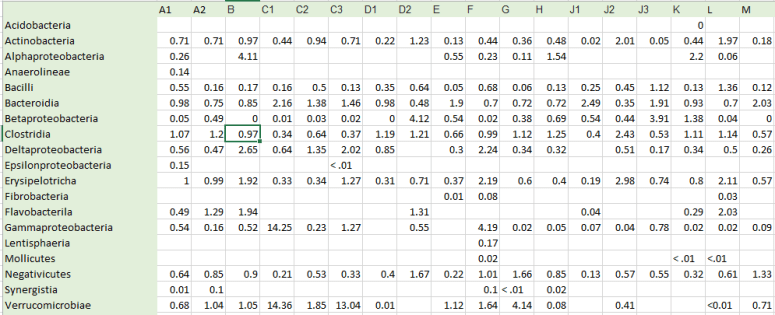
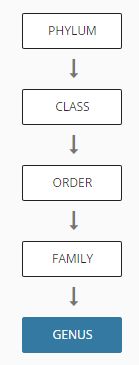
The Phylum levels had 12 items reported. The Class level had 19 items. The next level down, the Order level has 24 items. Some of the Class will be divided into several parts. For other, we have just one part of the class reported.
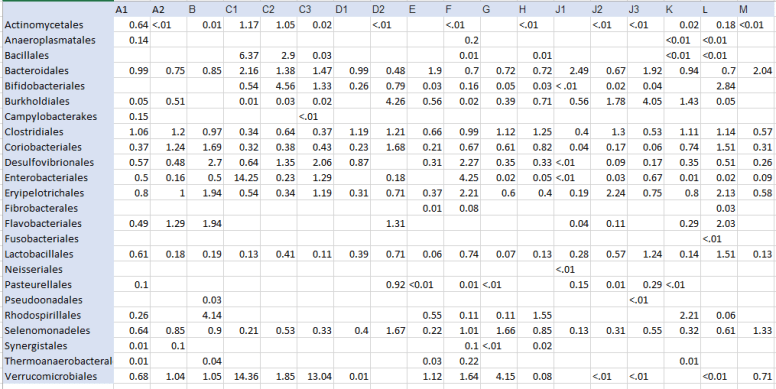
Common Items
I will not go thru every item, just the high points. For many of the items we have very limited knowledge on what they do. For “normal”, we would expect both an average and middle value between 90% (.9) and 110% (1.1). Using a wider range of 70% (.7) and 140% (1.4) could be describe as “slightly off”. If the numbers are further off, then something is happening.
- Bifidobacteriales [Actinobacteridae / Actinobacteria]Average 63%, Middle value 4% (some may have taken bifidobacteria probiotics prior to the tests)
- Clostridiales [Clostridia / Firmicutes]- normal
- Coriobacteriales [Actinobacteria /Actinobacteria]Average 64%, Middle value 40%
- Desulfovibrionales [ Deltaproteobacteria / Proteobacteria ] Average 74%, Middle value 41% – appears to be a go high or go low (almost no one near normal) “The majority are sulfate-reducing” increasing foods containing sulphur would be appropriate (i.e. dark green vegetables)
- Enterobacteriales [ Gammaproteobacteria / Proteobacteria ] Average 124%, Middle value 13%. – 75% are very low
- Lactobacillales[Bacilli/Firmicutes] Average 42%, Middle value 22%
- Selenomonadeles Average: 70%, Middle value 58%
- Verrucomicrobiales: About 50% are very low.
The 1998 report on the microbiome shift seen with CFS appears to be confirmed. Low Bifidobacteriales, Lactobacillales, Enterobacteriales (which includes Escherichia, i.e. E.Coli). All of the patients have at least 2 of the three being very low.
Some details
Result C
Result C illustrates that the microbiome can be changed. I suspect that prior to the second test, C2, there was significant intake of Bifidobacteria Probiotics, increasing lactobacillus and reducing verrucimicrobiales and what appears to a pathogenic enterobacteriales overgrowth.
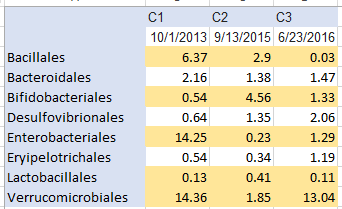
A high level of verrucimicrobiales is reported after antibiotics:
- “Dramatic colonisation of the human gut microbiota by the Verrucomicrobia phylum following a broad-spectrum antibiotic regimen occurred without significant gastrointestinal manifestations, suggesting that influenced by external factors such as antibiotics, the gut repertoire remains partially unknown.” [2012]
- ” Proteobacteria (including Escherichia coli), and Verrucomicrobia (including Akkermansia mucinophila) are typically present in smaller numbers in the healthy gut microbiota, but these organisms have considerable potential to influence health outcomes.” [2015]
Result L:
“at the time I took the test I had not taken any probiotics as pills for over a year, but was eating lacto fermented vegetables, yoghurts cultured from whatever was in the commercial greek and natural yoghurts that I had purchased as starter cultures and pseudonatto. I guess the yoghurts could have contained bifidobacteria but I had intentionally bought the old fashioned brands that do not boast any particular probiotic species. The ubiome test did pick up 87 l. delbruekii and 14 s. thermophilus so I guess I have some idea of what was in the yoghurt.”
- This is the highest level of Lactobacillales and second highest Bifidobacteriales seen in all of the tests. Unfortunately Enterobacteriales was still very low.
- One model is that d-lactic acidosis is involved (heavily produced by Lactobacillales) and only a little by Enterobacteriales is the cause of ongoing symptoms. The Enterobacteriales are needed to get the amount lowered.
- High levels of Erysipelotrichaceae
- “The importance of Erysipelotrichaceae in inflammation-related disorders of the gastrointestinal tract is highlighted by the fact that they have been found to be enriched in colorectal cancer.” [2015]
- Decrease (Toxoplasma gondii or Giardia muris infections) or increases (TNF Driven Crohn’s Disease) – see link for more details
- Impacts obesity
- “The importance of Erysipelotrichaceae in inflammation-related disorders of the gastrointestinal tract is highlighted by the fact that they have been found to be enriched in colorectal cancer.” [2015]
Downloads
PDF: order
Excel: order