine secretion (11.2%-17.5%). Other bacteria strains (Staphylococcus epidermidids, Enterococcus faecalis, Escherichia coli, Actinomyces naeslundii (two strains) and Lactobacillus fermentum (two strains) caused very low (4.2% – 8.8%) histamine release.” [2002]
- So SymbioFlor-2 (E.Coli) and Symbioflor-1 (Enterococcus faecalis) are suggested in the hope they will displace the higher producing histamine bacteria. [A few E. faecalis strains rduces S. Aureus [2014] ..
No or Low Histamine Probiotics
These are also candidates against S. Aureus.
- E. Coli – Mutaflor, Symbioflor-2
- Enterococcus faecalis – Symbiolfor-1,
- L. rhamnosus strains “are neither haemolytic nor producer of biogenic amines such as histamine, putrescine, cadaverine and tyramine.”[2014] “might diminish mast cell allergy-related activation by downregulation of the expression of high-affinity IgE and histamine receptor genes” [2011]
- Lactobacillus sakei – “Histamine decarboxylase (HDC) activity could only be detected in one L. sakei strain,” [2011] “Lactobacillus sakei CRL1862 produced neither histamine nor tyrosine and exhibited no resistance to the antibiotics assayed.” [2012]
L. Reuteri is NOT on the list
- L. Reuteri (certain strains only)= “: Lactobacillus salivarius, Lactobacillus reuteri, Lactobacillus johnsonii, Pediococcus acidilactici, and Lactobacillus paralimentarius. None of the isolates [from poultry] produced tyramine or histamine.” [2012] “hdc(+) L. reuteri, which can convert l-histidine to histamine in the gut,” [2015]
Almost all human L.Reuteri are histamine producers. See chart below from From prediction to function using evolutionary genomics: human-specific ecotypes of Lactobacillusreuteri have diverse probiotic functions[2014].
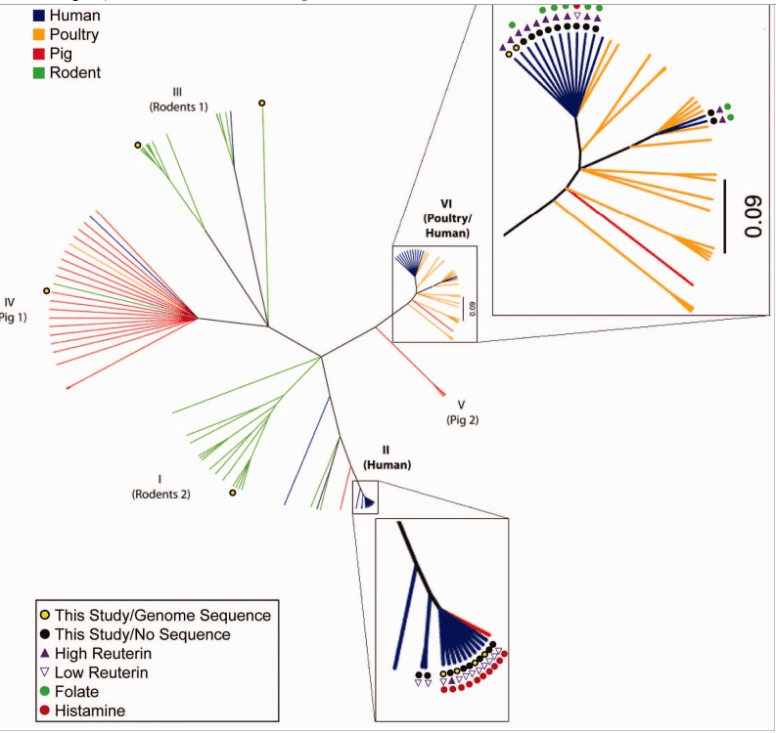
Proposed Model
It seems that some strains of Staphylococcus aureus are likely involved. See my earlier post on S. Aureus where I cite 4 specific probiotics (Propionibacterium freudenreichii, Lactobacillus reuteri,Bacillus clausii, Lb. plantarum WLPL04) as well as a list of herbs.
- Staphylococcus aureus enterotoxins induce histamine and leukotriene release in patients with atopic eczema.[2001]
- “The mechanism needs to be further understood. Staphylococcus aureus infection has a close relation with diarrhea; its cell wall component peptidoglycan (PGN) has strong biological activity on immune cells and possibly plays a role in S. aureus-induced diarrhea. The present study showed that oral PGN-induced diarrhea in mice in a dose-dependent manner. Intestinal epithelial cells absorbed PGN via the intracellular pathway. Intestinal mast cells[Histamine release] were activated after PGN gavage.” [2007]
- ” Experimental colds do not alter bacterial dispersal, but respiratory allergies multiply the effect of dispersing S. aureus.” [2006] i.e. S.aureus may have adapted to create histamines as a way of spreading..
Herbal Attack
In an earlier post I listed some herbs reported effective against S. Aureus. I am working off the assumption that some of these strains are significant players and thus need to be reduced. The problem is determining if these herbs are also histamine releasers (not good).
Information on PubMed tend to be parse, so I am relying on some histamine intolerance web sites also
- [a] https://histaminepirate.wordpress.com/about-histamine-intolerance/
- [b] http://www.foodsmatter.com/allergy_intolerance/histamine/articles/histamine_joneja.html
The list below is not comprehensive, but a good start. Each and every herb or spices should be documented to be:
- Effective against S.Aureus
- Inhibits histamine release
A third desired characteristic is that it is not in the usual herbs and supplements. Why? Because S. Aureus will have developed mutations to deal with the supplements and herbs usually taken — hence we want chemicals that have not been seen prior by the S. Aureus strains.
| L – Low A- Avoid T – Take/ Inhibits |
| Herb | Histamine | Note |
| Salvia officinalis (common sage) | L[a] | http://www.ncbi.nlm.nih.gov/pubmed/6485822 |
| Eucalyptus globulus, Tasmanian bluegum | T | http://www.ncbi.nlm.nih.gov/pubmed/11297859 |
| Coleus forskohlii, Plectranthus barbatus, Indian Coleus | T | http://www.herbal-supplement-resource.com/coleus-forskohlii.html |
| Forsythia suspensa (連翹 Lián Qiào) | T | http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4003708/ |
| Turnera diffusa, | L | http://www.tropilab.com/damianatea.html |
| Larrea tridentata | T | http://herbup.com/larrea.htm |
| Fresh Garlic | T[b] | Must be fresh |
| Cinnamon | A | https://migraine.com/blog/elimination-diet-foods-to-eat-foods-to-avoid/ |
| Black Cummin Seed | T[b] | |
| Milk Thistle | A | http://www.livestrong.com/article/333974-can-milk-thistle-cause-skin-rashes/ |
| Withania somnifera (Ashwangdha) | A | http://www.daburmediclub.com/clinicalreport/stresscom.pdf |
| Bacopa monnieri | T | https://healingherbalsnewzealand.com/bacopa/ |
| sulphoxide extracts of green chamomile tea | T[b] | |
| Turmeric | T[b] |
My suggested short list would be:
- Eucalyptus globulus, Tasmanian bluegum
- Coleus forskohlii, Plectranthus barbatus, Indian Coleus
- Forsythia suspensa (連翹 Lián Qiào)
- Larrea tridentata
Start with one for 1 week, then add the next one a week later (stopping each after 2 weeks) and keep rotating. As you see in my earlier post, all of these unusual herbs are available (typically via Swanson or Amazon).
