A few years ago American Gut and uBiome were both new kids on the block. It seems that uBiome is the dominant one at the moment. I was delighted when a reader forwarded their gut results because every lab result is interesting in what is there and what is not there. See this page on what is or is not on various ones.
Both report at the genus level.
Data Visualization Report

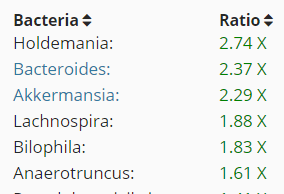
Looking at the above we clearly see the over-dominance of Bacteroidetes from the left chart and almost extermination of several others.
There are NO OTHER reports.
Patient History
- Childhood and pre-CFS days: lots of penicillin and septrin ( trimethoprim and sulfamethoxazole)
- Comment: Those antibiotics appear to be counter-indicated for CFS.
- 1979 — flu whose symptoms persisted
- Severe vertigo attacks
- Severe anxiety with agoraphobia
- Started teaching career
- Picked up infections and more antibiotics
- 2001 Tested positive for heavy metal poisoning (nickel and mercury).
- 13 amalgams replaced.
- Andy Cutler’s protocol
- 2006 Tested normal for mercury
Current state:
“I was able to do small amounts of voluntary work for a few hours each week and also walk my dog for around 25 minutes most days. However I have never been able to walk for longer than 30 minutes maximum at a time before my energy runs out and once my blood sugar drops to say 5 all energy is gone and there is nothing left in my legs. Using a oxygen concentrator for 30 minutes at a time helps me to feel better and I tend to do this 3 times daily.”
“I guess I have about 60 g carbs daily which are mainly nuts and seeds, a small amount of Sourghan crispbread, lots of vegetables including daily salad, a tiny amount of mixed organic berries from the garden just once daily, a small portion of meat or fish. I am ok with dairy but not gluten so have a small quantity of whole milk yoghurt most days together with things like flax seed, chia seeds and psyllium. Have been doing this since the Genova report in late 2015.”
I have taking various Probiotics over the years but none of made a difference to how I feel. One interesting thing is that I made my own Kefir for a long time this past year but it seemed to make my gut a lot worse which lots of rumbling and rolling and very loose bowel movements so I have stuck with the natural yoghurt which is fine. I am in the process of trying a small amount of Sauekraut each day to see if that will help me.
My main problem is the severe almost daily migraine, very little dizziness now and bp is fine whereas it used to be so low before treatment. Still energy runs out and I have to PACE very carefully. During the winter I can pick up many viruses which always start in my throat. Echinacea Augustraflora does help this if I drop it frequently down my throat btw.”
Earlier Analysis
Genova Diagnostics 2008
- High pH: 8.1
- High Acetate
- Lactobacillus: – “in lower than optimal levels”
- Eschericha coli 4+ (Mucoid E.Coli)
- Bifidobacterium – “in lower than optimal levels”
Genova Diagnostics 2015
- Low Diversity (remember this varies according to test sensitivity)
- High Verrucomicroba Phylum
- High Fusobacteria Phylum
- Low Proteobacteria Phylum
Commensal Bacteria
Bacteria Genus of interest
- Bacteroides (genus)
- Peptococcaceae (family)
- Clostridium (genus)
- Part of
- Lachnospira (genus)
- Ochrobactrum (genus)
- Rubellimicrobium (genus)
- Rhodospirillum (genus)
- Citrobacter (genus)
- Odoribacter spp
- Pseudoflavonifractor –
NUTRIENTS/ SUBSTRATES
INHIBITED BY
ENHANCED BY
INHIBITS
Bottom Line
I would not recommend AmericanGut because the amount of information available to the patient is very little compared to uBiome results (a test that cost less than $100 and does not need a prescription or MD involvement). uBiome has occasionally offered them for free.
Microbiome
Most of the sugar substitutes encourages growth of the above bacteria – bad (Aspartame, Saccharin, Stevia) where as high sugar diet or Sucralose (Splenda) reduces the growth. Sugar substitutes are conceptually nice — but they have major risk for maintaining a bad microbiome.
Citrobacter is still high — there are two paths: Pomegranate ellagitannins or the antibiotics cited above (I would start with minocycline first if you go the antibiotic route — one of the tetracycline family).
There are no apparent clustering of inhibited by or enhanced by, so just try working off the lists.
Regular Breakfast Suggestion: Barley porridge and some walnuts (without Aspartame, Saccharin, Stevia). For a month avoid flax seed, chia seeds and psyllium as an experiment — I was unable to find reliable information on what types of resistant starch these could be.
Occasion Supper: Navy beans with a high fat content meat.
Patient History
It was interesting to read that home-made Kefir made her worst — this is likely because it contains lactic acid producing bacteria (which is why I advocate avoiding most Lactobacillus bacteria — see this post “D-lactic Acidosis -Sauerkraut is not good for you if you have CFS!“). A list of strains in Kefir is here. In general, avoid most yogurts and kefirs — use Activia (bifidus regularis) if you wish to continue having yogurt (See Confusion At The Yogurt Aisle? Time for Probiotics 101).
She also wrote: “I changed my diet to lower carb and higher protein and fats because I had such swings of blood sugar in 2001. This helped and because of the steroid I have to be very careful with the carbs or my blood sugar will stay a bit too high unless I am active which of course I cannot do all the time. “ which are inhibitors of the overgrowth bacteria cited above. ” I feel better on a lower carb diet because otherwise I get extremely high blood sugar readings and feel generally horrible, sluggish, headachy, muzzy and falling asleep.”
It is also interesting that we have a lot of the bacteria associated with sugars and there are challenges maintaining sugar levels.
Probiotics: The patient did not specify what she has tried. I suspect they are the typical health food stores ones high in lactobacillus species (which can actually make you worst). I would suggest trying at least one from each of the following two groups:
- Soil Based Organisms
- E-Coli Probiotics (Note there are good E.Coli and bad E.Coli — the items below are known to displace bad E.Coli)
Subject for future post MSG:
“One thing comes to mind is if I ever I eat MSG by mistake in a restaurant it hits my brain almost immediately like a gun going off in my head. I will pour with sweat, be dizzy and then get a 2 day migraine. I have often wondered if I produce too much glutamate and some of the meds I have had for migraine prevention do work on the conversion of glutamate to GABA and have been slightly effective until the side effects kick in and I cannot tolerate them.”
As always — this is education information and not intended to treat. Always consult with a knowledgeable medical professional.