https://www.amazon.com/dp/B07GBFJLXM/
See https://cfsremission.wordpress.com/2018/08/02/an-awesome-clinical-trial-for-ibs-folks/
This is a review of recent studies recorded on PubMed. The focus is on new information – so studies reporting prior information will rarely be mentioned.
We continue to lack any significant studies on microbiome shifts for FM. A microbiome dysbiosis model fits well — including the increased risk of progression into dementia (which have greater dysbiosis). L. Casei and Vitamin D are both known modifiers of the microbiome.
This is another one of a series of posts dealing with various conditions that appear to be microbiome related. My first posts dealt with Alzheimer’s Disease, ALS and Parkinson’s Disease. Additional posts are listed here. My personal suspicion is that a significant catalyst (if not actual cause) is the lost of microbiome as we age. For all of these conditions, it appears microbiome correction moderates the condition.
Almost a decade ago, I had a relapse of a condition that I had before and was sent for a SPECT scan. The radiologist suggested that it may be early onset Alzheimer’s. I was having problems with memory then, especially retaining recent memories. In 2017, for the same condition, a patient died and when their brain was examined, this study found
“Among the most remarkable pathological features of the case are focal areas of white matter loss, neurite beading, and neuritic pathology of axons in the white matter with axonal spheroids. Atypical neurons displaying aberrant sprouting processes in response to injury are observed throughout cortical gray and white matter. Abundant amyloid deposits identical to Alzheimer’s disease plaques with accompanying intracellular granular structures are observed as well. Neurofibrillary tangles are also present in the white matter of the frontal cortex, thalamus and basal ganglia. “
For myself, I went into remission. Memory and other issues faded — I am not 100% as strong in some cognitive aspects that I was prior, but to most people they cannot detect the remaining issues.
The condition that I had was successfully treated using a protocol that altered the microbiome. What if this was true for other similar conditions — especially the untreatable ones? Recent literature appears to support this (this is only a fraction of 2017 and 2018 studies)
A 2011 Study found that Cerebrospinal Fluid Proteomes were different for my condition, a normal population and PTSD. These CFP’s are also heavily studied with MS “Statistical analysis evidenced different levels on 23 proteins: 8 proteins showed lower levels in multiple sclerosis patients with respect to controls”[2018].
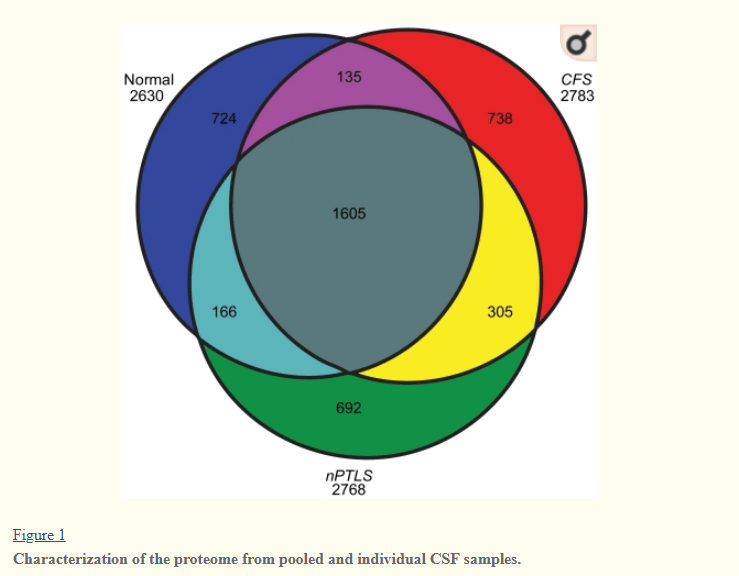
My working hypothesis is that these CSF proteins are due to microbiome disruption. This disruption may not be a magic bacteria that causes it, but due to undersupply or oversupply of metabolites causing epigenetic changes in the bacteria resulting in these new proteins. With MS there are a large number reported (see image below)
The hypothesis implies that there would distinctive shifts in bacteria seen with MS. What does the literature say? I actually listed many studies a year ago in this post, Multiple Sclerosis and microbiome. Remember a change of diet means a change of the microbiome.
