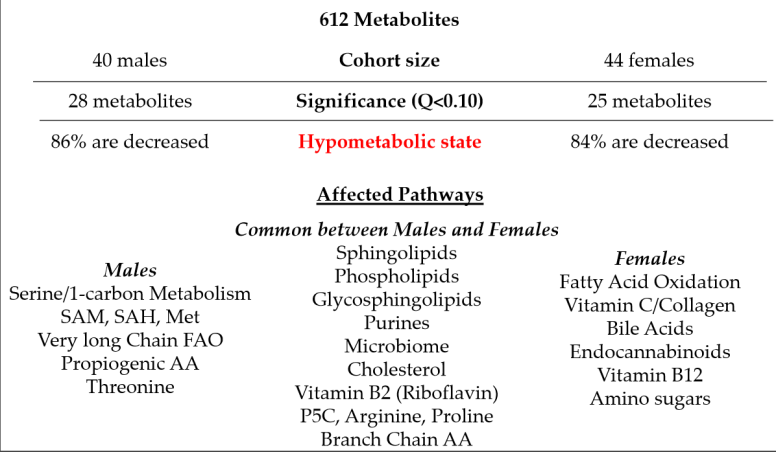
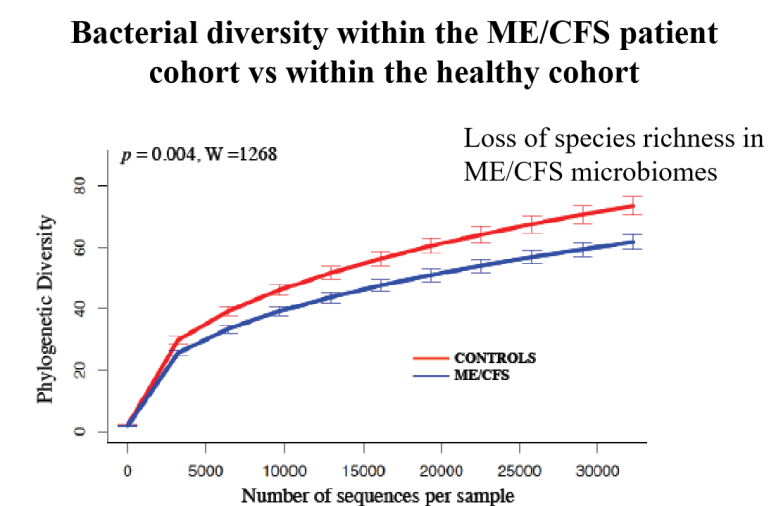
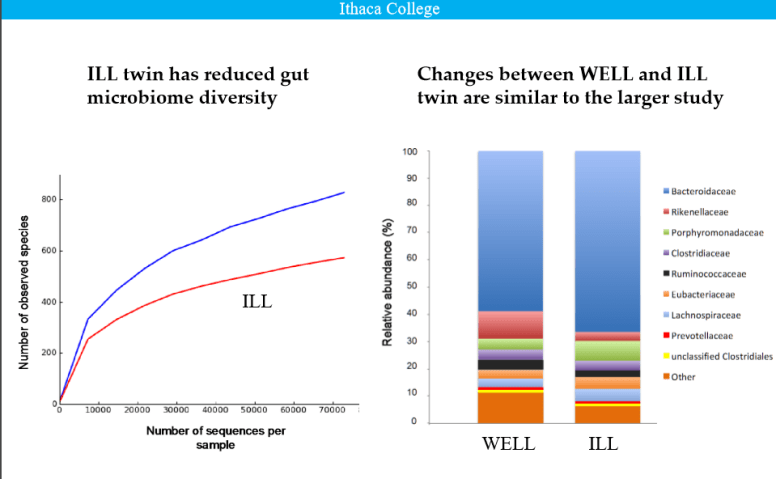
A reader email me and stated that he believe that he has an overgrowth of (bad) Enterococcus. I had done an earlier post and thought that I should dig deeper, there are some hints that enterococcus is involved with Chronic Lyme [2007]
Background
“The first description of Enterococcus spp. as agents of infection causing infective endocarditis was reported in 1899 (Maccallum and Hastings 1899); however, enterococci emerged as major multidrug-resistant opportunistic pathogens in the 1990s (Uttley, Collins, Naidoo et al., 1988; Sood, Malhotra, Das et al., 2008). As recently reviewed by Arias and Van Tyne, ‘enterococci epidemiology’ has evolved with antibiotic use and evolution of medical practices (Arias and Murray 2012; Van Tyne and Gilmore 2014). Over the past 30 years, enterococci have become a leading cause of healthcare-associated infections (HCAIs) worldwide (Arias and Murray 2012). Enterococcus faecalis was the first species found to be responsible for infections, but clinical E. faecium strains have been increasingly reported since 2000. A correlation was established between the use of antibiotics in animal feed and human medicine and the emergence of resistant enterococci, in particular of vancomycin-resistant enterococci (VRE) and ampicillin-resistant enterococci (ARE) in fragilized populations (Agudelo Higuita and Huycke 2014).” [2015]
Option #1 Displace the bad Enterococcus
My initial take would be to displace them with good Enterococcus from probiotics:
- * Symbioflor-1 Enterococcus faecalis (Germany)
- * Bioflorin – Enterococcus faecium SF 68 (Germany)
- * BENOIT Enterococcus AF2 (ITALY)
Option #2 Probiotics that reduce enterococcs
- Mutaflor (E.Coli Nissle 1917) [2011]
- Potentially Symbioflor-2 may also be effective.
