This is the second of a series of posts dealing with various forms of cognitive impairment that are often age related. My first post dealt with Alzheimer’s Disease and later posts on ALS. My personal suspicion is that a significant catalyst (if not actual cause) is the lost of microbiome as we age.
The Light Bulb Event
Almost a decade ago, I had a relapse of a condition that I had before and was sent for a SPECT scan. The radiologist suggested that it may be early onset Alzheimer’s. I was having problems with memory then, especially retaining recent memories. In 2017, for the same condition, a patient died and when their brain was examined, this study found
“Among the most remarkable pathological features of the case are focal areas of white matter loss, neurite beading, and neuritic pathology of axons in the white matter with axonal spheroids. Atypical neurons displaying aberrant sprouting processes in response to injury are observed throughout cortical gray and white matter. Abundant amyloid deposits identical to Alzheimer’s disease plaques with accompanying intracellular granular structures are observed as well. Neurofibrillary tangles are also present in the white matter of the frontal cortex, thalamus and basal ganglia. “
For myself, I went into remission. Memory and other issues faded — I am not 100% as strong in some cognitive aspects that I was prior, but to most people they cannot detect the remaining issues.
The condition that I had was successfully treated using a protocol that altered the microbiome. What if this was true for other similar conditions — especially the untreatable ones? Recent literature appears to support this.
- “More recently, microbial dysbiosis has been associated with a number of brain pathologies, including autism spectrum disorder, Alzheimer’s disease (AD), Parkinson’s disease (PD), and amyotrophic lateral sclerosis (ALS), suggesting a direct or indirect communication between intestinal bacteria and the central nervous system (CNS). ” [2018]
- “Gut microbial dysbiosis and alteration of microbial metabolites in Parkinson’s disease (PD) have been increasingly reported… Microbiota-targeted interventions, such as antibiotics, probiotics and fecal microbiota transplantation, have been shown to favorably affect host health.” [2018]
- Progression of Parkinson’s disease is associated with gut dysbiosis: Two-year follow-up study.[2017]
- “alterations in the gut microbiota composition in humans have also been linked to a variety of neuropsychiatric conditions, including depression, autism and Parkinson’s disease.” [2017]
- “Alterations in bowel function, mainly constipation, often precede the onset of motor symptoms associated with PD“[2017]
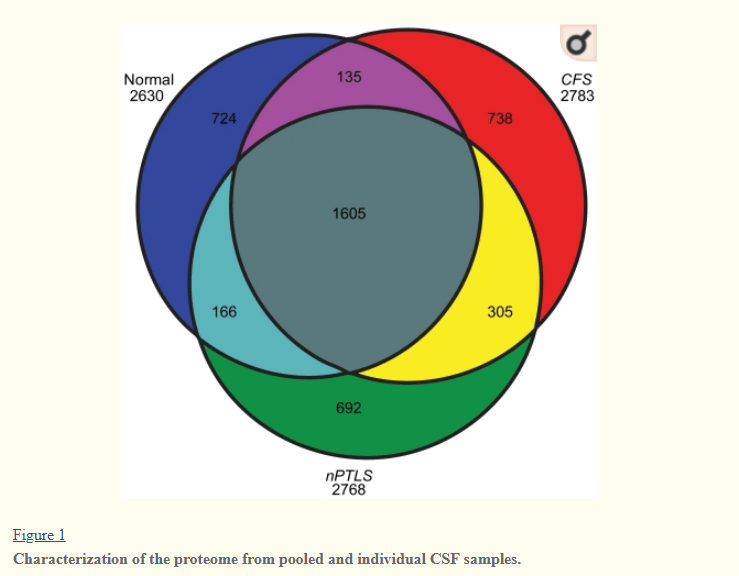
CSF Proteins Dimension
A 2011 Study found that Cerebrospinal Fluid Proteomes were different for my condition, a normal population and PTSD. These CFP’s are also heavily studied with Parkinson’s Disease ( 2009 Study) “proteins were identified that were able to differentiate atypical parkinsonian syndrome patients from healthy controls. Our study indicates that markers that may reflect neuronal function and/or plasticity, such as the amyloid precursor protein, and inflammatory markers may hold future promise as candidate biomarkers in parkinsonism.” [2017] – both have novel proteins (i.e. proteins not seen in a healthy population).
