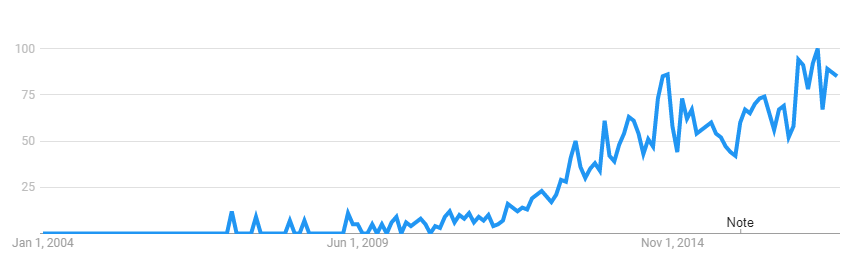
My ideas on this blog have evolved, as more and more information becomes available. This post is an attempt to bring readers up to date with my current thinking. I am striving to be transparent in my logic — showing the evidence I am working from, and my thought processes.
Notes to Treating Physicians Quick Self Start on treating CFS
Analysis of Microbiome/stool with recommendations
Site: has moved to http://microbiomeprescription.azurewebsites.net
- Ubiome Analysis Upload
- Other tests
- Enter KyberKompakt Report
- Enter Verisana Report
- Enter Bioscreen Report
- Genova Parasitology
- Gesundsheitscheck Darm Medivere
- Metagenomics Stool (De Meirleir)
- Diagnostic Solution GI-Map
- Other Tests
The data is available in an online collaborative python workbook for analysis. See this post.
Microbiome Definition of CFS/FM/IBS
A coarse condition that results from:
- Low or no Lactobacillus, AND/OR
- Low or no Bifidobacteria , AND/OR
- Low or no E.Coli , AND/OR
- A marked increase in number of bacteria genus (as measured by uBiome) to the top range
- Most of these genus are hostile to/suppress Lactobacillus, Bifidobacteria, E.Coli
- Several are two or more times higher than normally seen
- The number of bacteria genus goes very high (using uBiome results), but most of them are low amounts.
(“Death by a thousand microbiome cuts” and not “Death by a single bacteria blow”)
- The appearance of rarely seen bacteria genus in uBiome Samples.
A finer definition would be a condition with a significant number of abnormalities in the ‘Autoimmune profiles see this page for the current criteria (i.e. over 25%).
The specific genus and their interactions determine the symptoms seen — likely due to the over- or under-production of metabolites (chemicals). Other autoimmune conditions may share these core shifts. The specific high and low bacteria determine the symptoms if the person was the DNA/SNP associated with the symptoms.
Replace the metabolites produced by the missing bacteria
Replacing the metabolites should result in the reduction of symptoms associated with a deficiency of these metabolites.
See this post for the study references. These items should/could be done continuously.
- Acetylcholine See this post
- Warning: lots of writing on the web. Some suggestions are contraproductive.
- Regular eating of almonds
- Repeated administration of almonds increases brain acetylcholine levels and enhances memory function in healthy rats while attenuates memory deficits in animal model of amnesia [2016].
- Riboflavin (B2) [1999]
- 400 mg/day [Src]
- Biotin (B7)
- 100 mcg/day [Src]
- Folate (B9)
- 6,000 mcg and 13,000 mcg of Folate, OR
- 15 mg of Folininc Acid [src]
- Vitamin B12
- 1000 mcg/ 1 mg [post]
- GABA
- 1000-3000 mg often cites on various sites
- Up to 0.8g/kg day [Src]
- Urolithins requires bacteria and dietary ellagic acid (pomegranate juice is a source).
- Bifidobacterium probiotics should be taken (at same time) WITH pomegranate juice.
- While the bifido will not stay around, they may utilize the pomegranate during their transit in your body)
- No dosage information.
- Bifidobacterium probiotics should be taken (at same time) WITH pomegranate juice.
