This is my periodic review of news on probiotics (not always CFS specific)
- “Proteins secreted by a strain of E. coli suppress bad gut bacteria – posted in Immunology Products: There are both good and bad bacteria in our bodies. The balance of the intestinal bacteria group is essential for health. Now, a new research from University of California Irvine has identified that the beneficial bacterium Escherichia coli Nissle 1917 (EcN) secretes small proteins called microcins that limit the growth of harmful gut bacteria during intestinal inflammation.” [2016]
- “The researchers compared the gut microbiota of healthy Chinese centenarians, and nonagenarians (90-99 years old) (n = 67), with younger individuals (including 54 elderly and 47 young adults) and with the results from the previous study of gut microbiota in Italian centenarians (n = 15) and semi-supercentenarians (n = 24) by Biagi et al.Datasets from the Chinese and Italian studies were combined and re-analyzed. Significant differences in overall community membership and structures between the Italian and Chinese long-lived groups were observed. Despite these differences, common features that discriminated long-lived from younger individuals were identified in both groups.
A total of 50 features (including bacterial operational taxonomic units –OTUs– and alpha-diversity measures) from the combined Chinese and Italian dataset differentiated long-lived individuals from others. Specifically, 11 features were shared by the older individuals in the Chinese and Italian studies, including community richness, members of Blautia, Clostridium XIVa, Faecalibacterium, Escherichia_Shigella, and unclassified Lachnospiraceae, Ruminococcaceae, and Erysipelotrichaceae. Alpha diversity – an estimator of within-community diversity – was among the top features that distinguished long-lived people from younger ones. Besides this, both community richness and community diversity were greater in the long-lived group than in the younger group.”[2016]
- ” In a new study, scientists developed a new tool to examine genetic differences within bacterial species and uncover novel transmission patterns in mother-infant microbiomes” [source]
- “Gnotobiotic mouse model is generally used to evaluate the efficacy of gut microbiota. Sex differences of gut microbiota are acknowledged, yet the effect of recipient’s gender on the bacterial colonization remains unclear.” [source]
- ” bacteria also live in a woman’s breast tissue-and the mix of those microbes may have an equally important effect on health, according to a new study in Applied and Environmental Microbiology.” [source]
- “Bacteria from celiac patients influence gluten’s digestion and its ability to provoke an immune response” [source]
- “A specific strain of Lactobacillus acidophilus may relieve symptoms of lactose intolerance” [source]
- “Dietary fibre/short-chain fatty acids and vitamin A may protect mice against peanut allergy via gut microbiota” [source]
- “Mucosal Inflammation, and the Environment in Post-Infectious Chronic Gut Syndromes”[source]
- “It is known that infection may trigger post-infectious chronic gut syndromes for example, post-infectious irritable bowel syndrome and post-infectious functional dyspepsia. This sequence of events is likely dependent upon a myriad of other host and environmental factors and an inherent inflammatory response of the gut mucosa to pathogens, which may be regulated by the genetic background. This review topic aims to unravel genetic influences on host response, which lead to differing clinical outcomes in enteric infection preceding chronic gut syndromes.”
- “Chronic sleep fragmentation (SF) commonly occurs in human populations, and although it does not involve circadian shifts or sleep deprivation, it markedly alters feeding behaviors ultimately promoting obesity and insulin resistance. These symptoms are known to be related to the host gut microbiota.” [source]
- “The results of our study demonstrated that 17.7% chicken protein diet promoted the beneficial genus Lactobacillus in young rats, but the opposite effect were found in the middle-aged group [decreased Lactobacillus]. To evaluate the linkage between diet and host health, age effect should be considered in the future studies.” [2016]
- “Dietary modification has long been used empirically to modify symptoms in inflammatory bowel disease, irritable bowel syndrome, and a diverse group of diseases with gastrointestinal symptoms. There is both anecdotal and scientific evidence to suggest that individuals respond quite differently to similar dietary changes, and the highly individualized nature of the gut microbiota makes it a prime candidate for these differences.” [source]
- “Princeton researchers have for the first time revealed the mechanics of how bacteria build up slimy masses, called biofilms, cell by cell. When encased in biofilms in the human body, bacteria are a thousand times less susceptible to antibiotics, making certain infections, such as pneumonia, difficult to treat and potentially lethal.” [source]
- “Researchers … found an association between migraines and microbes that reduce nitrates….suggests that migraine suffers avoid eating nitrate-filled foods if they suspect it is causing them migraines.” [source]
- “certain proteins produced by gut bacteria may be linked to neurodegeneration in rats.”[source]
- “the FDA announced<https://www.federalregister.gov/articles/2016/03/01/2016-04372/enforcement-policy-regarding-investigational-new-drug-requirements-for-use-of-fecal-microbiota-for> that it intended to tighten its rules on the procedure, known as fecal microbiota transplantation (FMT), making it harder for doctors to buy stool from banks,”
- “the immune system programmes itself on the spectrum of strains that are presented to it in the first months of life and thereafter rejects anything that is not exactly the same strain as an early resident.”
