This is the first of a series of posts dealing with various forms of cognitive impairment that are often age related. The next posts deal with Parkinson’s and ALS. My personal suspicion is that a significant catalyst (if not actual cause) is the lost of microbiome as we age.
The Light Bulb Event
Almost a decade ago, I had a relapse of a condition that I had before and was sent for a SPECT scan. The radiologist suggested that it may be early onset Alzheimer’s. I was having problems with memory then, especially retaining recent memories. In 2017, for the same condition, a patient died and when their brain was examined, this study found
“Among the most remarkable pathological features of the case are focal areas of white matter loss, neurite beading, and neuritic pathology of axons in the white matter with axonal spheroids. Atypical neurons displaying aberrant sprouting processes in response to injury are observed throughout cortical gray and white matter. Abundant amyloid deposits identical to Alzheimer’s disease plaques with accompanying intracellular granular structures are observed as well. Neurofibrillary tangles are also present in the white matter of the frontal cortex, thalamus and basal ganglia. “
For myself, I went into remission. Memory and other issues faded — I am not 100% as strong in some cognitive aspects that I was prior, but to most people they cannot detect the remaining issues.
The condition that I had was successfully treated using a protocol that altered the microbiome. What if this was true for other similar conditions — especially the untreatable ones? Recent literature appears to support this.
- “More recently, microbial dysbiosis has been associated with a number of brain pathologies, including autism spectrum disorder, Alzheimer’s disease (AD), Parkinson’s disease (PD), and amyotrophic lateral sclerosis (ALS), suggesting a direct or indirect communication between intestinal bacteria and the central nervous system (CNS). ” [2018]
- “It seems that, inflammatory-infectious hypothesis of AD, with the great role of the gut microbiome, starts to gently push into the shadow the amyloid cascade hypothesis that has dominated for decades.” [2018]
- “The first indication of a potential mechanistic link between the pathobiology of the human gastrointestinal (GI)-tract microbiome and its contribution to the pathogenetic mechanisms of sporadic Alzheimer’s disease (AD) came a scant 4 years ago (1).”[2018] — I suspected this much earlier 😉
CSF Proteins Dimension
A 2011 Study found that Cerebrospinal Fluid Proteomes were different for my condition, a normal population and PTSD. These CFP’s are also heavily studied with Alzheimer’s Disease (2016 study), “We report strong evidence of previously reported CSF proteins and several novel CSF proteins specifically associated with amyloid pathology or neuronal injury and tau hyperphosphorylation.” [2018] – both have novel proteins (i.e. proteins not seen in a healthy population).
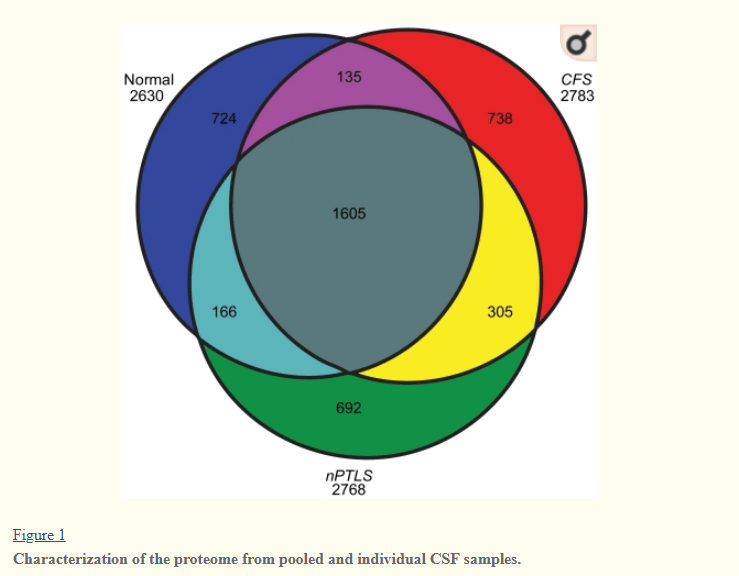
Working Hypothesis
My working hypothesis is that these CSF proteins are due to microbiome disruption. This disruption may not be a magic bacteria that causes it, but due to undersupply or oversupply of metabolites causing epigenetic changes in the bacteria resulting in these new proteins.
