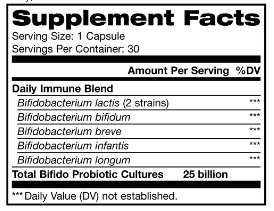
LOW Akkermansia is associated with a variety of conditions according to the Smart Gut test, including Crohn’s Disease and Obesity.
A reader asked explicitly how to increase akkermansia bacteria in the body, is there a probiotic available? Low levels of akkermansia is associated with obesity.
- Melatonin: “… melatonin supplementation reversed 14 operational taxonomic units OTUs [of 69]…in particular through its ability to decrease the Firmicutes-to-Bacteroidetes ratio and increase the abundance of mucin-degrading bacteria Akkermansia, which is associated with healthy mucosa.” [2017]
- Capsaicin (CAP) – found in cayenne peppers! “reduces body weight…showed a higher abundance of Akkermansia muciniphila, a mucin-degrading bacterium with beneficial effects on host metabolism.” [2017]
- Lingonberries [IKEA stocks often] “The relative abundance of Akkermansia and Faecalibacterium, genera associated with healthy gut mucosa and anti-inflammation, was found to increase in response to lingonberry intake.” [2016]
- “Increased gut microbiota diversity and abundance of Faecalibacterium prausnitzii and Akkermansia after fasting: a pilot study.“Akkermanisa and Bifidobacteria increased in abundance due to intervention. The inflammation-associated gut microbes Enterobacteria and Lactobacilli increased during the first week and then declined by the end of the intervention.” [Human study — full text]
- Table Grapes: Table grape consumption reduces adiposity and markers of hepatic lipogenesis and alters gut microbiota in butter fat-fed mice [2016]. ” tended to increase the abundance of the beneficial bacterium Akkermansia muciniphila compared to controls”
-
“First day: breakfast: Pernegg muesli (prunes, dates, raisins, flaxseed, water); lunch: potatoes and vegetables; dinner: vegetable soup.
Second day: breakfast: herbal tea, Glauber’s salt, lunch: fresh squeezed fruit and vegetable juice, dinner: fasting soup.
All other fasting days: breakfast: herbal tea, lunch: fresh squeezed fruit and vegetable juice, dinner: fasting soup.”- The modulatory effect of infusions of green tea, oolong tea, and black tea on gut microbiota in high-fat-induced obese mice[2016]. “Tea consumption has been identified to have an anti-obesity effect…it was revealed that tea infusion consumption substantially increased diversity and altered the structure of gut microbiota.”
- ” the fibre-rich macrobiotic Ma-Pi 2 diet… resulting in an increase of the ecosystem diversity and supporting the recovery of a balanced community of health-promoting SCFA producers, such as Faecalibacterium, Roseburia, Lachnospira, Bacteroides and Akkermansia.”[2016] [British Medical Journal description of this diet is here: bmjdrc-2014-000079supp]
- A probiotic for use with lab animals is cited [2017] [2016]
- Akkermansia muciniphila: a novel functional microbe with probiotic properties[2016]. “Moreover, products containing A. muciniphila are not on the market and are thus controlled by the Novel Foods Regulation, which requires extensive safety assessment.”
- “We observed a low abundance of the mucin-degrading bacterium Akkermansia muciniphila in the mice that were fed Enterococcus faecium NCIMB 10415 for 8 weeks.” [2012] — So Enterococcus faecium probiotics (like symbioflor-1) should not be taken concurrent with above approaches to increase Akkermansia. 😦
- [in terms of infants] ” In Finland probiotics were given to mothers (n = 79) for 2 months prior to and 2 months after delivery. In Germany probiotics were started in infants (n = 81) at weaning, at the latest at 1 month of age, and continued for 4 months …n breast-fed infants a trend toward higher counts of bifidobacteria was detected in Finland (p = 0.097) as against Germany, where a more diverse microbiota was reflected in higher Akkermansia (p = 0.003),”[2012] Again, an interaction between probiotics(bifidobacteria) and Akkermansia
- ” High Fat feeding significantly reduced (P < 0.05) 1 operational taxonomic unit (OTU) of the genus Bifidobacteria (64-fold) and 5 OTUs of the genus Akkermansia (≥16-fold).” [2016] Reduce the amount of fat in your diet!
- “pH 5.5–8.0, with optimum growth at 37 C and pH 6.5″ [2004] – thus an alkaline environment would inhibit it some what.
Bottom Line
A shift reduce fat content and increase fiber content, especially fiber from fruits which in polyphenol, appears to be an effective pattern. Table grapes and lingonberries are known to benefit. Increased tea consumption (increased polyphenols) and trying a fasting diet or Ma-Pi 2 diet are additional approaches.
I suspect that an Akkermansia probiotic could first appear in the US — given the current push for deregulation — as long as there are no claims of actual benefits from it on the label…