I have mentioned VSL#3 probiotic is passing but have not done an explicit review. I know that it is heavily promoted directly to MDs. In terms of readers’ experience…
- “taking VSL#3 (I hadn’t discovered your website yet). I switched over to Prescript Assist, and it hasn’t even been a week yet, and yesterday, for the first time in 6 months I went for a 2 mile walk/jog around my neighborhood. My mono symptoms have disappeared.” [2017]
So what is known about VSL#3 from clinical studies ideally. There are 250+ citations on PubMed, so it is well studied. It is helpful for some conditions and many MDs will suggest it blindly for any issue dealing with the microbiome or digestion.
Not Specific to CFS/IBS/FM
- The Probiotic Compound VSL#3 Modulates Mucosal, Peripheral, and Systemic Immunity Following Murine Broad-Spectrum Antibiotic Treatment [2017].
- Amelioration of intestinal and systemic sequelae of murine Campylobacter jejuni infection by probiotic VSL#3 treatment [2017].
- Possible determinants of VSL#3 probiotic failure in preventing gastrointestinal adverse events associated with dacomitinib in patients with advanced non-small-cell lung cancer enrolled in ARCHER-1042 trial [2016].
- Unexpected improvement in core autism spectrum disorder symptoms after long-term treatment with probiotics [2016]. – single patient
- Probiotic mix VSL#3 is effective adjunctive therapy for mild to moderately active ulcerative colitis: a meta-analysis[2014]. By itself, not significant effect.
- Oral Probiotic VSL#3 Prevents Autoimmune Diabetes by Modulating Microbiota and Promoting Indoleamine 2,3-Dioxygenase-Enriched Tolerogenic Intestinal Environment[2016]. From which I found the chart below. By itself, only a minor effect — but when combined with RA is retinoic acid, a major shift
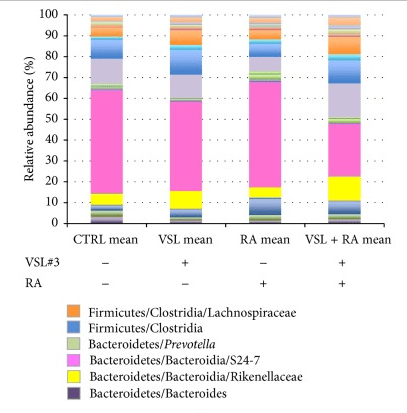
Relevant Studies
Research Double Speak: “Improvement” – may mean that there is only a 2% improvement, shown by statistical analysis which is often indicated by the use of the word “significantly“.
- Probiotics for Irritable Bowel Syndrome: Clinical Data in Children. ” concluded that Lactobacillus GG, Lactobacillus reuteri DSM 17938 and VSL#3 significantly increased treatment success. We recently showed that, in children with IBS, a mixture of Bifidobacterium infantis M-63®, breve M-16V® and longum BB536® is safe and is associated with better AP control and improved quality of life when compared to placebo.” –
- ” clinical trials in children showed an improvement in abdominal pain for Lactobacillus GG, Lactobacillus reuteri DSM 17938, and the probiotic mixture VSL#3. The patients most benefiting from probiotics were those with predominant diarrhea or with a post-infectious IBS.” [2014]
- “Before therapy, intestinal microbiota of IBS subjects differed significantly from that of healthy controls, with less diversity and evenness than controls (n = 9; P < 0.05), increased abundance of Bacteroidetes (P = 0.014) and Synegitestes (P = 0.017), and reduced abundance of Actinobacteria (P = 0.004). The classes Flavobacteria (P = 0.028) and Epsilonproteobacteria (P = 0.017) were less enriched in IBS. Abundance differences were largely consistent from the phylum to genus level. Probiotic treatment in IBS patients was associated with a significant reduction of the genus Bacteroides (all taxonomy levels; P < 0.05) to levels similar to that of controls." [ [2013] The genus bacteroides improved, but not Actinobacteria, Synegistetes, or Epsilonproteobacteria. Flavobacteria was low, and article implies that it went lower.
- Gut microbiota is not modified by Randomized, Double-blind, Placebo-controlled Trial of VSL#3 in Diarrhea-predominant Irritable Bowel Syndrome [2011].
- Does VSL#3 really improve symptoms in children with IBS? [2012] – summarizes some major problems with how earlier studies were done.
- “A randomized controlled trial of a probiotic combination VSL# 3 and placebo in irritable bowel syndrome with bloating[2005]. “VSL# 3 reduces flatulence scores and retards colonic transit without altering bowel function in patients with IBS and bloating.”
No studies with SIBO, Chronic Fatigue Syndrome or Fibromyalgia.
Bottom Line
There is low value (and high costs) to taking VSL#3 for IBS/FM/CFS/SIBO. While it does reduce one of the groups of bacteria — it does not impact other significant groups. I greatly favor taking Prescript Assist or General Biotics Equilibrium as a better choice than VSL#3.
- “Conclusion. The probiotic formula[5 g of VSL#3 twice daily] when taken orally over the 12-week period did not significantly alter the microbiota measured in this population. ” [2016]
- VSL#3 Persistance
“Streptococcal population was detected after 3 days of administration and persisted for 6 days after the treatment suspension.” [2003] — No part of it was detected after a week. It’s benefit requires constant taking.
The use of retinoic acid with probiotics is an interesting aspect.
- “Epithelial cells have also been shown to metabolize vitamin A into retinoic acid (RA) (2)”
On a naive level, it suggests that taking Vitamin A with probiotics may be beneficial — but this is strictly speculation.
