- L-glutamine impacts gut bacteria http://www.nutritionjrnl.com/article/S0899-9007(15)00035-0/abstract
- The Firmicutes/Bacteroidetes ratio decreased after glutamine supplementation.
- Firmicutes and Actinobacteria reduced significantly after glutamine supplementation.
- Dead Probiotics have some benefits
- [Article] heat killed Lactobacillus gasseri TMC0356 (TMC0356) can modify the immune response in the elderly
- non-viable Lactobacillus rhamnosus CRL1505 http://www.sciencedirect.com/science/article/pii/S1567576915000521
- Can pass traits to children http://www.biosciencetechnology.com/news/2015/02/mothers-can-pass-traits-offspring-through-bacterias-dna?et_cid=4420409&et_rid=688877945&type=cta
- “The study is the first to show that bacterial DNA can pass from parent to offspring in a manner that affects specific traits such as immunity and inflammation.”
- “When the scientists housed mice with low levels of the antibody with mice that had high levels of the antibody, all of the mice ended up with low antibody levels in a few weeks. … low antibody levels is [associated with] a bacterium called Sutterella”
- Shift seen with onset of type 1 diabetes http://www.nutraingredients.com/Research/Microbiome-changes-linked-to-onset-of-type-1-diabetes
- Impact of diet: http://www.microbecolhealthdis.net/index.php/mehd/article/view/26164
- Vegetarian Diet: increased proportions of Bacteroides/Prevotella group, Bacteroides thetaiotaomicron, Clostridium clostridioforme, and Faecalibacterium prausnitzii
- Western Diet:
- The least microbial diversity in this study was observed for adult Americans
- the genus Prevotella was underrepresented
- WHOLE GRAIN PRODUCTS
- proportion of Lactobacillus/Enterococcus group was increased
- barley flakes, brown rice flakes, or a mixture of both increased microbial diversity, as well as a rise in the proportion of Firmicutes and a reduction of the Bacteroidetes phylum
- barley:a higher abundance of Blautia and Roseburia and a lower abundance of Bacteroides.
- white bread vs rye bread: numbers of Bacteroidetes decreased, whereas levels of Clostridium cluster IV, Collinsella, and Atopobium spp. increased.
- FRUITS AND NUTS
-
- an increased amount of Bifidobacterium spp. in the feces of volunteers after blueberry drink consumption.
- increase of the Bifidobacterium genus after consumption of red berries
- consumption of red wine and de-alcoholized red wine the abundance of Bifidobacterium,Enterococcus, Eggerthella lenta, and the phylum Fusobacteria were increased compared to baseline values (most effects were more pronounced after red wine consumption)
- pistachios had a stronger impact on microbiota composition than the consumption of almonds.
Author Archives: lassesen
Latest News on Probiotics
My irregular review on recent probiotics news:
- Reduces Anxiety
- http://newsroom.ucla.edu/releases/changing-gut-bacteria-through-245617: Danone Yogurt (sponsored study)
- http://www.nature.com/news/2011/110830/full/news.2011.510.html : Lactobacillus rhamnosus
- http://www.sciencedirect.com/science/article/pii/S0889159115000884#b0100:Bifidobacterium infantis 35624
- http://www.alphagalileo.org/ViewItem.aspx?ItemId=151650&CultureCode=en : Mixture
- http://www.sciencedirect.com/science/article/pii/S0889159115000884
- Bifidobacterium bifidum W23, Bifidobacterium lactis W52, Lactobacillus acidophilus W37, Lactobacillus brevis W63, L. casei W56, Lactobacillus salivarius W24, and Lactococcus lactis (W19 and W58).
- http://www.sciencedirect.com/science/article/pii/S0889159115000896 Antibiotics increases
- http://www.ncbi.nlm.nih.gov/pubmed/24888394 The order Bacteroidales showed an overrepresentation (p = 0.05), while the family Lachnospiraceae showed an underrepresentation (p = 0.02) of OTU’s associated with depression.