Other Supplements Reported to Help
- Vitamin D3 -15,000 IU/day
- “Baseline vitamin D level was found to moderate treatment effect on several outcome measures. Dry mouth and sleep disruption were reported more frequently in the placebo group. [Control took Lactobacillus helveticus and Bifidobacterium longum]” [2017]
- Vitamin D deficiency changes the intestinal microbiome reducing B vitamin production in the gut. The resulting lack of pantothenic acid adversely affects the immune system, producing a “pro-inflammatory” state associated with atherosclerosis and autoimmunity[2016].
- Thiamine Vitamin B1
- 100 mg 2 times a day
- Bacopa monniera and Cognitive Function
- Impacts GABA, acetylcholine
Bootstrapping Bifidobacterium and Lactobacillus
The items below were found in studies to increase bifidobacterium and lactobacillus:
- Almonds/ almond skins: Enhances Bifidobacterium, Lactobacillus
- Sesame seed: Enhances Bifidobacterium Enterococcus Lactobacillus
- Dark Chocolate
- “heparin- or heparosan-treated animals were different from those of the saline-treated animals, with increased Lactobacillus spp. and decreased Enterococcus sp….heparin or heparosan may be used as an effective gut microbiota modulator by increasing the subpopulation of Lactobacillus.” [2013] – Note: Berg’s anticoagulant therapy for CFS used heparin
- “After the intake of apples (2 apples a day for 2 weeks) by eight healthy adult humans, the number of bifidobacteria in feces increased ” [2010]
Unless the bifidobacterium and lactobacillus (B&L) are human sourced, there is almost zero chance of taking up residency. Taking probiotics will not allow B&L to get established. In fact, there are grounds to believe that most commercial probiotics actually reduce your native B&L. You want to encourage your native B&L. See this post for citations.
Bootstrapping E.Coli
The E.Coli probiotics below are human sourced and known to take up residency in the human gut.
- Core: D-Ribose a preferred food that it uses
- Mutaflor probiotics — E.Coli Nissle 1917
- Symbioflor 2 — multiple strains
Dealing with the other microbiome shifts
The other microbiome shifts appear to be in different clusters of microbiome shifts. This 2017 paper by Peterson, Klimas, Komaroff, Lipkin (and a stack of other CFS researchers) makes that clear in its title: “Fecal metagenomic profiles in subgroups of patients with myalgic encephalomyelitis/chronic fatigue syndrome”.
The best way at present to proceed is to order an analysis from uBiome. (Disclosure: I have no financial interest in this company.) When your get your results back, log in, click on the “Compare” tab, then go to “Genus,” and click on “ratio” twice, so the results are in descending order.
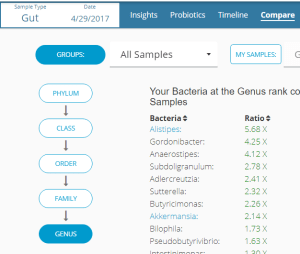
This is the “hit list” of what you are trying to reduce. DataPunk provides a nice summary of what we know about these. See, for example, Alistipes:
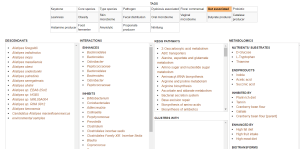
At this point, we run into a logistical challenge. You want to avoid items that are “Enhanced By” (which is in common across all of the high items) and take the items that are “Inhibited By” (which are not on any of the “Enhanced By” lists). You may also wish to reduce foods that are high in items listed in “Nutrients/Substrates.” It becomes a jig-saw puzzle! I have done this exercise for many readers’ uBiome results:
- https://atomic-temporary-42474220.wpcomstaging.com/2017/09/11/ubiomes-before-and-after-a-fecal-microbiota-transplant/
- https://atomic-temporary-42474220.wpcomstaging.com/2017/09/03/ubiome-result/
- https://atomic-temporary-42474220.wpcomstaging.com/2017/09/18/another-ubiome-review-with-bifidobacteria-overgrowth/
- https://atomic-temporary-42474220.wpcomstaging.com/2017/08/27/ubiome-of-a-mcs-with-cfs-person/
I have discovered that DataPunk is not absolutely current, and have started creating posts based on its data, and then added studies from 2016 and 2017 to the page. Past pages are below, for current list MicrobiomePrescription site.