Working Hypothesis
My working hypothesis is that these CSF proteins are due to microbiome disruption. This disruption may not be a magic bacteria that causes it, but due to undersupply or oversupply of metabolites causing epigenetic changes in the bacteria resulting in these new proteins. Changes in Bacteroides fragilis is seen with both Parkinson’s Disease and Alzheimer’s disease.
- “When stressed, overpopulated or pathogenically stimulated, B. fragilis releases a remarkably complex array of endotoxins and exotoxins (such as fagilysin), lipooligosaccahrides (LOS), lipopolysaccharide (LPS), including an extremely proinflammatory B. fragilis LPS (BF-LPS), microRNA-like sncRNA, and a wide variety of bacterial-derived amyloids (9–11, 56, 57, 64–66). ” [2018]
Hypothesis Tests
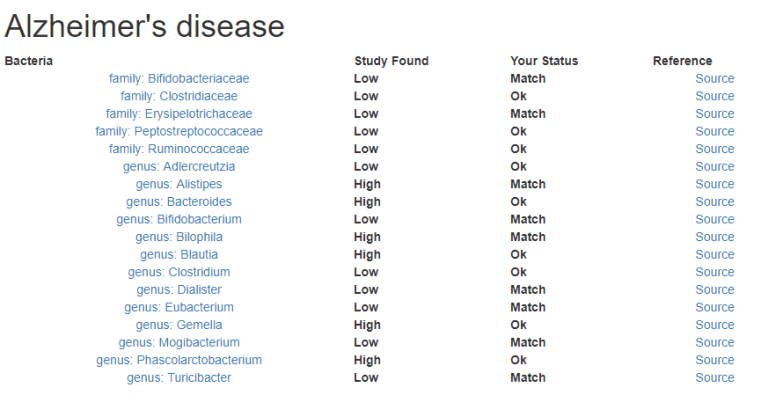
The hypothesis implies that there would distinctive shifts in bacteria seen with AD. What does the literature say?
- “In addition, low counts of Bifidobacterium at year 0 were associated with worsening of hallucinations/delusions in 2 years. Similarly, low counts of B. fragilis at year 0 were associated with worsening of motivation/initiative in 2 years. The patients were evenly divided into the deteriorated and stable groups based on the degree of worsening of total UPDRS scores. The deteriorated group had lower counts of Bifidobacterium, B. fragilis, and Clostridium leptium than the stable group at year 0 but not at year 2, suggesting that the deteriorated group may demonstrate accelerated lowering of these bacteria at year 0.” [2017]
- ” Among patients, independent signals were detected for catechol-O-methyltransferase-inhibitors (P = 4E-4), anticholinergics (P = 5E-3), and possibly carbidopa/levodopa (P = 0.05). We found significantly altered abundances of the Bifidobacteriaceae, Christensenellaceae, [Tissierellaceae], Lachnospiraceae, Lactobacillaceae, Pasteurellaceae, and Verrucomicrobiaceae families. Functional predictions revealed changes in numerous pathways, including the metabolism of plant-derived compounds and xenobiotics degradation… 13 operational taxonomic units (OTUs) had significantly altered abundances in PD vs. control samples, both using ANCOM (FDR<0.05) and Kruskal-Wallis tests (FDR<0.05).” [2017]
- Prevotella was very high — Seven times that of controls.
