A reader asked about this – is it helpful? is it worth the cost? Being a former general science teacher, there is really nothing to it. I taught it in my high school science classes. In fact, an ancestor was a favorite lens grinder for the early dutch microscope inventors. See wikipedia or Rice University page (where I borrowed the microscope image below from).
The main thing is that most MDs have stopped using microscopes and using one for dark-field is a bit of an alternative-fad.
- “ME Medical Advisor Dr Andy Wright takes a look at new technology enabling ‘live’ blood analysis and asks ‘Could this help ME patients?” [Prohealth 2000] like 200 years new!
- Below is a darkfield micrograph taken in 1910 [source]
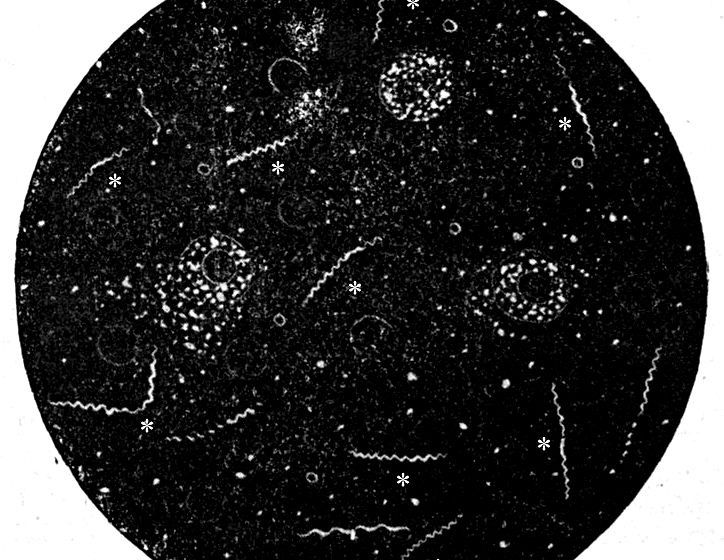
There are two ways that a specimen can be viewed in a normal microscope:
- Light passes thru the specimen
- Light is shone on the sample — often from the side.
Video of what it takes to make an ordinary microscope into a dark field microscope
Dark Field and CFS
On the web you will find links to articles about using dark field with CFS. So exactly what did they find?
- “this is certainly not a diagnostic tool for any one condition.’” [Prohealth 2000]
- “Using Dark field microscopy you see the red blood cells of these people clumping together. This reduces the oxygen that they can supply to the tissues of the body.” [site] – Low oxygen is a known for CFS patients (hyper-coagulation)
- “Bradford also claimed that the microscope was especially useful in detecting the spirochete that causes Lyme disease. Bradford promoted these methods through several publications as well as through symposia for medical doctors. Neither the device nor the three products had FDA approval, so they were not legal to market in interstate commerce..and admitted they were part of a conspiracy to commit mail fraud and to introduce misbranded drugs into interstate commerce. .” [devicewatch]
Bottom Line
Dark field microscopy is still used by medicine for certain conditions. It has been around for hundred of years (literally). Dark field video can produce an impressive presentation for a CFS patient when presented by a health professional well , “confirming a physical cause”. IMHO — it has no direct or indirect impact on remission. For the microbiome, dark field is not done — there are just two many species (over 2000 usually), many of which will die quickly when expose to oxygen. You cannot tell a bad strain from a good strain visually (or even identify the strain!)
If you look at the video below, which describes a healthy system and then imagine a dialog describing everything as evidence of infection and bacteria – you would be impressed and be a believer!
Does it have any apparent benefit to a CFS patient? None that I can identify- except reducing their savings.
Does it help with treatment?
A test helps with treatment only if it swings the decision to do a certain treatment from the normal default treatment. I can find no evidence that this alters (or authorizes) treatment. A Lyme tests known to produce false positives (because of reactivated EBV) does authorize/justify the use of antibiotics in CFS patients. This is now the system works.
Does it help with insurance and other claims?
If it is not accepted by traditional medical science, then it will be very unlikely to be significant for an insurance or benefit claim. If anything, it may cause the claim to be more critically (negatively) reviewed.
