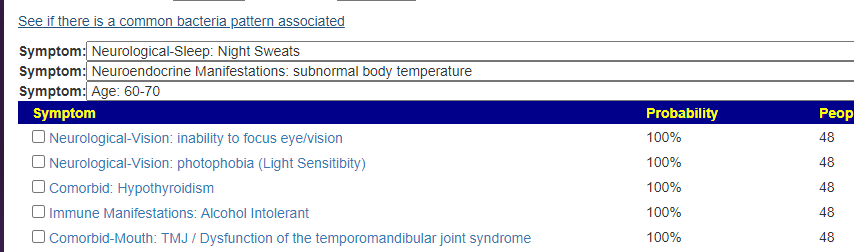
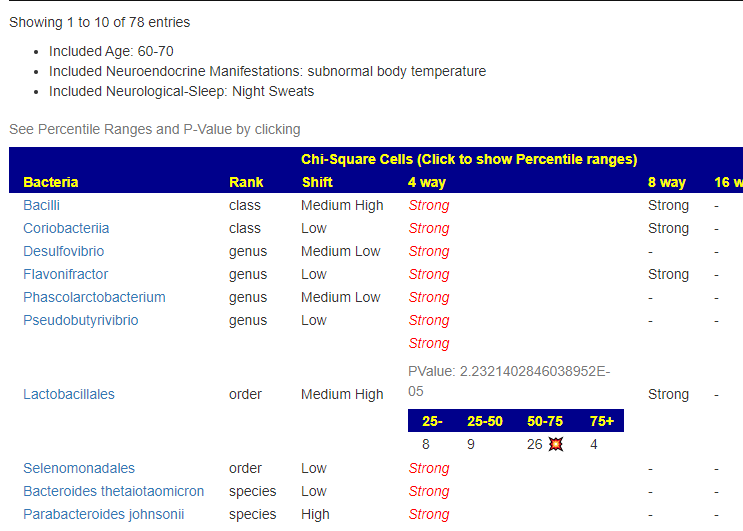
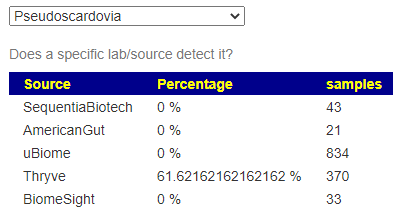
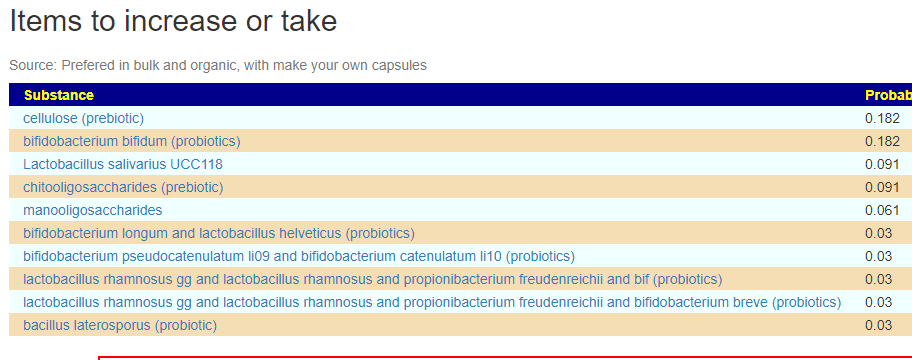
A reader asked me about this element today. I know that the abundance or absence of some minerals/elements have health impact. A simple introduction is here. A quick summary of interesting studies is shown below
- Comparative psychopharmacology of autism and psychotic-affective disorders suggests new targets for treatment [2019] ME/CFS have neurological issues often and this discusses some possible pathways.
- Lithium’s antiviral effects: a potential drug for CoViD-19 disease? [2020] ME/CFS often have virus re-activation as a contributing factor, sometimes reinforcing ME/CFS.
- The mood-stabilizing drug lithium eases repetitive behaviors seen in mice missing SHANK3, an autism gene, according to a new study. [2020]
- Emotionality is a common problem with ME/CFS. Fortunately, the people are too exhausted to become violent. But this paper raise some speculation: Is violence in part a lithium deficiency state?[2016]
- It is known to lower suicide rates [2020]
- “Trace lithium in water is negatively linked with changes in AD mortality, as well as obesity and type 2 diabetes, which are important risk factors for AD. “[2018] Translation: more lithium means less AD, obesity and diabetes.