- Acetitomaculum: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/14/decreasing-acetitomaculum-genus
Acetitomaculum (31.02% of Samples) genus - Acidaminococcus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/01/reducing-acidaminococcus-genus
Acidaminococcus (18.52% of Samples) genus - Actinobaculum: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/21/decreasing-actinobaculum-genus
Actinobaculum (4.17% of Samples) genus - Actinomyces: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/25/reducing-actinomyces-genus
Actinomyces (66.2% of Samples) genus - Adlercreutzia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/14/decreasing-adlercreutzia-genus
Adlercreutzia (73.15% of Samples) genus - Akkermansia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/14/decreasing-akkermansia-genus
Akkermansia (71.76% of Samples) genus - Alistipes: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/09/decreasing-alistipes-genus
Alistipes (98.61% of Samples) genus - Anaeroplasma: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/11/decreasing-anaeroplasma-genus
Anaeroplasma (8.33% of Samples) genus - Anaerosinus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/29/reducing-anaerosinus-genus
Anaerosinus (5.56% of Samples) genus - Anaerotruncus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/19/reducing-anaerotruncus-genus
Anaerotruncus (98.15% of Samples) genus - Anaerostipes: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/07/decreasing-anaerostipes-genus
Anaerostipes (100% of Samples) genus - Bacteroides: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/20/decreasing-bacteroides-genus
Bacteroides (100% of Samples) genus - Barnesiella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/15/decreasing-barnesiella-genus
Barnesiella (68.06% of Samples) genus - Bilophila: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/14/decreasing-bilophila-genus
Bilophila (85.65% of Samples) genus - Blautia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/29/reducing-blautia-genus
Blautia (100% of Samples) genus - Brevundimonas: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/04/decreasing-brevundimonas-genus
Brevundimonas (2.31% of Samples) genus - Butyricimonas: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/14/decreasing-butyricimonas-genus
Butyricimonas (66.67% of Samples) genus - Butyrivibrio: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/15/increasing-butyrivibrio-crossotus/
- Caldicoprobacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/15/decreasing-caldicoprobacter-genus
Caldicoprobacter (16.67% of Samples) genus - Candidatus Stoquefichus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/30/reducing-candidatus-stoquefichus-genus
Candidatus Stoquefichus (19.91% of Samples) genus - Catenibacterium: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/18/reducing-catenibacterium-genus
Catenibacterium (46.3% of Samples) genus - Citrobacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/11/reducing-citrobacter-freundii
Citrobacter (6.48% of Samples) genus - Collinsella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/10/decreasing-collinsella-genus
Collinsella (100% of Samples) genus - Collinsella (100% of Samples) genus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/06/decreasing-coprobacter-genus/
- Clostridium : https://atomic-temporary-42474220.wpcomstaging.com/2017/10/07/decreasing-clostridium-genus
Clostridium (100% of Samples) genus - Cronobacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/21/decreasing-cronobacter-genus
Cronobacter (9.72% of Samples) genus - Desulfovibrio: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/decreasing-desulfovibrio-genus
Desulfovibrio (61.11% of Samples) genus - Dialister: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-dialister-genus
Dialister (71.76% of Samples) genus - Dorea : https://atomic-temporary-42474220.wpcomstaging.com/2017/10/18/reducing-dorea-genus
Dorea (100% of Samples) genus - Eggerthella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/19/decreasing-eggerthella-genus
Eggerthella (72.69% of Samples) genus - Eisenbergiella: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/25/reducing-eisenbergiella-genus
Eisenbergiella (68.06% of Samples) genus - Enterococcus: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/29/reducing-enterococcus-genus
Enterococcus (19.44% of Samples) genus - Enterorhabdus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-enterorhabdus-genus