- Obesity
- http://www.the-scientist.com//?articles.view/articleNo/42392/title/Sewage-Bacteria-Linked-to-Obesity/ Bacteroidaceae were found in greater abundance in the locales with the relatively high obesity rates
- Improves Serotonin leves
- http://www.cell.com/cell/abstract/S0092-8674(15)00248-2: Indigenous spore-forming bacteria
- Impacts Body Odors
- Pears Appear to “balance Microbiota”
- http://www.sciencedirect.com/science/article/pii/S0963996914007844 H. pylori inhibition
- Agave better than maltodextrin [Study]
- Gut bacteria shared by family groups of Baboons. http://dx.doi.org/10.7554/eLife.05224#sthash.3coIKCFq.dpuf
- Can predict food allergies http://www.ncbi.nlm.nih.gov/pubmed/25599982
- Diabetes: May both detect risk, and treat http://www.ncbi.nlm.nih.gov/pubmed/25818484
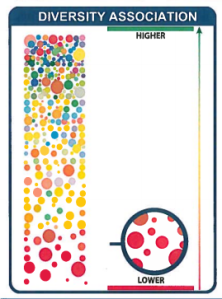
Increasing Biodiversity of the Microbiome/Gut Bacteria
A reader forwarded his Genova Stool results and I want to focus on one aspect of it that is shown below. Low biodiversity of gut bacteria, as show below.
A flippant answer would be “Stop washing you fruit,vegetables, hands and have a tablespoon of good organic living soil every day!” In other words, extreme Hygiene Hypothesis! Instead, I will do a conservative, pubmed based analysis.You may also wish to read this post by Dr. Lipman
Probiotics
The obvious first choice is Prescript-Assist with some thirty species, followed by Floracol probiotics which is similar, but in theory should have different strains. As well as Microflora Restore and any other soil based probiotics that you can fine, In some cases, you may have to search overseas to find such offerings.
Foods
The first food that comes to mind is what I use to encourage biodiversity, 100% rye bread [2012]. Rye was the stable of most North European diet until only a few hundred years ago. Our gut bacteria far better evolved to live off rye instead of wheat. There are usually two choices – both imported from Europe (US Rye bread is usually made with a little rye and a lot of wheat!). Loafs form Germany and Poland (for example Mestemacher Whole Rye Bread) and Sweden/Norway Crisp breads).
Exercise also improves diversity[2014] and as a corollary, less obese people have better diversity[2013]. Fasting also increases diversity [2015]
Going over to AmericanGut.Org, they reported in 2014
- How much of the microbial diversity participants shared with other participants depended greatly on how recently they had taken antibiotics. Those participants who had taken antibiotics within the last year tended to have less shared diversity with other participants.
- Alcohol imbibers tended to have greater microbial diversity than those that don’t drink alcohol at all.
- Spikes in microbiome populations seem to occur around holidays: in July, and in November through January.
- There is no single organism that is found in every person, but some are more common across the population than others.
- People who sleep more and who exercise outdoors have more diverse microbiomes.
- The microbiomes of the elderly resemble those of infants in certain respects, as seen in other studies
Most of the other articles dealt with increasing the amount (that is already there) and not diversity.
Speculation: Eating a wide variety of ethically different (and not “americanized”) foods would also increase diversity.
And the last way, horrible horrible way, long deep french kisses with healthy young things! [80 million living units per kiss! – [2014] … new pick up line, “Kiss me — I don’t want your body, just the bacteria in your body!!”
“
Anti-TNF Supplements – Part 2
I am continuing the review of items listed at “HOW TO INCREASE PERFORMANCE AND IMPROVE HEALTH BY INHIBITING TNF-ALPHA“ to identify items with good and bad impacts on microbiome. While taking TNF-alpha reducers is a good intent to reduce inflammation, some have adverse effects, similar to what I found is anticoagulant supplements.
He has a long list so I will not be doing deep searches and excluding items with no information. I have NOT verified if his assertions are backed by PubMed articles.
- Bile (R)
- Bacillus cereus increases [2015]
- Regulation is key. Increases Fusobacteria [2014]
- Glycine (R)
- Chromium (R)
- Increases Actinobacteria and Acidobacteria [2012]
- Sialic Acid (R, R2)
- Arginine (R),
- shift in the Firmicutes-to-Bacteroidetes ratio to favor Bacteroidetes [2014]
- Bromelain (R),
- Inhibits enterotoxigenic Escherichia coli[1996]
- Berberine (R, R2), — NOT recommended for CFS
- Decrease Clostridium difficile [2015]
- Increased the generation of bile acids [2015]
- lower counts of Escherichia coli but greater Lactobacillus[2013]
- Blautia and Allobaculum, were selectively enriched, [2012]
- berberine has demonstrated highly significant activity againstStaphylococcus, Streptococcus, Salmonella, Klebsiella, Clostridium, Pseudomonas, Proteus, Shigella,Vibrio, and Cryptococcus species [2011]
- Apple polyphenols (R)
- Silymarin (R), – Nothing
- Honokiol (R), – Nothing
- Chinese Skullcap (R)/Baicalin (R), – Nothing
- Ginkgo (R), – Nothing
- Hespderidin (R), (in Citric) see apple literature above [2015]
- Carnosine (R), – Nothing clear
- Phytosterols (R),
- Reduces lactobacilli [1999]
- Tart Cherry (R) high in sorbitol, not recommended for some conditions.