- “When stressed, overpopulated or pathogenically stimulated, B. fragilis releases a remarkably complex array of endotoxins and exotoxins (such as fagilysin), lipooligosaccahrides (LOS), lipopolysaccharide (LPS), including an extremely proinflammatory B. fragilis LPS (BF-LPS), microRNA-like sncRNA, and a wide variety of bacterial-derived amyloids (9–11, 56, 57, 64–66). ” [2018]
Hypothesis Tests
The hypothesis implies that there would distinctive shifts in bacteria seen with AD. What does the literature say?
- “the most enriched bacteria at genus level, the proportions of Acetobacter and Lactobacillus decreased dramatically. Acetate was the most abundant SCFA derived from the dysregulated microbiota and markedly downregulated in AD Drosophila.” [2018]
- “We identified phylum- through genus-wide differences in bacterial abundance including decreased Firmicutes, increased Bacteroidetes, and decreased Bifidobacterium in the microbiome of AD participants. Furthermore, we observed correlations between levels of differentially abundant genera and cerebrospinal fluid (CSF) biomarkers of AD. ” [2017]
- “Also, a very intriguing discovery in AD is that the Mediterranean diet (MeDi), containing an unusually large quantity of Lactobacilli, is very effective in preventing AD… it is our opinion that the reduction of blood ammonia levels by Lactobacilli in MeDi is the therapeutic agent of MeDi for AD. ” [2018]
- Lactobacilli and bifidobacteria ameliorate memory and learning deficits and oxidative stress in β-amyloid (1-42) injected rats.[2018]
- Therapeutic potential of Bifidobacterium breve strain A1 for preventing cognitive impairment in Alzheimer’s disease.[2017]
- “These findings indicate that AD pathology might not only affect brain function directly, but also exacerbate cognitive deficits through reducing the level of SCFAs via alterations of gut microbiota induced by intestinal amyloid deposition. Our data may support a role of gut microbiota, and suggest a novel route for therapeutic intervention in AD.”
- “Clinical studies have shown that, in cognitively impaired elderly patients with brain amyloidosis, there is lower abundance in the gut of E. rectale and B. fragilis, two bacterial species which have an anti-inflammatory activity, versus a greater amount of pro-inflammatory genera such as Escherichia/Shigella. ” [2018]
- “Our findings suggest an increase in bacterial populations in Alzheimer brain tissue compared with normal.” [2017]
- “We concluded that the cognitive and biochemical indications in the patients with severe AD are insensitive to the probiotic supplementation.” [2018]
Bottom Line
If you are a carer for someone with Alzheimer’s Disease, you may wish to get a 16S analysis done ( for example uBiome.com – < $100) and upload the results to http://microbiomeprescription.com/. The suggestions there are based on hundreds of studies of what shifts different members of the microbiome. It’s a free site and the information is not available easily any wherelse.
An example of getting suggestions is shown in this post.
I have updated the Alzheimer’s Microbiome template, i.e.
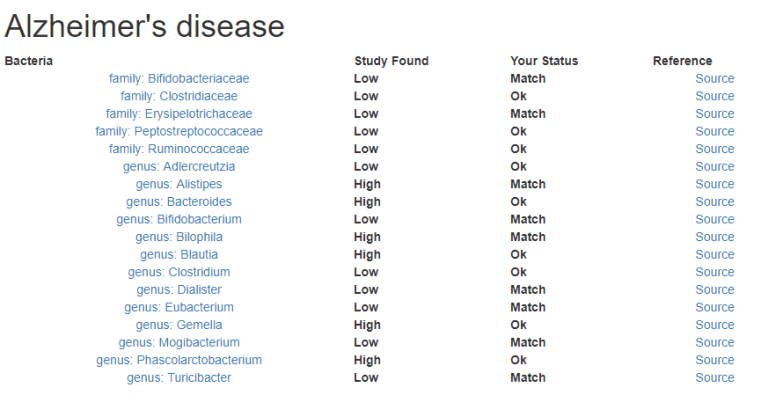
Look at the suggestions and discuss them with your treating physician.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.