Enterorhabdus (44.44% of Samples) genus - Erysipelatoclostridium: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/14/decreasing-erysipelatoclostridium-genus
Erysipelatoclostridium (100% of Samples) genus - Faecalibacterium: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/11/reducing-faecalibacterium-genus
Faecalibacterium (100% of Samples) genus - Flavobacterium:
https://atomic-temporary-42474220.wpcomstaging.com/2017/12/06/reducing-flavobacterium-genus
Flavobacterium (54.63% of Samples) genus - Flavonifractor: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-flavonifractor-genus
Flavonifractor (100% of Samples) genus - Fusicatenibacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/03/decreasing-fusicatenibacter-genus
Fusicatenibacter (94.91% of Samples) genus - Gelria: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/22/reducing-gelria-genus
Gelria (40.74% of Samples) genus - Gordonibacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/09/decreasing-gordonibacter-genus/ Gordonibacter (61.11% of Samples) genus
- Granulicatella: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/25/reducing-granulicatella-genus
Granulicatella (42.59% of Samples) genus - Haemophilus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/19/reducing-haemophilus-genus
Haemophilus (68.52% of Samples) genus - Herbaspirillum: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/12/reducing-herbaspirillum-genus
Herbaspirillum (44.44% of Samples) genus - Hespellia: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-hespellia-genus
Hespellia (75% of Samples) genus - Hydrogenoanaerobacterium: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/22/reducing-hydrogenoanaerobacterium-genus
Hydrogenoanaerobacterium (45.83% of Samples) genus - Intestinibacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/22/reducing-intestinibacter-genus
Intestinibacter (100% of Samples) genus - Intestinimonas: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-intestinimonas-genus
Intestinimonas (97.69% of Samples) genus - Johnsonella: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/04/decreasing-johnsonella-genus
Johnsonella (1.39% of Samples) genus - Kluyvera: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/31/reducing-kluyvera-genus
Kluyvera (75% of Samples) genus - Lachnospira: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/03/reducing-lachnospira-genus
Lachnospira (96.76% of Samples) genus - Lactonifactor: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/29/reducing-lactonifactor-genus
Lactonifactor (62.04% of Samples) genus - Leuconostoc: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/26/reducing-leuconostoc-genus
Leuconostoc (12.5% of Samples) genus - Marvinbryantia: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/06/decreasing-marvinbryantia-genus/
- Megasphaera: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/18/reducing-megasphaera-genus
Megasphaera (67.59% of Samples) genus - Mitsuokella: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/21/reducing-mitsuokella-genus
Mitsuokella (5.09% of Samples) genus - Moryella: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/11/decreasing-moryella-genus
Moryella (87.5% of Samples) genus - Odoribacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/19/decreasing-odoribacter-genus
Odoribacter (84.26% of Samples) genus - Oscillospira: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/15/decreasing-oscillospira-genus
Oscillospira (87.04% of Samples) genus - Oxalobacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/15/increasing-oxalobacter-formigenes
Oxalobacter (0% of Samples) genus - Papillibacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/06/decreasing-papillibacter-genus
Papillibacter (56.02% of Samples) genus - Parabacteroides: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/17/decreasing-parabacteroides-genus
Parabacteroides (97.22% of Samples) genus - Paraprevotella:https://atomic-temporary-42474220.wpcomstaging.com/2017/11/28/decreasing-paraprevotella-genus
Paraprevotella (29.63% of Samples) genus - Parasutterella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/19/decreasing-parasutterella-genus
Parasutterella (77.31% of Samples) genus - Peptococcus: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/28/decreasing-peptococcus-genus
Peptococcus (59.72% of Samples) genus - Peptoclostridium: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/18/reducing-peptoclostridium-genus