- Astaxanthin (R), – nothing
- Astragalus (R), -Not recommended for CFS
- Cat’s claw (R), – Nothing
- Artemisinin (R)
- Reduces Aggregatibacter actinomycetemcomitans, Fusobacterium nucleatum subsp. animalis, Fusobacterium nucleatum subsp. polymorphum, and Prevotella intermedia.[2015]
- Carnitine (R) – Nothing clear
- Genistein (R) – Nothing clear
- Amla/Gooseberry (R)
- Increases lactobacilli and bifidobacteria, decreases Clostridium spp. and Bacteroides spp were decreased [2014]
- CoQ10 (R), – Nothing significant
- Magnolol (R) – Nothing
- Echinacea (R) – Nothing
- Chaga/Betulin (R) – Nothing
- Bitter melon (R) – Nothing
- Mastic gum (R),
- Oxymatrine (R) – Nothing clear
- Red clover (R) – Nothing clear
- NAG,
- Quercetin (R)
- Reduces Firmicutes/Bacteroidetes ratio, reduces Erysipelotrichaceae, Bacillus, Eubacterium cylindroides [2015]
- Feeds Escherichia coli, Stretococcus lutetiensis, Lactobacillus acidophilus, Weissella confusa, Enterococcus gilvus, Clostridium perfringens and Bacteroides fragilis [2014]
- Inhibits R. gauvreauii, B. galacturonicus and Lactobacillus sp [2012]
- Rutin (R) – no impact [2008]
- Myricetin (R)
- Increases B. adolescentis [2013]
- Ashwagandha,
CFS 201 Treatment and Treatment Model
Following up on my earlier post, CFS 101, I want to first describe the model that I have concluded is the best model using classic scientific criteria (simplest that is consistent with all known data) and then look at the two dimensions of treatment:
- Symptom Mitigation
- Remission
Symptom mitigation is relief of symptoms but the conditions continues. For example, taking immune-system suppressants may reduce many symptoms and may create the illusion of remission — but CFS continues. Stopping the symptom mitigation results in the symptoms returning. Think of taking antihistamine for hay-fever, they do not cure it, just take away the symptoms.
Model
CFS (and in general all post-infection malaise conditions which could include post-vaccination as well as environment exposure to mold, organic phosphates etc) results in a stable dysfunction of gut bacteria. There was a recent microbiome study where they took gut bacteria from a half dozen diseases, ran the microbiome through big data algorithms, and developed a forecasting model. This model was 90% accurate when applied to new patients coming in before a formal diagnosis. At present diagnosing by gut bacteria is unlikely to be a clinical tool for several reasons:
- It takes weeks to do the analysis
- Only a few conditions has been studied — and they were done largely as academic proof of concept
- This is new science and thus takes time to be accepted by a conservative professional like MDs
Premise #1: Infections and environments can alter gut bacteria.
” On the basis of only 15 biomarkers, a highly accurate patient discrimination index is created and validated on an independent cohort. Thus microbiota-targeted biomarkers may be a powerful tool for diagnosis of different diseases.”[2014]
Corollary #1.A: The gut bacteria shift produces many of the symptoms of the disease.
- Different bacteria causes different symptoms in CFS. Gut bacteria is inherited and equivalent to a finger print. When it gets altered, it is uniquely altered resulting in unique symptoms.
For several post-infection malaise, there have been studies on how long it has lasted since technical remission. The short version is something like 60% are back to normal within 4 weeks (leaving 40% tired), over the next 4 weeks, half of those recover (leaving 20% tired after two months), Around 6 months, the recovery rate drops to just 30% of those still exhausted, and by 2 years, the rate is down to just 10% every year. This agrees with a mathematical modelling study that found that a stable altered microbiome can fail to recover to normal after N months — a new stable microbiome (producing a different set of chemicals being sent into the body).
Premise #2: Recovering to a healthy microbiome without intervention occurs with declining probability over time
Treatment for Remission
There is a nice full text Pub Med article that is a good starting point: Manipulating the gut microbiota to maintain health and treat disease. [2015] which covers the entire scope of options.