- “Lactobacillus fermentum VET 9A, L. rhamnosus VET 16A, and L. plantarum VET 14A … the concentrations of Clostridium perfringens and Enterococcus faecium, which typically increase during diarrhea episodes in dogs, were decreased in probiotic group feces” [2016]
- “six lactobacillus strains (L. gasseri, L. rhamnosus, L. acidophilus, L. plantarum, L. paracasei, L. acidophilus)… had similar moderate antimicrobial activities against…Enterococcus fecalis. [2016]
- “ingestion of the Butyricicoccus pullicaecorum strain 25-3T strain significantly lowered the abundance of Campylobacter spp. in the caecum and Enterococcus and Escherichia/Shigella spp. in the ileum at day 40.” [2016]
- Lactobacillus rhamnosus GG Outcompetes Enterococcus faecium via Mucus-Binding Pili: Evidence for a Novel and Heterospecific Probiotic Mechanism [2016].
- Effect of Lactobacillus rhamnosus GG Administration on Vancomycin-Resistant Enterococcus Colonization in Adults with Comorbidities.[2015]
- Potential use of probiotic and commensal bacteria as non-antibiotic strategies against vancomycin-resistant enterococci. [2015]
- Lactobacillus rhamnosus GG but “In contrast, L. rhamnosus Lcr35, related to the strain GG, did not show a significant decrease in VRE” – the right strain is needed!
- “a probiotic mix of 10 strains of Bifidobacterium bifidum, Bifidobacterium lactis, E. faecium, Lactobacillus acidophilus, Lactobacillus rhamnosus, Lactobacillus paracasei, Lactobacillus plantarum and Lactobacillus salivarius …At the end of the 4.5 month trial, …showing no preventive effect”
- In lab animals: Bacillus coagulans, Pediococcus acidilactis MM33, Lactococcus lactis MM19, Bacteroides thetaiotaomicron
Option #3 Herbs and Spices
- “Brillantaisia lamium… Enterococcus faecalis… were the most sensitive to all the tested compounds.” [2011]
- “the annual herb Acanthospermum hispidum DC. (Asteraceae) …a selective antibacterial activity was observed against pathogenic strains of Staphylococcus aureus and Enterococcus faecalis ” [2012]
- “Rubus parvifolius L. (Rp) is a medicinal herb that possesses antibacterial activity…inhibited the growth of a wide range of Gram positive and negative bacteria, including … Enterococcus faecalis,[2012]
- “Conyza sumatrensis (Retz.) E.WALKER (Asteraceae) is a spontaneous annual herb.. the leaf oil exhibited significant in vitro antibacterial activity against Enterococcus faecalis” [2013]
- “among the most active EOs against MDR E. faecalis strains, O. glandulosum, T. capitata, L. multifida, and A. verticillata EOs are constituted principally by terpenoid phenols,…a good synergetic effect between compounds of Eucalyptus globulus EO against multidrug-resistant bacteria, Staphylococcus aureus and Enterococcus faecalis. [2014]
- From my earlier post on Enterococcus overgrowth,