- ” Several studies have also found an association between the receipt of antibiotics and an increased incidence of psychiatric disorders, perhaps due to alterations in the microbiome. Studies to characterize the intestinal microbiome of individuals with these disorders are in progress.” [2016]
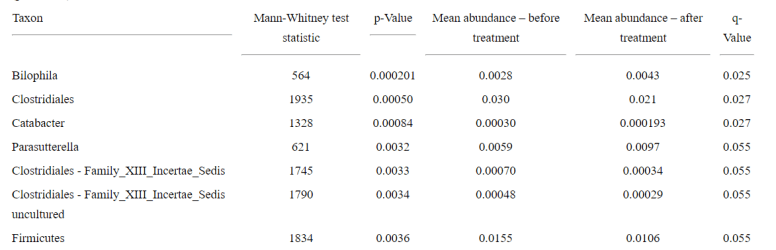
- “Identification of an Intestinal Microbiota Signature Associated With Severity of Irritable Bowel Syndrome[2016]” – ” In our study, the LASSO procedure identified 90 bacterial OTUs that could be used as a composite gut microbial signature for IBS severity.“
- ” find that mice carrying a mutant version of the Foxp3 gene show changes in their gut microbiome at around the same time that they develop autoimmune symptoms. In particular, the mice have lower levels of bacteria from the genus Lactobacillus. The researchers discovered that by feeding the mice with Lactobacillus reuteri, they could “reset” the gut bacterial community and reduce the levels of inflammation, significantly extending the animals’ survival.” [2016]
- “reports that short-chain fatty acids produced by a mouse’s gut microbiome can affect the epigenetics[how DNA is activated] in the animal’s cells: The compounds change the activity of enzymes that help add acetyl and methyl groups to histone proteins, thereby altering the availability of nearby DNA for transcription” [2016]
- “”We conclude that Faecal Microbiota Transplant can transfer not only microbiota but also the donors’ intestinal innate immune status and improved intestinal integrity”.” [2016]
- “Previously, we demonstrated that Lactobacillus salivarius was more abundant in patients with rheumatoid arthritis (RA), an inflammatory autoimmune disease wherein the gut microbiota is altered, than in healthy individuals.” [2016]
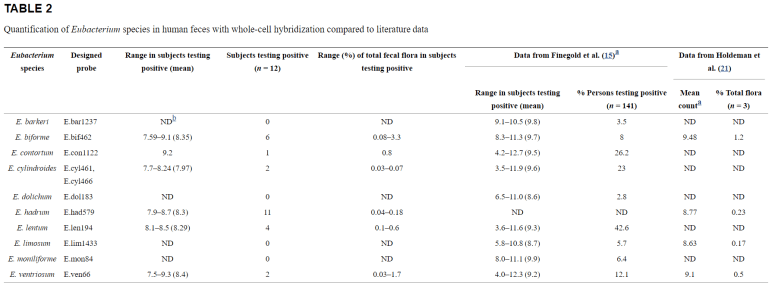
- “Optimization of culturing techniques has allowed the identification of 1,057 prokaryotic species within the human gut microbiome repertoire, doubling the previous number of isolated species from the human gut.” [2016]
-

New members of the human gut