Peptoclostridium (80.09% of Samples) genus - Phascolarctobacterium: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/12/decreasing-phascolarctobacterium-genus
Phascolarctobacterium (68.52% of Samples) genus - Planomicrobium: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/21/decreasing-planomicrobium-genus
Planomicrobium (2.31% of Samples) genus - Prevotella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/14/decreasing-prevotella-genus
Prevotella (59.26% of Samples) genus - Pseudoflavonifractor:https://atomic-temporary-42474220.wpcomstaging.com/2017/11/19/reducing-pseudoflavonifractor-genus
Pseudoflavonifractor (65.28% of Samples) genus - Pseudobutyrivibrio: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/15/decreasing-pseudobutyrivibrio-genus
Pseudobutyrivibrio (100% of Samples) genus - Robinsoniella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/12/decreasing-robinsoniella-genus
Robinsoniella (23.61% of Samples) genus - Romboutsia: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/09/reducing-romboutsia-genus
Romboutsia (52.78% of Samples) genus - Roseburia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/29/decreasing-roseburia-genus
Roseburia (100% of Samples) genus - Rothia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/25/decreasing-rothia-genus/
- Ruminococcus: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/18/reducing-ruminococcus-genus
Ruminococcus (1.39% of Samples) genus - Sarcina: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/12/decreasing-sarcina-genus
Sarcina (100% of Samples) genus - Senegalimassilia: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/18/reducing-senegalemassilia-genus
Senegalimassilia (29.17% of Samples) genus - Shuttleworthia: https://atomic-temporary-42474220.wpcomstaging.com/2017/12/22/reducing-shuttleworthia-genus
Shuttleworthia (36.11% of Samples) genus - Slackia: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/15/decreasing-slackia-genus
Slackia (40.74% of Samples) genus - Streptococcus: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/25/reducing-streptococcus-genus/
- Subdoligranulum: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/10/decreasing-subdoligranlum/
- Succinivibrio: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/decreasing-succinivibrio-genus
Succinivibrio (1.39% of Samples) genus - Sutterella: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/13/decreasing-sutterella-genus
Sutterella (70.37% of Samples) genus - Terrisporobacter: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/05/reducing-terrisporobacter-genus
Terrisporobacter (81.48% of Samples) genus - Thalassospira: https://atomic-temporary-42474220.wpcomstaging.com/2017/10/22/reducing-thalassospira-genus
Thalassospira (55.56% of Samples) genus - Veillonella: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/29/reducing-veillonella-genus
Veillonella (68.52% of Samples) genus - Victivallis: https://atomic-temporary-42474220.wpcomstaging.com/2017/11/11/decreasing-victivallis-genus
Victivallis (46.76% of Samples) genus
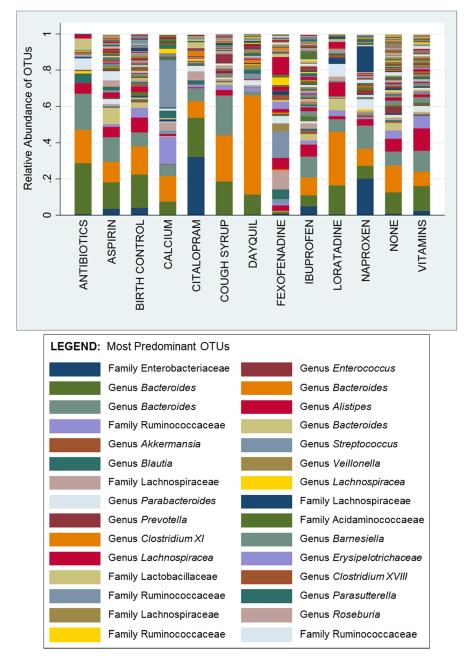
Src: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4754147/
General Suggestions (no uBiome results)
Some of these items are contraindicated with a few uBiomes that I have reviewed. This likely is why person B reports no results while person A reports improvement. Example: Magnesium is usually very helpful — but there are a few cases where it encourages overgrowth of undesired bacteria.
Probiotics
Most probiotics do not take up residency. They are “here today, gone tomorrow”. Their primary role in my model is producing natural antibiotics against other bacteria. For example:
- Inhibition of Clostridium perfringens by an antibiotic substance produced by Bacillus licheniformisin the digestive tract of gnotobiotic mice: effect on other bacteria from the digestive tract [1976].
- “Among those, seven Paenibacillus polymyxa strains showed the highest antibotulinal activity and the largest antimicrobial spectrum against C. botulinum strains. ” [2002] – this is in Prescript Assist Probiotics
Probiotics should be rotated: 2 weeks on a specific one, then several weeks off. As a general rule, you want about 6-12 B CFU taken three times a day (or 2-3 times the recommended dosage) — but work up slowly because you may get be a major herx! In general, do not take Lactobacillus with Bifidobacteria or with E.Coli etc. Keep to one family per cycle. You do not want them to kill off one another!