I have added a few more recent studies below.
If you are a carer for someone with MS, you may wish to get a 16S analysis done ( for example uBiome.com – < $100) and upload the results to http://microbiomeprescription.com/. The suggestions there are based on hundreds of studies of what shifts different members of the microbiome. It’s a free site and the information is not available easily any wherelse.
An example of getting suggestions is shown in this post.
I have updated the MS Microbiome template on that site, and added it as a symptom (Official Diagnosis). The number of bacteria changes reported is very large.
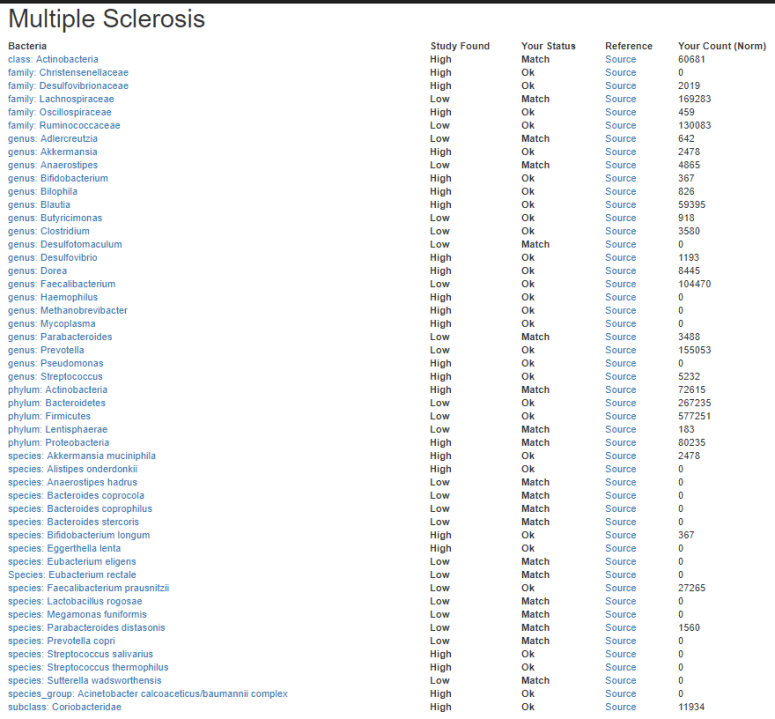
Look at the suggestions generated and discuss them with your treating physician.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.
This is the third of a series of posts dealing with various forms of cognitive impairment that are often age related. My first posts dealt with Alzheimer’s Disease and Parkinson’s Disease. My personal suspicion is that a significant catalyst (if not actual cause) is the lost of microbiome as we age.
Almost a decade ago, I had a relapse of a condition that I had before and was sent for a SPECT scan. The radiologist suggested that it may be early onset Alzheimer’s. I was having problems with memory then, especially retaining recent memories. In 2017, for the same condition, a patient died and when their brain was examined, this study found
“Among the most remarkable pathological features of the case are focal areas of white matter loss, neurite beading, and neuritic pathology of axons in the white matter with axonal spheroids. Atypical neurons displaying aberrant sprouting processes in response to injury are observed throughout cortical gray and white matter. Abundant amyloid deposits identical to Alzheimer’s disease plaques with accompanying intracellular granular structures are observed as well. Neurofibrillary tangles are also present in the white matter of the frontal cortex, thalamus and basal ganglia. “
For myself, I went into remission. Memory and other issues faded — I am not 100% as strong in some cognitive aspects that I was prior, but to most people they cannot detect the remaining issues.
The condition that I had was successfully treated using a protocol that altered the microbiome. What if this was true for other similar conditions — especially the untreatable ones? Recent literature appears to support this.