- “Long-term increased lithium exposure in drinking water may be associated with a lower incidence of dementia” [2017]
Problems
Lithium increases hypothyroidism [2020] [2020], unfortunately hypothyroidism is common with ME/CFS [2019]. This makes it a high risk experiment if thyroid levels are low. Zinc supplements may reduce the risk [2017]
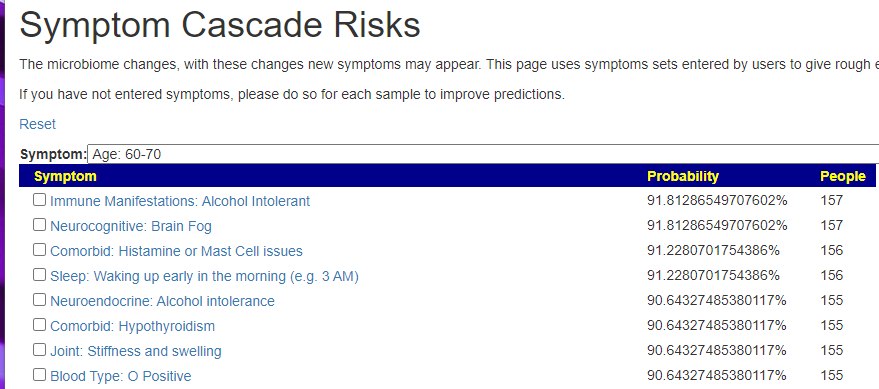
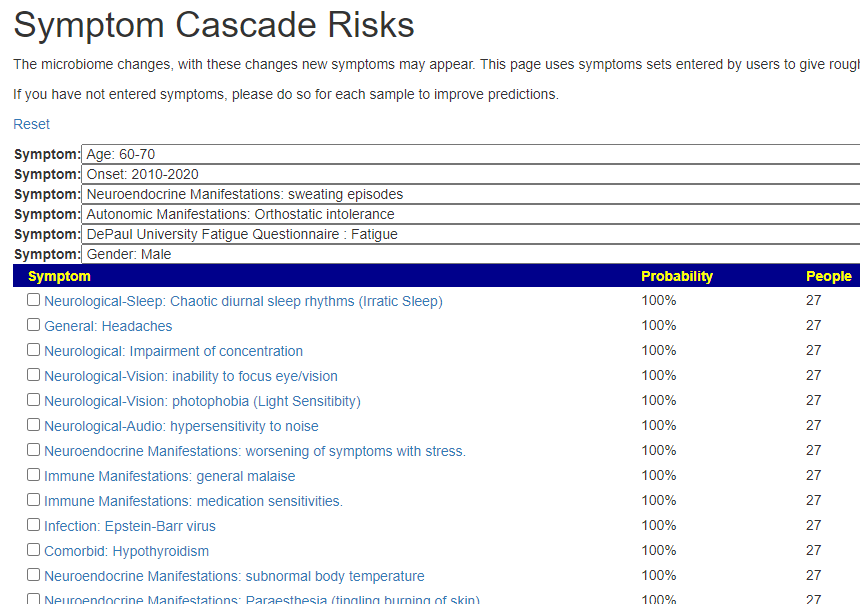
It’s known impact on the microbiome is below (and has been added to the analysis site)
” Lithium, valproate and aripiprazole administration significantly increased microbial species richness and diversity, while the other treatments were not significantly different from controls. At the genus level, several species belonging to Clostridium, Peptoclostridium, Intestinibacter and Christenellaceae were increased following treatment with lithium, valproate and aripiprazole when compared to the control group. “
Differential effects of psychotropic drugs on microbiome composition and gastrointestinal function [2018]
“Bacterial richness was increased in both treatments compared to vehicle-treated animals; moreover, at the genus level, lithium increased the relative abundance of Ruminococcaceae and decreased Bacteroides“
Psychotropics and the Microbiome: a Chamber of Secrets… [2019]
Bottom Line
It appears that Lithium was tried on ME/CFS patients a few decades ago [See the old egroup CFSFMExperimental posts on the wayback machine). We can infer that the results were not significant on the patient population as a whole. On the flip side, it does appear to have positive neurological impact for select conditions, with some risk. For Autism where it is known that the SHANK3 defect is present, we need a well constructed study to determine the benefits to risk factors.