” Even when causality between changes in the Firmicutes/Bacteroidetesratio and lupus progression requires further validation, these results will generate new hypotheses to test dietary strategies to correct dysbiosis in this pathology, suggesting a new therapeutic approach to treat autoimmunity diseases.”[2015]
Antibiotics – Prescription
This has been part of my treatment in all three cases of CFS that I have had. How does this work? Simple — it disrupts the gut bacteria! Exactly the reason many people do not want to take antibiotics. IMHO the best protocols are those of Cecile Jadin — long term rotation of different types of antibiotics. They need to be long term to de-stablize the dysfunctional stable microbiome. The antibiotics in her protocols appears to impact the typical species associated with CFS well. Note: we are using the antibiotics not to fight an infection but to destablize the gut bacteria.
Antibiotics – Herbal
The same logic applies to herbs and spices with antibiotic characteristics. As with antibiotics, the species impacted by each is very important — which typically means slugging through PubMed articles. The ones that seem to be effective are (in order of preference) are:
- Tulsi
- Neem
- Olive Leaf Extract
- Wormwood
- Haritaki
The typical dosage that I have worked up to have been 6 capsules per day (in the case of home-made capsules — “00” capsules). We do not know which are friendly to which probiotics, so if you have limited budget — do not take them at the same time as probiotics (if you have deep pockets, give it a try).
As with antibiotics, you should be rotating them regularly because the name of the game is disruption!!
Probiotics
Initially I was opposed to any Lactobacillus because of a lack of positive information for many species and negative for others. Today, I am in favor of including the following strains and species:
- Culturelle – Lactobacillus rhamnosus GG (ATCC 53103) – well documented on Wikipedia.
- L. Reuteri — as many different strains as you can obtain (I currently use 3 different strains)
- This species produces B12, which CFS are usually low in
The following are documented to be effective for IBS — which tends to ~ 80% co-morbid with CFS
- Align – Bifidobacterium longum subsp. infantis 35624
- Prescript Assist
Lastly, because E.Coli is typically very low or non-existent with CFS,
- Mutaflor – E.Coli Nissle 1917.
On my secondary list are any Bifidobacterium-ONLY probiotics. I still avoid taking any lactobacillus acidophilus, while it has some health benefits for healthy individuals, it inhibits E.Coli (which are at unhealthy low levels with CFS) [2015]
Since our intent is to disrupt and replace with good ones, and the recommended dosage is for maintenance of a healthy individual, I have typically (after consulting with my health professional) gone up to 3x the recommended dosage.
Fecal Transplants
This has resulted in short term remission (i.e. 6-9 months, from correspondence) to permanent. There are challenges in getting it done (although there is medical literature going back almost 2000 years), for example:
“In the USA, their Food and Drug Administration has classified fecal microbiota as a drug, and by this classification physicians have to submit a time-consuming application,” [2015]
Attack the Reserves
Good oral health is essential — and I think a little clarification is needed. Toothpaste and mouthwash impact cavities but not oral bacteria (or impacts in the wrong way!). The use of a water pic followed by rotating different oral probiotics (usually dissolved in the mouth) should be part of daily hygiene. Rinsing with EDTA or NAC dissolved in warm water (to break down biofilms) should also be considered.
“around 50% were suggestive of oral isolate, raising the possibility of oral commensals invading the gut.” [2014]
The use of biofilm busters to expose the gut bacteria to the above agents may also be needed. There are a number of biofilm busters such as EDTA and NAC. Several herbs and other supplements are also biofilm busters.
Treatment For Symptom Relief
The following is reported in the literature as reducing CFS and/or FM and/or IBS Symptoms:
- Vitamin D3 — high normal values have less symptoms, 20,000 IU/day is what I typically take.
- Magnesium
- B12
- CoQ10 300 mg/day – Studies in this post.
- Licorice
- D-Ribose
- Piracetam and other Racetams
On top of these are anti-inflamatories, like TNF-Alpha reductors.
Coagulation Relief
Dave Berg, Hemex Labs, found that hyper-coagulation is often involved (85%). Coagulation can act the same as biofilms, allowing reserves to be kept alive and thus keep pumping their chemicals into your system. The gotcha is that this is generally associated with an inherited coagulation defect and there are many! Each have different characteristics. Piracetam (cited above) and Turmeric(with 1% black pepper) have very similar impacts on some form of coagulation plus the added advantages for Turmeric of being a antibacterial, antiviral, and antifungal [2014].