A 2011 Study found that Cerebrospinal Fluid Proteomes were different for my condition, a normal population and PTSD. These CFP’s are also heavily studied with ALS ( 2015 Study) ” Ten proteins were differently regulated in ALS CSF compared to controls in at least 2 studies. ” [2017] – both have novel proteins (i.e. proteins not seen in a healthy population). “We identified significant differences in the CSF proteomebetween living and post mortem ALS subjects, as well as living and post mortem control subjects. We also noted differences in the CSF proteome of ALS subjects that have exhibited symptoms for varying lengths of time and between ALS and Alzheimer’s Disease subjects at end-stage of disease.” [2007]

My working hypothesis is that these CSF proteins are due to microbiome disruption. This disruption may not be a magic bacteria that causes it, but due to undersupply or oversupply of metabolites causing epigenetic changes in the bacteria resulting in these new proteins. Unlike both Parkinson’s Disease and Alzheimer’s disease, I could not find any studies of ALS and Bacteroides fragilis with humans. But with ALS mice (G93A), we see that in studies.
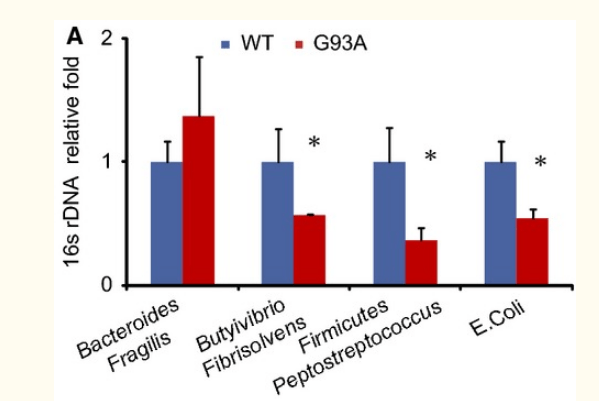
You may wish to read my Reducing bacteroides fragilis
The hypothesis implies that there would distinctive shifts in bacteria seen with AD. What does the literature say?
If you are a carer for someone with amyotrophic lateral sclerosis, you may wish to get a 16S analysis done ( for example uBiome.com – < $100) and upload the results to http://microbiomeprescription.com/. The suggestions there are based on hundreds of studies of what shifts different members of the microbiome. It’s a free site and the information is not available easily any wherelse.
An example of getting suggestions is shown in this post.
I have updated the ALS Microbiome template on that site, i.e.
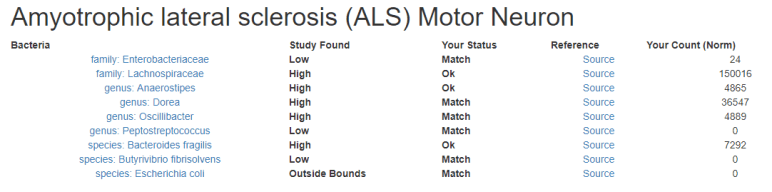
Look at the suggestions and discuss them with your treating physician.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.
A reader sent me an interesting email that interested me greatly about her daughter. Some extracts
“confined to her bed or at least her house with CFS for 5 -7 years. We’ve been following your suggestions as best we can, given my goofiness about science, and we’ve had some modest success, but in the last three weeks she began to get stirrings of energy. Her doctor…has had great success with other non-CFS patients using HCG, which here … is fashionable, along with a diet, for weight loss. … He talked her into trying HCG 3 weeks ago (without the diet- she’s on a Mediterranean diet as you recommend), first on 2 doses of .4 of 125 iu a day, which seemed to achieve nothing, then 10 about days ago, he increased it to 2 doses of 150iu a day. Within 3 days of that, she unexpectedly got out of the house at 6AM to go the airport to welcome a friend home, then stayed up all day travelling (though not driving) 130 km by car and was still awake and bubbly at 9 pm. Only a little delayed exhaustion and rattiness the next day- usually after this she’d expect to be laid out for a week or more with slurred speech etc The next two days she was on the go…. A low energy three days followed – but today as I write she’s out and about finding out what the shops look like these days! She’s begun to think about what she’d like to do in the world!”
The risk factors for continued use is high. I am pleased for this patient’s mother to see the change that occured, but there is too much risk and too little basis to even suggest it as an experiment for others. Some of the adverse effects (hypotension, hypoglycemia, constipation, fatigue) hints that it does cause alteration of the microbiome — but there are no studies on what the alterations are.
I would be inclined to discontinue use and see what the consequences are (it may have done the essential work and addition dosages may not have benefit — even for maintaining).
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.