Why 3x per day? Because almost none of them are detected after 12-24 hrs. So to keep them — and the production of natural antibiotics — going, you need to keep taking them during the day. See this post for citations.
The following probiotics commonly seem to help people with CFS/Lyme/Fibro:
- Symbioflor-2
- Mutaflor
- Lactobacillus Fermentum ME3
- Lactobacillus Kefiri LKF01
- Lactobacillus Reuteri
- Lactobacillus Casei
- Bifidobacterium infantis
- Bifidobacterium Longum
- Bifidobacterium bifidum
- Bifidobacterium Breve
- Prescript Assist
- General Biotics Equilibrium
Some probiotics, however, may make your symptoms worse! And, unfortunately, most commercial probiotics contains some of these. At the moment Bifidobacterium animalis, Saccharomyces boulardii and Lactobacillus acidophilus are on my best to totally avoid list.
- “. The findings show that the six species of Bifidobacterium differed in their ability to relieve constipation. B. longum, B. infantis and B. bifidum were the most effective in relieving constipation, B. adolescentis and B. breve were partially effective and B. animalis was not effective. Furthermore, edible Bifidobacterium treated constipation by increasing the abundance of Lactobacillus and decreasing the abundance of Alistipes, Odoribacter and Clostridium. .” [2017]
On my neutral list (no clear benefit) is Lactobacillus Plantarum.
Teas
Some teas can also be antibiotics (among other roles). There are two teas that seem to produce significant results quickly:
- Rosehip Tea
- Tulsi Tea
Again, rotate and, if practical, change brands too. Their antibiotic compounds are different from different sources.
Herbs and Spices
The best choice needs examination of your microbiome (i.e. uBiome results) and doing the work cited above. Survey results found:
- Neem and Oregano with 80% improving
- Olive Leaf and Licorice with 56% improving
- Thyme with 50% improving
- Wormwood and Tulsi with 33% improving
Other things
If you do not know your microbiome, then see https://atomic-temporary-42474220.wpcomstaging.com/reader-surveys-of-probiotics-herbs-etc/ for suggestions. Your results will vary because your microbiome vary.
Thick blood is an issue also — but here things gets more complicated and not suitable for this recap.
Antibiotics can have a role — but getting prescriptions for the right ones can be a major challenge.
Metabolism Shifts
From volunteered data, we can identify some distinctive shifts, see Metabolism Explorer Summary
Bottom Line
Working with the microbiome and autoimmune is like working with fragments of the dead sea scrolls. For many bacteria we can identify it — what inhibits or encourages it is not known to modern medical science. We have extremely thin slices of knowledge –Almonds enhances Bifidobacterium, Lactobacillus (B&L) as do sesame seeds. What about sunflower seeds? Peanuts? Cashews? We find that Walnuts help the bacteria that inhibits B&L — so we cannot safely generalize to “all seeds/nuts are helpful”.
In many cases, we find that healthy diet or supplements demonstrated to work for normal people have the opposite effect on CFS and other altered microbiome conditions. This is made even worst because most of the studies were done on males and most people with CFS are females. We end up having to swim up-stream thru good and valid suggestions — that are just wrong for us.
My model is simple to understand and allows us to filter many suggestions and candidates. With the availability of uBiome testing (without needing a prescription!) we have entered the age of explicit treatment based on your unique microbiome. We do not know the role of many bacteria involved. We do not know what will inhibit or enhanced all of these bacteria. Frustrating little knowledge!
On the flip side, many readers have reported significant improvement, reduction of prescription medication, etc. so the model and suggestions have potential and thus hope of remission! Microbiome studies are exploding on PubMed, a lot of research is being done and we can often borrow their results.
This is an education post to facilitate discussing this approach with your medical professionals. It is not medical advice for the treatment of any medical condition. Always consult with your medical professional before doing any changes of diet, supplements or activity. Some items cites may interfere with prescription medicines.