Your patient may have referred you to this blog. This physician directed page may assist you to get up to speed on evaluating the risks, benefits and logic of a model that I am proposing. I am not advocating a specific generic treatment, but a way of approaching treatment for individual CFS patients.
Original Study from 1998
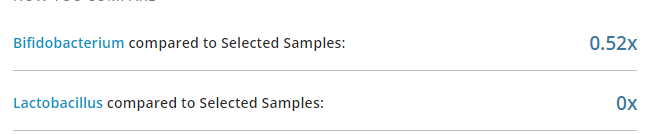
This was presented in Australia in 1998, Faecal Microbial Growth Inhibition in Chronic Fatigue/Pain Patients. The key finding was no or low lactobacillus, bifidobacterium and/or E.Coli. You can test and verify that in your own patients. Many CFS patients have used uBiome.com. In dozens of results that I have reviewed this pattern has been constant.
Simple Model
CFS symptoms are caused by a severe disturbance of metabolites produced by the microbiome being altered. The microbiome has stabilized in an unhealthy state. Various definitions have been proposed with one common characteristic: You must have N out of M symptoms
- CDC (Fukuda 1994) Definition: 4 out of 8 [Src]
- Canadian Definition: have two or more neurological/cognitive manifestations (out of ~ 12 choices) and one or more symptoms from two of the categories of autonomic (10 choices), neuroendocrine (7 choices) and immune manifestations (6 choices) [Src]
A way to reconcile all of this is simple: There are overgrowth of different bacteria genus which share one thing in common: most of these inhibit one of more of Lactobacillus, Bifidobacterium or E.Coli. The specific bacteria genus overgrown impacts the symptoms by the metabolites they produce.
What are the possible overgrowth bacteria genus?
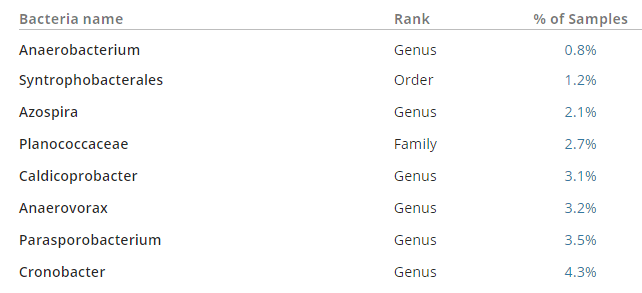
The simplest way to gain insight is to refer to the “Substrata” section of the DataPunk website, provided by Peter D’Adamo, Distinguished Professor of Health Sciences at the University of Bridgeport. It details the “bad guy” species that inhibit Bifidobacterium.
When we look up Escherichia coli, on the same site, we see which species E. Coli inhibits. Those species are listed below. When there is no E.Coli in the colon, it would allow these to overgrow. Each genus found in the above list, I have put in bold italic — and, as you can see, it’s a 100% match. When there is no E.Coli, the “bad” genuses below overgrow, bifidobacterium is eliminated, and the cascade continues.
Simple explanation: Something, like an infection, knocks down E.Coli (or similar “policing” bacteria), then many “crime families” of bacteria are free to fight it out with different combinations winning in different patients. The winners determines the symptoms because each one consumes and generate different metabolites. Got it?
Ah… just probiotics!
The unfortunate answer is likely no — the “bad guys” above will quickly dispatch the rookie cops sent in. The likely best ones are Mutaflor (E.Coli 1917) and Symbioflor-2 (a mixture of several E.Coli probiotics) — both are challenging to get outside of Germany.
A Treatment Approach to Consider
- Get a genus level comprehensive report on a patients microbiome. uBiome.com appears the easiest to get worldwide.
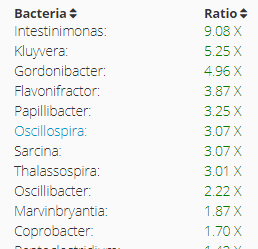
- Examine the high bacteria genus (1.5x higher than reference is my arbitrary criteria) and determine how you wish to reduce them.
- Diet changes
- Prebiotics
- Probiotics
- Antibiotics
- There is a jigsaw puzzle here because some items that reduces one overgrown genus may encourage another overgrown genus.
- What works for one patients bacteria genus overgrowth mosaic may harm a different patient (who has a different mosaic).
Bottom Line
Simple model, appearance of causality established, treatment approach based on lab results … unfortunately treatment plan is a jigsaw puzzle that is different for each patient 😦 .
Remember this is just a model.