- “At the taxonomic level of genus, putative, “anti-inflammatory” butyrate-producing bacteria from the genera Blautia, Coprococcus, and Roseburia were significantly more abundant in feces of controls than PD patients. Bacteria from the genus Faecalibacterium were significantly more abundant in the mucosa of controls than PD. Putative, “proinflammatory” Proteobacteria of the genus Ralstonia were significantly more abundant in mucosa of PD than controls. “[2015]
- “In particular, the abundance of Lachnospiraceae was reduced by 42.9% in patients with PD, whereas Bifidobacteriaceae was enriched in patients with PD. ” [2018]
Bottom Line
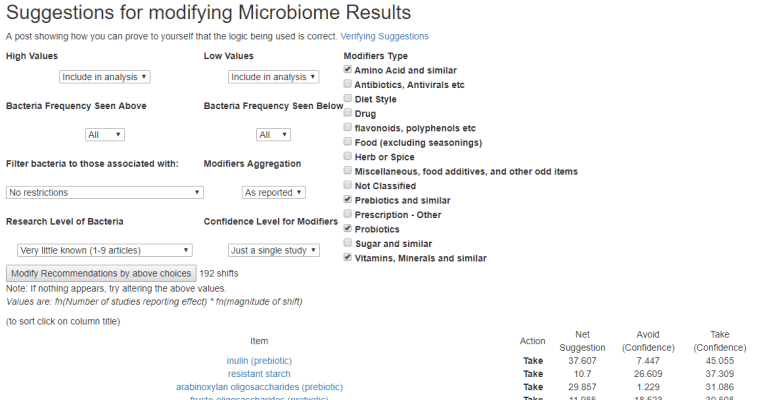
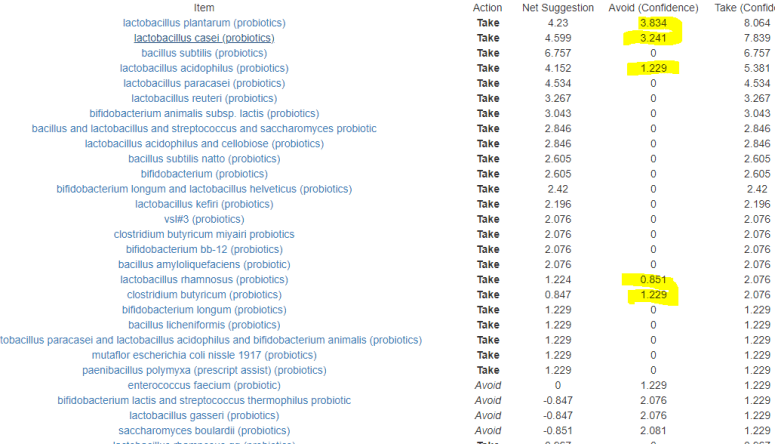
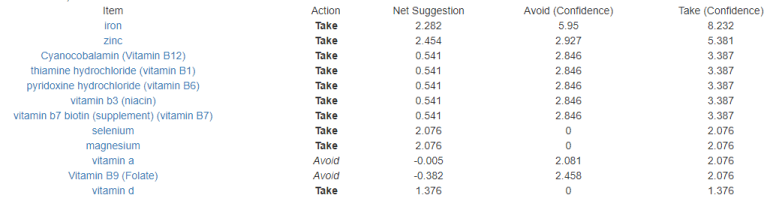
If you are a carer for someone with Parkinson’s Disease, you may wish to get a 16S analysis done ( for example uBiome.com – < $100) and upload the results to http://microbiomeprescription.com/. The suggestions there are based on hundreds of studies of what shifts different members of the microbiome. It’s a free site and the information is not available easily any wherelse.
- “By applying metagenomic sequencing procedures, it is even possible to distinguish PD cases from healthy individuals at a very early disease stage by means of individually modified microbiota. ” [2018]
An example of getting suggestions is shown in this post.
I have updated the Parkinson’s Microbiome template on the site, i.e.

Look at the suggestions and discuss them with your treating physician.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.